Lupus and Biomarkers
Talking about “biomarkers” may not sound exciting, or even particularly interesting, yet they are absolutely critical to both diagnosing lupus and improving treatment plans for patients. They are also vitally important tools that scientists use in their search for a cure, and the future of biomarkers is a bright one for those living with lupus! Read on to find out more.
- A Brief Introduction to Biomarkers
- Lupus Biomarkers
- The Future of Biomarkers is Bright!
- In Conclusion
.
A Brief Introduction to Biomarkers
What are biomarkers?
The word “biomarker” is actually short for the term, “biological marker.” So, what does that mean? Technically, a biomarker is any measurement of your body’s biological activity – basically any measurement of your health.
Examples of biomarkers range from the straightforward measurements that have been been a part of medicine for centuries, like pulse rate, breathing rate, temperature and blood pressure to the sophisticated lab tests that are used today.
.
There are four types of biomarkers:
- Physiologic, such as blood pressure and heart rate;
- Histological, which include biopsy results;
- Radiographic, such as x-rays and CT scans, and
- Molecular, which include all of the chemicals measured with blood and urine tests.
.
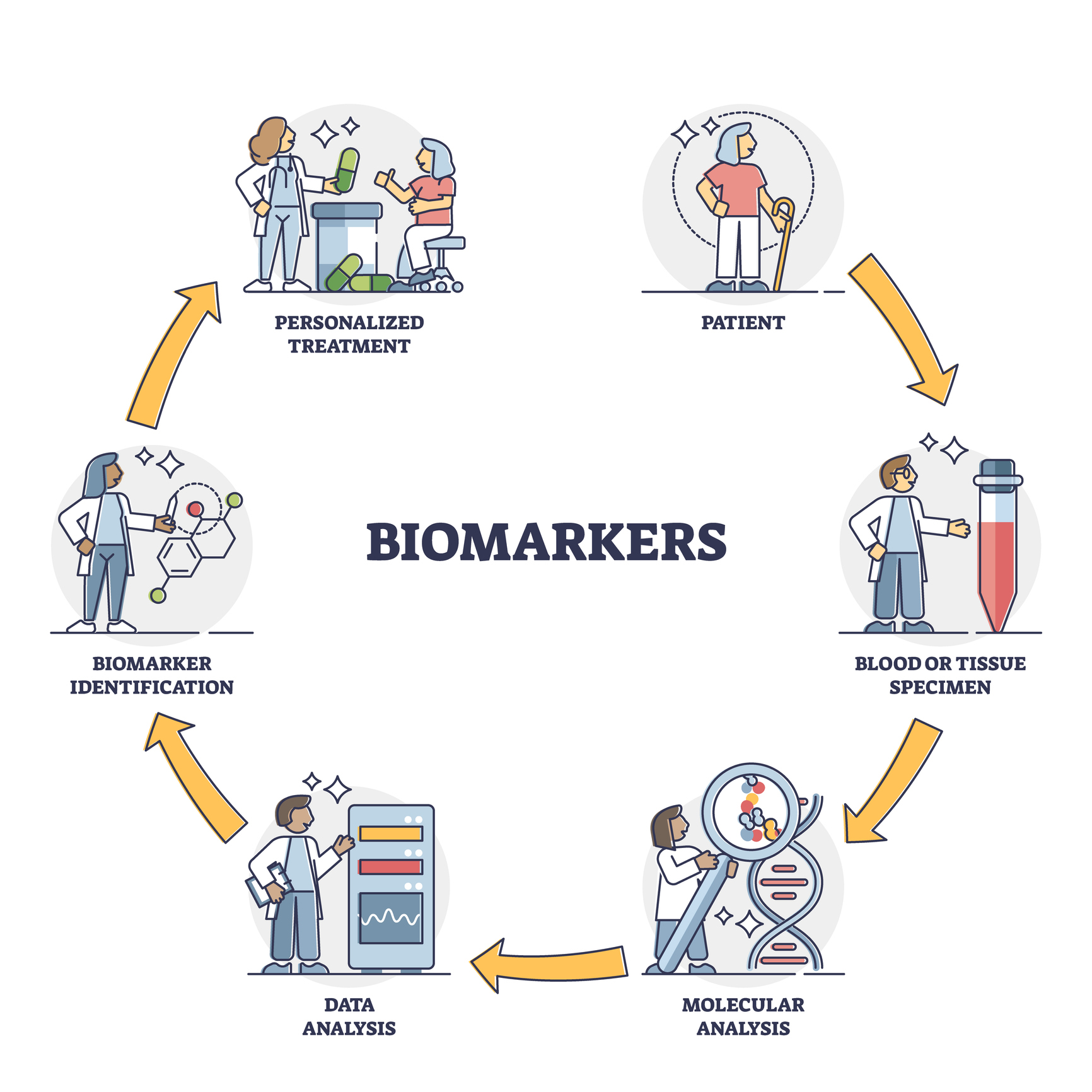
Basically, any number that comes from a lab test is the measurement of a biomarker. A common example is blood glucose, which is a biomarker for diagnosing and managing diabetes. Glucose is an incredibly useful biomarker for diabetes because the test is very accurate, and it requires a relatively simple procedure that patients can do on their own.
