Lupus and the Endocrine System
The endocrine system doesn’t get the respect it deserves – after all, it influences almost every cell, organ and function of the body. It is also intimately connected to your immune system and can be heavily influenced not only by your lupus, but also by the medications you take. How? Read on to find out!
- Introduction : The 1-Minute Overview!
- The Endocrine System in a Bit More Detail
- How can you keep your endocrine system healthy?
- In Conclusion: The Most Important Take Aways!
Introduction: The 1-Minute Overview!
The job of your endocrine system is to help regulate the major functions of your body. It does this with a collection of organs, called glands, that produce chemical messages, called hormones, which are secreted directly into your blood stream. Ideally, it works with your nervous system to keep your body in balance, maintaining such things as body temperature, optimum rates of growth and metabolism, sufficient oxygen levels in your blood, healthy reproductive cycles, etc. It also plays a role in regulating the activity level of your immune system, and that is where lupus comes in!
Hormones can affect your lupus and lupus can affect your hormones!
We do not know exactly how some of this takes place, but here is a brief overview of what we do know!
- Those living with lupus have an increased risk of developing an endocrine disease, the most common of which involve the thyroid gland.
- About 22% of lupus patients with an endocrine disease have an increased risk of developing a second endocrine disease.
- Several hormones, especially estrogen can have a strong influence on lupus.
- Some lupus medications can have a dramatic effect on the endocrine glands. This is especially true for the pancreas and sex organs.
- The symptoms of many endocrine diseases, such as fatigue, brain fog and kidney involvement, can mimic lupus symptoms, making their diagnoses even more challenging.
- Yet, even though an endocrine disease may share some lupus symptoms, it will require its own, specific treatment plan, and one that may be quite different from what is prescribed for lupus.
- One endocrine gland, the thymus, directly affects how T cells develop, and T cells are one of the most important cellular components in causing the damage of autoimmune diseases like lupus.
In order to get beyond these basic facts, and to appreciate the truly awe-inspiring complexity of the endocrine system, it is helpful to describe different parts of the endocrine system and how each can affect your life with lupus.
Warning: This is a long article – 2,400 words. You may want to explore it one gland at a time!
