Lupus and the Skin Microbiome
Your skin is amazing! It is your first line of defense against foreign germs, yet simultaneously, an incredibly complex ecosystem of bacteria, fungi and more that make up your skin’s natural microbiome. It is also where lupus can make its most obvious appearance – with rashes, sores, alopecia and even scaring. So, how do lupus and your skin’s microbiome influence each other and affect your overall health? Read on to find out!
- The 1-minute Overview
- More on the Skin Microbiome
- Lupus and the Skin Microbiome
- So what can you do to maintain a healthy microbiome with lupus?
- In Conclusion
.
The 1-minute Overview
Your skin is your largest organ, your first line of defense against threats from the environment and a complex ecosystem harboring millions upon millions of bacteria, fungi, viruses and other microorganisms – your skin’s microbiome. Most of the time, these organisms live on the skin’s surface in a delicate balance that usually benefits you. Bacteria, in particular, play a huge role in this balance and they are an important component of your skin’s health … until they aren’t.
Lupus, of course, commonly affects the skin as well. As an overly aggressive immune response, it can attack the skin from the inside causing rashes, lesions, photosensitivity and sometimes scarring or hair loss.
Lately, research has begun to reveal the hidden relationship between the skin’s microbiome and lupus. In short, those with SLE tend to have a significantly different mix of bacteria than those who do not have lupus. Technically, the term for this is dysbiosis, an unhealthy imbalance in your skin’s microbiome. Yet, what does that mean? Can skin bacteria trigger flares or perhaps cause lupus? Does lupus directly affect a person’s skin microbiome?
There are still few definitive answers to these questions. However, here are some facts that we do know:
- Those with lupus tend to have fewer kinds of skin bacteria – a less diverse microbiome – than healthy individuals.
- Often, the less diverse and populated their microbiome, the more intense is the experience of lupus symptoms for those with SLE.
- Some bacteria, like Staphylococcus aureus, seem to be more prevalent on those with lupus.
- Certain cells of your immune system and some of the bacteria on your skin can actually cooperate to protect each other from invading bacteria.
- Unfortunately, bacterial infections of the skin can induce SLE by triggering an immune response.
- “Staph” is the leading type of infection for people with lupus.
Normally, there is a healthy balance – a homeostasis – that is maintained between your immune system and the native bacteria of your skin. It is still unclear how lupus might disrupt this balance or whether skin bacteria can actually cause lupus. However, learning a bit more about this complex relationship may give you an advantage in managing your lupus.

.
More on the Skin Microbiome
The skin’s major role is to be a physical barrier – protecting our bodies from infections and injury from external threats. Yet, it has to remain flexible and adapt to changing environments. It houses a surprising number of sensory nerves and glands that secrete substances like sweat and oils. It is also affected by hormones, such as the increase in acne during puberty, or by emotions, as when a person is embarrassed, their cheeks tend to flush red.
When it comes to the microbiome, it is also helpful to think of the skin as a complex ecosystem with many different habitats – each with its own collection of organisms that are adapted to live there. The skin between your toes is a much different environment from the skin on your hands or the top of your head. This leads to different parts of the skin being colonized by different kinds of bacteria. For example, Staphylococcus bacteria (which cause staph infections) are more common on the feet, toes and other moist areas, while Propionibacterium (which causes acne) is more common on the relatively oily skin of the face and back.
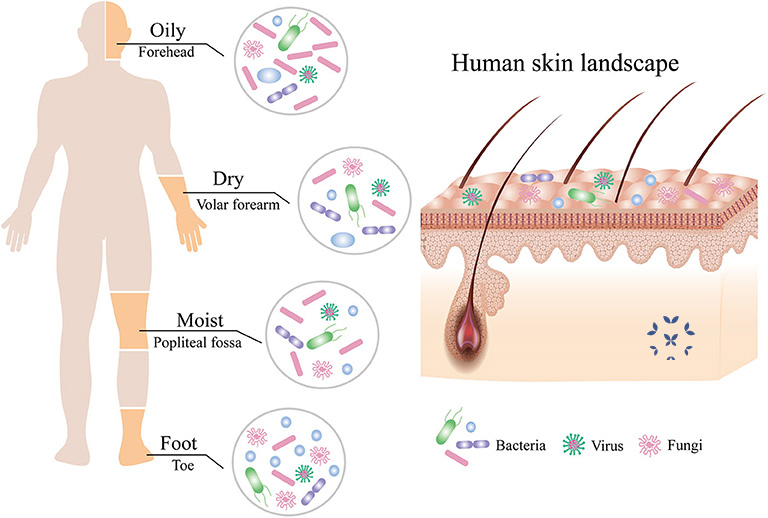
With so many different micro-environments, the skin can support a wide variety of microorganisms – over 1,000 species of bacteria alone!
As it turns out, this diversity is important. We tend to notice bacteria when they grow too numerous or cause noticeable problems, like the bacteria that cause acne in sebaceous glands, the bacteria that cause body odor in armpits or the those that infect minor cuts. However, an important role for the skin’s natural bacteria is to take up the space that might be otherwise occupied by other microorganisms – ones that might make us really sick.
This is where the skin microbiome actually cooperates with the immune system to fight infections. There are some bacteria that even produce antibiotics against competitive bacteria! Unfortunately, this also opens the door to immune “over reactions” and this may lead to triggering autoimmune diseases like psoriasis … and possibly to lupus.
In one example, there are T cells and dendritic cells (part of the immune system) that actually live in the skin. They not only can respond to potentially bad bacteria that try to invade the body, but they are also known to work with friendly skin bacteria to create chemicals called antimicrobial peptides (AMP’s), as well as antibodies, that then can attack the foreign microorganisms. This is an example of you immune system and your native microbiome working together for mutual protection.
