Living With Lupus: In What Ways Can Lupus Affect the Body?
Contents:
Living With Lupus: How Can Lupus Affect the Body?
Lupus Effect on the Body: A Head to Toe Listing
Living With Lupus: How Can Lupus Affect the Body?
In Lupus and other autoimmune diseases, the immune system begins to recognize and attack itself, going after and injuring healthy tissue. This can cause several complications as well as inflammation throughout the body’s various systems. Because lupus can affect nearly every part of your anatomy, it is a difficult disease to diagnose, predict the progress of, and treat. There are several emotional ramifications when coping with lupus, which is discussed in more detail in our blog, Coping With Lupus:How does lupus affect your state of mind and body? For the purposes of this blog, we will focus specifically on the physical ramifications that may occur in the body affected by lupus. It is also quite common to have lupus in combination with other connective tissue or autoimmune diseases. When this occurs, it is often called an overlap disease. This is one of the main reasons that lupus can be so difficult to diagnose and, all too often, misdiagnosed. *It is important to note that no two lupus patients are alike. While some may get certain symptoms of lupus, others will not get those same symptoms. Developing a strong relationship with your doctor is vital so that you may work together to create the most effective treatment plan specific to your needs. Back to top
Lupus Effect on the Body: A Head to Toe Listing
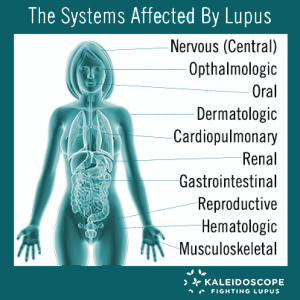 Brain and Nervous System: People with lupus often experience signs associated with the body’s brain and nervous system. This can affect both the central nervous system (brain and spinal cord) and the peripheral nervous system. Complications from this can cause headaches, depression, mood swings, cognitive dysfunction (brain fog), stroke and seizures. Many of these symptoms can be successfully treated and/or managed with medication.
Brain and Nervous System: People with lupus often experience signs associated with the body’s brain and nervous system. This can affect both the central nervous system (brain and spinal cord) and the peripheral nervous system. Complications from this can cause headaches, depression, mood swings, cognitive dysfunction (brain fog), stroke and seizures. Many of these symptoms can be successfully treated and/or managed with medication.
Opthalmologic (The Eyes): The eye complications that can occur include; dry eye, blocked tear ducts, cataracts, blurred vision, impaired vision or even vision loss. These can be related to the inflammatory process of lupus itself but in other cases, problems may be due to drug treatment (corticosteroids or antimalarials) or may be a separate problem (glaucoma or retinal detachment). It is very important to schedule annual comprehensive eye exams to catch and treat any issues that may come about.
Dermatologic (The Skin): There are three major types of skin disease specific to lupus: Discoid Lupus, Subacute Cutaneous Lupus and Acute Cutaneous Lupus. For more information on this topic, please read our blog on the butterfly rash and other rashes. Approximately two-thirds of people living with lupus will develop some type of skin disease or cutaneous lupus. Rashes and sores are a common complication of lupus. Up to 70 percent of lupus sufferers have photosensitivity (sensitive to ultraviolet, UV, light.) Some tips on mitigating the negative effects of lupus on the skin are:
- Avoiding direct exposure to sunlight or even some fluorescent light
- Stay out of the sun during the most intense times of the day, 10am-3pm
- Stay covered when out in the sun by wearing a wide brimmed hat, long-sleeved clothing and long pants
- Wearing sunscreen that has SPF of thirty or above
Hematologic (The Blood): Approximately 50 percent of lupus patients with active lupus have anemia (too little hemoglobin, a protein that moves oxygen throughout the body). Still others can develop leukopenia (an abnormally low level of white blood cells) or thrombocytopenia (decreased number of platelets that aid in blood clotting) or thrombosis which can cause very dangerous blood clots.
The Cardiopulmonary System: This includes your heart and lungs. A very important point to note- cardiovascular disease (heart disease), a common symptom of lupus, is the number one cause of death in people with SLE. About 50% of people with SLE will experience lung involvement during the course of their disease. Five main lung problems occur in lupus:
- Pleuritis (inflammation of the membrane lining of the lungs)
- Acute Lupus Pneumonitis
- Chronic (fibrotic) Lupus Pneumonitis
- Pulmonary Hypertension
- “Shrinking Lung” Syndrome.
Pleuritis is the most common of these, causing sharp, stabbing pains in your chest upon breathing deeply, coughing, sneezing, or even laughing.Therefore, the proper monitoring and maintenance of optimal cardiovascular health is essential for those with lupus.
The Renal System (Kidney): It is estimated that as many as *40 percent of all people with lupus, and as many as two-thirds of all children with lupus, will develop kidney complications that require medical evaluation and treatment. This is called lupus nephritis. If you experience swelling in your feet, legs, fingers, or eyes; blood in your urine or increased frequency in urination especially during the night, it could signify inflammation in your kidneys that, if not treated, can lead to kidney damage and kidney disease. The kidney is the most extensively studied organ that is affected by lupus.
The Gastrointestinal System (GI system): GI system complications and problems from the esophagus to the intestines are a common occurrence in lupus patients. This can include the surrounding organs such as the stomach, liver, pancreas, bile ducts, and the gallbladder. Often the muscles aren’t able to effectively move waste through the intestines causing many of these digestive problems.
The Musculoskeletal System: More than 90 percent of people with SLE will experience joint and/or muscle pain at some time during the course of their illness. Inflammation of the joints and muscles is the most common cause for this complication. Lupus Arthritis is recognized as pain, stiffness, swelling and a feeling of warming in your joints. The arthritis seen in lupus closely resembles rheumatoid arthritis (read more about “overlap” diseases below.) Although pharmaceutical medications are available for pain management, many patients find relief in natural remedies like moist heat, baths, showers, acupuncture, yoga, and chiropractic care.
The Bones: The use of corticosteroid medication often prescribed to treat SLE can increase the risk for, and even trigger, significant bone loss or osteoporosis. Getting enough calcium and vitamin D in your diet, regular exercise, and avoiding smoking can help combat the severity of any osteoporosis that may develop.
Oral Disease in Lupus: Approximately 95 percent of lupus patients suffer from some form of oral complications such as the development of sores and lesions inside the mouth or nose. Canker sores can also become more prevalent. Topical steroids are often prescribed and can help alleviate these problems. 
Reproductive System: Pregnancy with lupus has always been considered “high-risk” due to the potential for an increased possibility of miscarriage or premature delivery. However, it is important to know that many women with lupus, receiving the proper monitoring and care of a physician, go on to deliver normal, healthy babies! Back to top
In Conclusion
While lupus is a lifelong disorder of the immune system with as of yet, no cure, there are treatments that can minimize the damage that lupus causes to the body. Increased education among the medical community and the public are leading to earlier diagnosis and strides are being made in the discovery of new lupus treatments which will, one day, lead to a cure. Please join us in our mission to raise awareness for and help those who are living with lupus by sharing and commenting on this blog. And don’t forget- our newest blogs go out on the second and fourth Wednesday of every month. Back to top
Author: Karrie Sundbom
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