Alternately, if you want to jump to the end, past all the details, and find out how to keep your endocrine system healthy – click here!
.
.
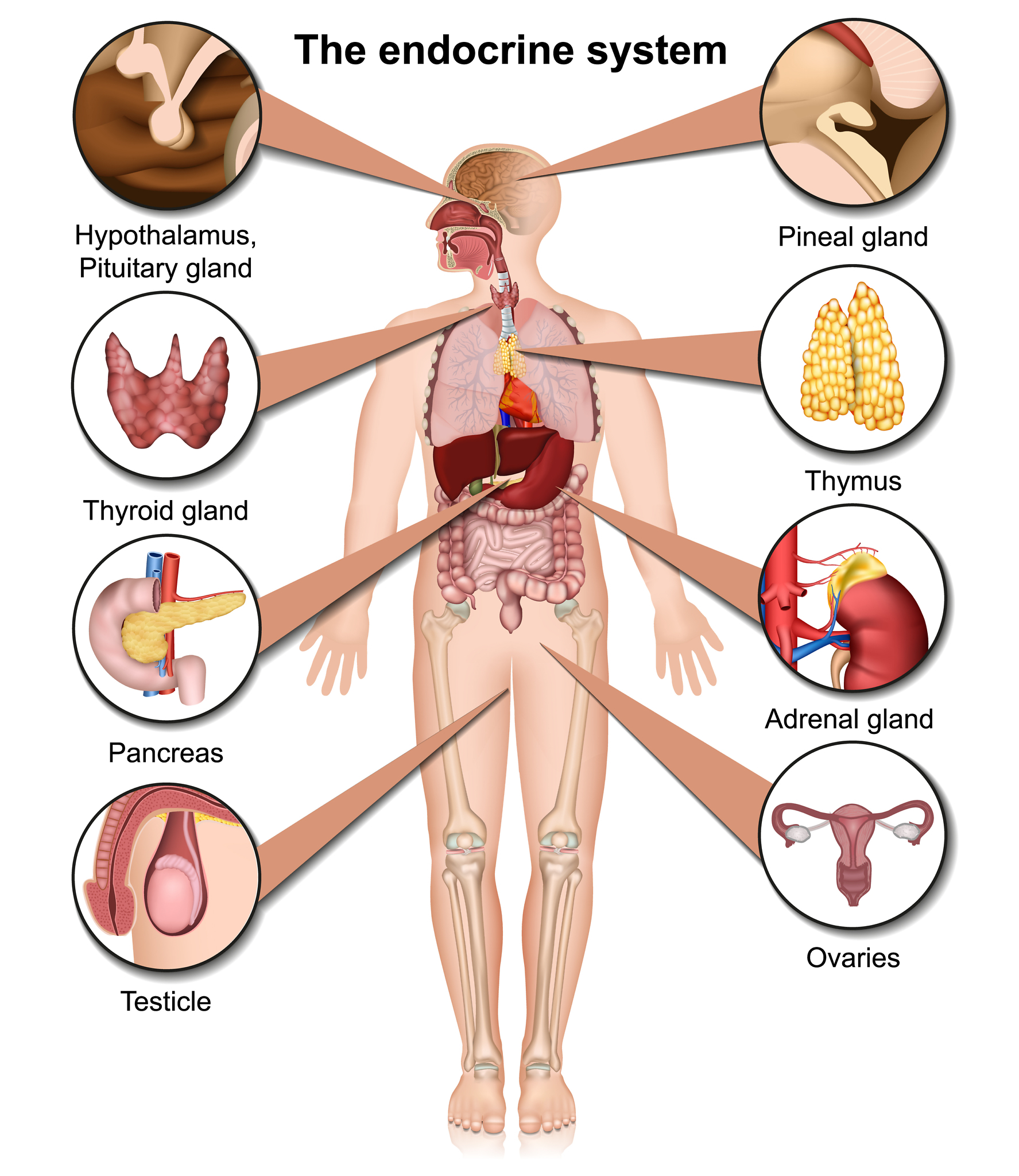
The Endocrine System in More Detail
The endocrine system is a collection of 9 or more organs in the body – usually called glands – each producing its own set of hormones. Unlike sweat glands and tear ducts, which are examples of exocrine glands, the endocrine glands secrete chemicals directly into the blood stream. In this way, hormones can spread throughout the body and can affect many other organs all at the same time.
These chemical messages are the messages of complex feedback loops that regulate almost all of the physiological functions of the body, such as:
- metabolic and growth rates;
- reproduction and sleep cycles;
- digestion and respiration;
- movement and sensory perception,
- even emotions like our mood and stress levels,
- and of course, immunity/autoimmunity.
You have probably heard about most of the endocrine glands before, but it is easy to forget how critical they are to every moment of your day. The ones most significant to lupus include the thyroid, parathyroids, thymus, pituitary, adrenals, the pancreas, ovaries, testes and pineal gland.
Trivia: There are other organs that are often not thought of as being part of the endocrine system, yet they can also secrete some hormones in special circumstances. These include the heart, stomach, liver, kidneys … even your skin.
The Thyroid
The thyroid is the gland seemingly most affected by lupus. Ironically, it is a butterfly-shaped organ that lies against the trachea at the front of your neck – about where the knot of a bow tie would be placed. Its hormones include:
- Thyroxine and triiodothyronine, which regulate your body’s base metabolic rate and influence a host of other things, such as your appetite, rate of digestion, the strength of your heart beat, overall growth rate, as well as your thought patterns and sexual functions.
- Calcitonin, which regulates the amount of calcium in your blood.
What does this mean for someone with lupus?
Lupus patients are predisposed to developing autoimmune thyroid diseases, and like lupus, autoimmune thyroid diseases affect women significantly more than men. Examples include:
- Hypothyroidism: When the thyroid produces less thyroid hormone than normal.
- This is the most common thyroid disease in patients with lupus – affecting about 6% to 15% of those with SLE.
- Symptoms include abnormal weight gain, a slow heart rate, fatigue, brain fog, hair loss, and sensitivity to cold.