Unfortunately, there is no truly similar biomarkers that can be used for lupus … and that has made discovering SLE biomarkers an important focus of current research labs around the globe.
.
A Few More Things You Should Know About the Importance of Biomarkers:
- Biomarkers can identify conditions that may be invisible to both the physician and even the patient. This makes it possible to discover a condition, like a lupus flair, even when the patient does not feel any symptoms. A good example are the protein biomarkers, which if detected in urine, may indicate kidney damage from lupus nephritis (LN). Without those biomarkers, LN can begin its damage with no noticeable symptoms!
- Biomarkers allow healthcare professionals to measure even small changes in a patient’s condition, and that makes it possible to see patterns and trends over time … and that means treatment plans can be changed and improved.
- Biomarkers make it easier for healthcare professionals to communicate a patient’s condition with each other – and to compare test results with those of other patients. This is a critical aspect of medicine that is often overlooked!
Yet, there are also some cautionary things to keep in mind about biomarkers:
- If a patient’s blood tests – their biomarkers – do not reflect how they are feeling, it can be challenging to convince others that what they are feeling is real! Have you ever felt bad even when your labs seem to be just fine … or vice versa?
- Some biomarker tests are not as reliable as others. That can make test results seem confusing. Make sure you understand what those lab results really mean!
- Another issue is that many biomarkers are indirect indicators of disease. Meaning, they may not perfectly correspond to a specific condition. Several blood and urine biomarkers used for lupus only indirectly measure possible kidney involvement caused by LN. That is why biopsies are sometimes required in order to get direct evidence of renal damage.
So, what makes a good biomarker? It requires the balance of two aspects that affect the accuracy of all lab tests: biomarker sensitivity and specificity.
Sensitivity: A highly sensitive biomarker test is one that reliably gives a positive result when a person actually has a disease. This makes it possible to diagnose a condition both quickly and early in the course of the disease. That is a very good thing! Unfortunately, highly sensitive tests can also bring up “false positives” if other, similar conditions also have the same biomarker.
Specificity: A test that is highly specific means that it uses a biomarker that will only diagnose a specific disease or condition – ignoring everything else. This can reduce “false positive” results, but also may lead to “false negatives” – when the disease is missed.
Unfortunately, finding a biomarker that is both highly sensitive and highly specific for lupus is very difficult – but there are things that physicians can do!
Biomarkers and Lupus
Lupus is challenging because it affects each person in so many different ways. So, at least for now, there is no single biomarker or test that can definitively diagnose lupus. That is why rheumatologists test for a combination of several biomarker over a long period of time in order to make a lupus diagnosis.
Also, since lupus can change dramatically over time – from full-scale flaring, to low disease state, or perhaps even remission – lupus patients have to undergo A LOT of testing. Each biomarker targets a different aspect of lupus and they need to be taken together to get a handle on the patient’s overall disease state.
Historically, lupus biomarkers were limited to blood antibodies and complement protein levels to measure the autoimmune activity … or testing the amount of cytokines in the blood. Cytokines are a group of chemicals that the immune system uses to coordinate the inflammatory response, so measuring these biomarkers can indicate the intensity a patient’s inflammatory response.
Currently, there are too many lupus biomarkers to describe in this article. However, here is a short list of some of the most important and interesting ones.
- Anti-nuclear Antibodies (ANA’s): These biomarkers are found in the blood and indicate how much the body is attacking its own tissues in general. For years, it has been one of the most commonly used biomarker in diagnosing SLE because it is highly sensitive, meaning that over 90% of those with lupus will test positive for ANA’s. Yet they are not specific some people without lupus will show positive ANAs.
- Complement 3 (C3) and Complement 4 (C4): Low levels of both of these biomarkers combined with positive ANA tests are 95% specific for an SLE diagnosis!
