Lupus and the Air You Breathe
There is nothing quite like a breath of fresh air … for a multitude of reasons. Yet, polluted air can hold the potential for triggering the immune system in a negative way with every breath. What can this mean for those living with lupus? Read on to find out!
Introduction
Air pollution of any kind can have a profound influence on individuals living with lupus … and that includes both outdoor pollution and poor indoor air quality! How? Pollutants that reach the lungs can worsen lupus symptoms, trigger flares and even affect a person’s long-term disease outcomes.
With each breath, smoke, pollen and other particulates, as well as ozone, and other chemical pollutants, can reach the lungs and cause the body to react – or over-react in the case of lupus.
Avoiding poor air quality can be easier said than done. However, understanding where pollutant exposure might take place, observing their effects on your own immune system and then taking steps to reduce your exposure can make all the difference! This is where the latest science and research (below) can help.
.
Lupus, The Air and Your Lungs
Lupus and the Lungs
There are two ways in which lupus and the lungs can affect each other:
First, lupus can attack a person’s lungs, just like it can damage any other tissue or organ of the body. To learn more about the science behind this, check out KFL’s article, “Lupus and the Lungs” here.
Second, the lungs can affect a person’s lupus – if it becomes a gateway for chemicals and other environmental factors that trigger inflammation or the autoimmune response.
From a physiological point of view, the lungs are the most sensitive and fragile part of the body that encounters the external environment. It has to be so delicate and exposed to the air in order to get the incredible amounts of oxygen and carbon dioxide in and out of the blood stream necessary to keep you alive.
This also means that the lungs are also the easiest way for pollutants to enter the body. Not to make you overly self conscious, but with every breath, your lungs can allow any number of possible pollutants with direct access to your blood stream. In the case of larger particulates, they might not enter the blood directly, but could get stuck in the delicate air sacs and cause physical damage to lung tissue.
Either way, these pollutants can be recognized by wandering white blood cells and become the target of the immune response … which could lead to an auto-immune response and end up the triggering a lupus flare.
What are the most important pollutants to think about?
Air Pollutants That Can Trigger Lupus
The most common airborne triggers for those living with lupus include: particular matter, like smoke, pollen and dust, and chemical pollutants, like ozone, nitrogen oxides, sulfur dioxide and volatile hydrocarbons / smog.
Particulate Matter (PM):
These microscopic particles suspended in the air, pose a significant threat to individuals with lupus. They often come from vehicle exhaust, industrial emissions, and wildfires, and can penetrate deep into the lungs, enter the bloodstream and trigger systemic inflammation – even for individuals without lupus.
For lupus patients, whose immune systems are already over-reactive, exposure to particulates can further disrupt immune function and exacerbate disease activity. Several studies have linked elevated levels of PM to increased disease flares, worsened symptoms, and greater disease severity in lupus patients. One study in Brazil found that children with SLE showed an increase in lupus symptoms 12 to 15 days after exposure to increased particulate matter.
Pollen and dust are examples of particulate matter that additionally can cause allergic reactions that may also be more intense for those living with lupus.
Chemical Pollutants
Ozone (O3), is a key component of smog, and another air pollutant with detrimental effects on lupus patients. Ozone exposure can create what is called oxidative stress that increases inflammation in the body, exacerbating existing symptoms and triggering flares.
For individuals with lupus, particularly those with skin involvement, ozone exposure can worsen dermatological manifestations such as rashes and photosensitivity. Additionally, ozone can impair lung function, leading to respiratory symptoms and complications in lupus patients who have underlying lung involvement.
Nitrogen dioxide (NO2) and sulfur dioxide (SO2), have also been tied to worse lupus symptoms. These pollutants are produced from industrial processes: SO2 is especially common in pollution from coal and oil power plants, while NO2 is more common in vehicle emissions. Both pollutants can irritate the respiratory system, trigger asthma attacks, and worsen respiratory symptoms in lupus patients.
One study showed that every 10% increase in SO2 concentrations produced a 2% increase in the hospitalization of rheumatic diseases, including lupus.
In a 2024 British study, NO2 was a particular trigger for patients who also had high “polygenic risk scores” – a genetic predisposition for lupus.
Additionally, exposure to NO2 and SO2 can contribute to cardiovascular complications, increasing the risk of heart disease and stroke, which are already higher in individuals with lupus.
 .
.
Exposure to air pollution can further heighten this risk by promoting atherosclerosis, hypertension, and other cardiovascular risk factors. Similarly, lupus patients with kidney involvement may experience worsened renal function and disease progression due to the systemic effects of air pollution on inflammation and oxidative stress.
Finally, air pollution can even impact mental health, further increasing stress and anxiety, which may in turn worsen lupus symptoms and trigger flares. The psychological and social impacts of living in areas with poor air quality can seriously affect a person’s overall well-being and quality of life!
Many countries around the world have defined air quality in many ways. In the United States, the Environmental Protection Agency developed the Air Quality Index below. In general, those living with lupus are considered “sensitive groups” and can expect to feel the effects from the AQ numerical values over 101.