This is a good thing, but it is not difficult to see how this cooperation might “go wrong” in the case of autoimmune conditions, like lupus, where the body ends up attacking the “good” bacteria or even its own skin cells.
 .
.
.
Lupus and the Skin Microbiome
Lupus affects the skin more than any other part of the body, other than the joints. So much so, that about 80% of those with lupus will have some skin involvement during their lifetime. This makes skin health particularly important for those living with lupus.
One well researched example of skin bacteria influencing an autoimmune disorder occurs when the Proprionibacterium bacteria that cause acne are replaced by too many Staphylococcus aureus bacteria. This simple change has been linked to the development of psoriasis in some patients.
In the case of lupus, recent studies have discovered several trends:
- The skin of SLE patients have significantly fewer kinds of bacteria than healthy individuals. The significance of this loss of microbiome diversity is not yet known.
- SLE patients also tend to have more of their skin colonized by Staphylococcus aureus than those who do not have SLE.
- In cutaneous lupus, special skin cells called SLE keratinocytes can overproduce a type of interferon that allows Staphylococcus aureus to colonize rapidly – producing lesions on the skin.
- Additionally, lupus patients tend to have a particular mix of three Staphylococcus bacteria on their skin. If this is found to be consistent, it might be possible to use these bacteria as “biomarkers” for accurately diagnosing SLE … without the need for a blood sample.
- Even the growth patterns of some skin bacteria, such as the level of Staphylococcus aureus in the nasal cavity, have been associated with level of kidney disease in lupus patients.
For more on how the body’s microbiome can affect SLE and cutaneous lupus, check out this video presentation, “Lupus Through the Looking Glass – Health Inside and Out” featuring dermatologist, Dr. Teri Greiling.
So what can you do to maintain a healthy microbiome with lupus?
So far, there is no definitive way to cause or prevent lupus based upon a person’s skin microbiome. However, there are things you can do, whether or not you are experiencing active lupus symptoms, to maintain healthy skin and a healthy microbiome. How?
Here is a good list of things to keep in mind:
- Protect the skin from damaging UV radiation – whether with clothing, sunscreen or avoiding too much direct sunlight. This is a good idea for anyone with lupus anyway.
- Regularly and gently wash your entire body using warm (not hot) water and mild cleansers that do not irritate the skin. Tamping dry also protects the skin from needless abrasion.
- Avoid using topical antibiotics unnecessarily – this can cause problems with beneficial bacteria or possibly create resistance strains of pathogenic bacteria. When in doubt, ask a trusted healthcare provider.
- Avoid dry, cracking skin by drinking plenty of water, and using skin moisturizers as necessary.
- Reducing stress can help! Emotions can affect skin. It is well-documented that stress can cause acne breakouts and trigger lupus skin reactions.
- Get enough sleep. Lack of sleep reduces subcutaneous blood flow and prevents the skin from healing itself.
- Eat a healthy diet, especially fruits, vegetables, whole grains and lean proteins.
- Avoid smoking. This narrows skin blood vessels and damages the skin’s collagen and elastin, which in turn increases wrinkles.
.
In Conclusion:
The complex relationship between your lupus and your skin’s microbiome is only now becoming the focus of serious research. Yet, the early findings are already changing how we view lupus and its effects on skin health … and that is important. After all, the skin is the largest and second most commonly affected organ by lupus – it pays to take care of it!
.
References
Boxberger, M., Cenizo, V., Cassir, N., & La Scola, B. (2021) Challenges in exploring and manipulating the human skin microbiome. Microbiome, (9). Article 125 https://doi.org/10.1186/s40168-021-01062-5
Byrd, a., Belkaid, Y., & Segre, J. (2018). The human skin microbiome. Nature Review. Microbiology, (16). 142-155. https://doi.org/10.1038/nrmicro.2017.157
Grice, E.A., & Segre, J.A. (2011). The skin microbiome. Nature Reviews. Microbiology, 9(4). 244-253. https://doi.org/10.1038/nrmicro2537
Huang, c., Yi, X., Long, H., Zhang, G., Wu, H., Zhao, M,. & Lu, Q. (2020). Disordered cutaneous microbiota in systemic lupus erythematosus. Journal of Autoimmunity,(108).
Mayo Clinic. (2022, January 22). Skin care: 5 tips for healthy skin. https://www.mayoclinic.org/healthy-lifestyle/adult-health/in-depth/skin-care/art-20048237
Sirobhushanam, S., Parsa, N., Reed, T.J., Berthier, C.C., Sarkar, M.K., Hile, G.A., Tsoi, L.C. Banfield, J., Dobry, C., Horswill, A.R., Gudjonsson, J.E., & Kahlenberg, J.M. (2020). Staphylococcus aureus colonization is increased on lupus skin lesions and is promoted by IFN-mediated barrier disruption. Journal of Investigative Dermatology, 140(5). 1066-1074. https://doi.org/10.1016/j.jid.2019.11.016
Zhou H-Y., Cao N-W., Guo B., Chen, W-J., Tao, J-H, Chu, X-J., Meng, X., Zhang, T-X., and Li, B-Z. (2021). Systemic lupus erythematosus patients have a distinct structural and functional skin microbiota compared with controls. Lupus, 30(10). 1553-1564. doi:10.1177/09612033211025095
Author: Greg Dardis, MS
Professor Dardis was formerly the Chair of the Science Department at Marylhurst University and is currently an Assistant Professor at Portland State University. His focus has been human biology and physiology with an interest in autoimmunity.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