- Anti-dsDNA Antibodies: These biomarkers are found in blood serum and are both associated with SLE and used to help predict the development of lupus nephritis.
- Erythrocyte Sedimentation Rate (ESR or “sed rate”): This test measures how quickly red blood cells separate from the serum of your blood in a special tube. High ESR values are an indicator of inflammation in lupus.
- C-Reactive Protein (CRP): Low CRP levels are also a key sign of inflammation in SLE and together with ESRs are used for monitoring lupus disease activity.
- Protein/Creatinine Ratio: This tests the levels of two biomarkers in the urine, protein and creatinine. The relative levels of these chemicals can indicate kidney damage in lupus nephritis patients and help determine whether a kidney biopsy may be needed to confirm a diagnosis.
- Anti–SSA Antibodies: These are commonly used skin biomarkers for diagnosing subacute cutaneous lupus.
- Monocyte–to-High-Density Lipoprotein Cholesterol Ratio: This biomarker, with a very long name, is important in identifying the risk of cardiovascular disease in SLE patients.
.

.
The Future of Biomarkers is Bright!
The great news is that every year, new biomarkers for lupus are found and developed … and the list is likely to grow dramatically as the technology to develop them improves. For example, using combinations of different biomarkers, it may be possible to not only accurately diagnose different types lupus nephritis from a simple urine test, but even predict who might be most at risk for developing nephritis. This way, damage might be prevented before it even begins!
Additionally, every time a new biomarker for SLE is found, it reveals yet another possible immunological process that may one day lead to finding fundamental causes for lupus … and that will lead to more individualized treatments … and that will hopefully lead to possible cures!
The future is bright!
.
In Conclusion
The search for better biomarkers is one of the most important areas of lupus research today. Short of finding a cure, discovering biomarkers that are both very specific and highly sensitive would significantly improve the lives of those living with lupus:
- Making a lupus diagnosis quicker and more accurate.
- Making it easier to monitor how treatments are working … or not working.
- Improving the ability of physicians and patients to monitor their disease state and perhaps reduce some of the uncertainty that comes with living with lupus.
- Ultimately, guiding future research to an ultimate cure.
Remember this the next time you look over your lab test results. Each represents a biomarker – a small piece of a very complex puzzle – that can help you and your healthcare team best manage your lupus.
.
References
Capecchi, R., Puxeddu, I., Pratesi, F., & Migliorini, P. (2020). New biomarkers in SLE: From bench to bedside. Rheumatology, 59(5). 12-18. https://doi.org/10.1093/rheumatology/keaa484
Collins, T. (2020, January 17). Emerging biomarkers for lupus. The Rheumatologist. https://www.the-rheumatologist.org/article/emerging-biomarkers-for-lupus/
Jacobs, S. (2022, June 21). Novel biomarkers for diagnosing systemic lupus erythematosus detected in plasma. Rheumatology Advisor. https://www.rheumatologyadvisor.com/home/topics/systemic-lupus-erythematosus/novel-biomarkers-for-diagnosing-systemic-lupus-erythematosus-detected-in-plasma/
Karakonstantis, S. & Kaemaki, D. (2023, June 18). The common pitfall in studies of biomarkers for diagnosing infections in patients with systemic lupus erythematosus. Open Access Text. https://www.oatext.com/the-common-pitfall-in-studies-of-biomarkers-for-diagnosing-infections-in-patients-with-systemic-lupus-erythematosus.php
Kim, H-A., Jung, J-Y, & Suh, C-H. (2015). Biomarkers for systemic lupus erythematosus: An update.International Journal of Clinical Rheumatology, 10(3), 195-204. https://www.openaccessjournals.com/articles/biomarkers-for-systemic-lupus-erythematosus-an-update.pdf
Strimbu, K. & Tavel, J.A. (2010). What are biomarkers? Current Opinions in HIV AIDS, 5(6), 463-466. DOI:10.1097/COH.0b013e32833ed177
Yu, H., Nagafuchi, Y., & Fujio, K. (2021). Clinical and immunological biomarkers for systemic lupus erythematosus. Biomolecules, 11(7). 928. DOI:10.3390/biom11070928
.
Author: Greg Dardis, MS
Professor Dardis was the Chair of the Science Department at Marylhurst University and is currently an Assistant Professor at Portland State University. His focus has been human biology and physiology with an interest in autoimmunity. Professor Dardis is also a former President of the Board of Directors of Kaleidoscope Fighting Lupus.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