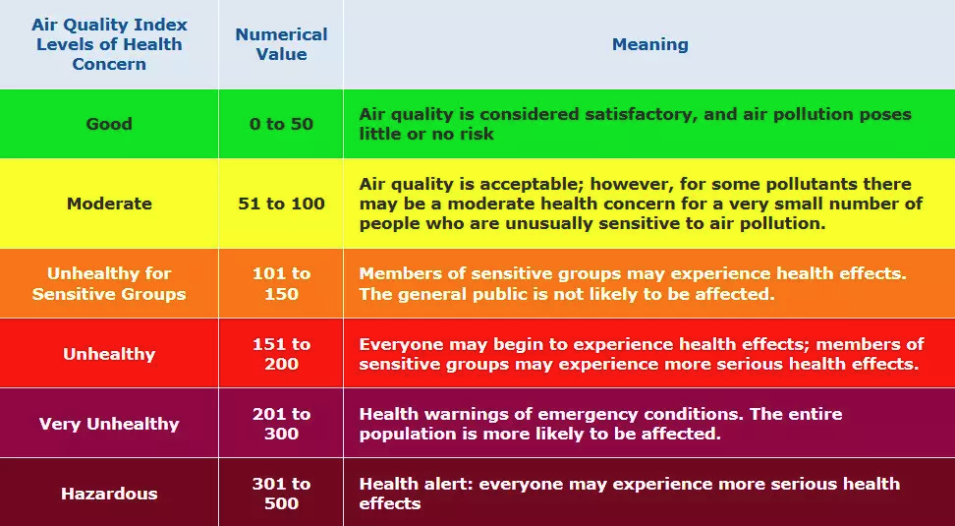
Courtesy of the EPA
.
So, what can you do?
If possible, avoid unnecessary exposure to air pollution. When outside:
- Monitor local air quality and avoid going outside during the most polluted times of the day.
- Avoid prolonged or heavy exertion outdoors or reschedule activities for a better day.
- If outdoor air quality is particularly unhealthy, find an indoor location with clean, filtered air, like a shopping mall, library or community center.
- Staying hydrated can also help prevent irritation of airways by smoke.
When indoors:
- Keep doors and windows closed during unhealthy air quality days, and set air conditioning systems to “re-circulate” to prevent bringing dirty air from outside.
- Invest in HEPA air purifying equipment.
- Avoid using aerosols, hairspray, paint or volatile glues indoors.
- Wear N-85 respiratory masks if particulate air pollution is unavoidable.
.

.
In Conclusion
Air quality and pollution can have a significant influence on individuals living with lupus, exacerbating symptoms, triggering flares, and potentially worsening disease outcomes. There are many types of air pollutants – from both indoor and outdoor sources. For those It is truly important to identify these sources and reduce your exposure to them.
.
References
Bai, H., Jiang, L., Li, T., Liu, C., Zuo, X., Liu, Y., Hu, S., Sun, L., Zhang, M., Lin, J., Xiao, W., Wang, Q., Zhao, D., Wu, H., Kong, X., Gao, W., Hou, W., Seong, M., Zhang, Y., Chen, F., Chen, S., Wu, X., Bao, C., Wang, Li, & Xu, H. (2021). Acute effects of air pollution on lupus nephritis in patients with systemic lupus erythematosus: A multicenter panel study in China, Environmental Research, 195, 110875, https://doi.org/10.1016/j.envres.2021.110875.
Blaskievicz, P. H., Silva, A. M. C., Fernandes, V., Junior, O. B. P., Shimoya-Bittencourt, W., Ferreira, S. M. B., & da Silva, C. A. L. (2020). Atmospheric pollution exposure increases disease activity of systemic lupus erythematosus. International Journal of Environmental Research and Public Health, 17(6), 1984. https://doi.org/10.3390/ijerph17061984
Gilcrease, G. W., Padovan, D., Heffler, E., Peano, C., Massaglia, S., Roccatello, D., Radin, M., Cuadrado, M. J., & Sciascia, S. (2020). Is air pollution affecting the disease activity in patients with systemic lupus erythematosus? State of the art and a systematic literature review. European Journal of Rheumatology, 7(1), 31–34. https://doi.org/10.5152/eurjrheum.2019.19141
Cakmak, S, Blanco-Vidal, C., Lukina, A.O., & Dales, R. (2021). The association between air pollution and hospitalization for patients with systemic lupus erythematosus in Chile: A daily time series analysis, Environmental Research, 192, 110469. https://doi.org/10.1016/j.envres.2020.110469.
Chen, J., Qu, W., Sun, L., Chen, J.C., Kong, W., Wang, F., Pan, W., Liu, L., Wu, M., Ding, F., Hu, H., Ding, X., Wei, H., Zou, Y., & Sun, L. (2021). The relationship of polluted air and drinking water sources with the prevalence of systemic lupus erythematosus: a provincial population-based study. Science Reports,11, 18591. https://doi.org/10.1038/s41598-021-98111-8
Rezayat, A.A., Niloufar, J., Nourbakhsh, S.H., Hoseini, F.S.H., Hooshman, N., Nour, M.G., Handjani, F., & Tabirizi, R. (2022). The effect of air pollution on systemic lupus erythematosus: A systematic review and meta-analysis. Lupus, 31(13):1606-1618. doi:10.1177/09612033221127569
Xing, M., Ma, Y., Cui, F., Li, D., Wang, J., Tang, L., Zheng, L., Yang, J. & Tian, Y. (2024). Air pollution, genetic susceptibility, and risk of incident systemic lupus erythematosus: A prospective cohort study. Arthritis & Rheumatology. https://doi.org/10.1002/art.42929
Yariwake, V.Y., Torres, J.I., dos Santos, A.R.P. et al. (2021). Chronic exposure to PM2.5 aggravates SLE manifestations in lupus-prone mice. Particulate and Fibre Toxicology, 18 (15). https://doi.org/10.1186/s12989-021-00407-0
.
Author: Greg Dardis, MS
Professor Dardis was formerly the Chair of the Science Department at Marylhurst University and is currently an Assistant Professor at Portland State University and the American College of Healthcare Sciences. His focus has been human biology and physiology with an interest in autoimmunity. Professor Dardis is also a former President of the Board of Directors of Kaleidoscope Fighting Lupus.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