- Hashimoto’s thyroiditis is an autoimmune condition and the leading cause of hypothyroidism in the U.S.
- Hyperthyroidism: This is the production of too much thyroid hormones.
- It occurs in about 1% to 9% of those with lupus.
- It can lead to abnormal weight loss, increased appetite, insomnia, anxiety, an irregular heartbeat, tremors, anxiety and sensitivity to heat.
- Grave’s Disease: This is anautoimmune disorder in which autoantibodies attack the thyroid. It is the most common cause of hyperthyroidism.
.
The Parathyroid Glands
These are four small glands located behind the thyroid. Their primary job is to control calcium and phosphate levels in the blood, and they do this by producing parathyroid hormone (PTH).
Hyperparathyroidism: This occurs when too much PTH is produced and blood calcium levels become too high (hypercalcemia) due to leaching calcium from the bones.
Hypoparathyroidism: This is the rare condition when too little PTH is produced and blood calcium levels drop.
What does this mean for someone with lupus?
- Diseases of the parathyroids are very rarely associated with lupus, but patients with SLE can develop hypercalcemia as a symptom of their disease and this may complicate the diagnosis of hyperparathyroidism.
The Pituitary Gland
The pituitary is the most important gland in the body. It sits directly under the brain, specifically under the hypothalamus. Even though it is only about the size of a pea, it controls many of the other endocrine glands by producing hormones such as:
- Adrenocorticotropic hormone (ACTH), which regulates the production of cortisol.
- Follicle-stimulating hormone (FSH), which stimulates the ovaries to produce estrogen.
- Growth hormone (GH), which stimulates, among other things, muscle and bone growth.
- Luteinizing hormone (LH), which stimulates ovulation by the ovaries and testosterone production by the testes.
- Prolactin, which stimulates breast milk production.
- Thyroid-stimulating hormone (TSH), which stimulates your thyroid to produce its own hormones.
What does this mean for someone with lupus?
- The relationship between lupus and the pituitary is unclear.
- Yet, about 2% of those with autoimmune hypophysitis (AH), the autoimmune inflammation of the pituitary, also have lupus.
- Some studies have shown that the excessive production of prolactin (hyperprolactenemia) can contribute to lupus disease activity. How? Prolactin can influence the levels of estrogen and testosterone in both men and women. In turn, estrogen levels are associated with the onset of SLE – and perhaps why lupus affects females ten times as much as males after puberty. This is an important area of active research!
The Pineal Gland
The pineal is a small pine cone shaped gland near the center of the brain between the two hemispheres. It secretes the hormone, melatonin, which helps control sleep patterns.
What does this mean for someone with lupus?
- Studies have found significantly lower melatonin levels in patients with lupus. This might add to the reasons for why over half of all patients with lupus have trouble with sleep and may be an indicator of neural involvement.

The Thymus
The thymus is another butterfly-shaped gland that lies just under your sternum (breastbone) and is actually part of two systems: the endocrine system (because it produces several hormones) and the lymphatic system, because it also contains may lymphocytes (white blood cells) important for immunity. The name “T cell” actually is short for “thymus cell lymphocytes.”
The thymus produces the hormones thymopoietin, thymosin and thymulin, which regulate the development of T cells.
What does this mean for someone with lupus?
- Since T cells are central to many aspects of the overactive inflammatory and autoimmune responses in with lupus, how the thymus may be involved in creating over-active T cells could be a key element in possible future therapies.
For more about T cells, the thymus and how they relate to lupus, check out the blog-article, “Lupus – B Cells, T Cells and the Immune System.”
The Adrenal Glands
The adrenal glands rest on top of each of your kidneys and produce a number of hormones, in particular the ones that are often involved in stress and the “fight or flight” response. These hormones include: adrenaline, cortisol and aldosterone.
Low production of cortisol by the adrenal glands is called adrenal insufficiency (AI) or Addison’s disease (an autoimmune condition). Cushing’s disease occurs when the adrenals produce too much cortisol.
What does this mean for someone with lupus?
- Some symptoms of adrenal insufficiency are similar to those of lupus so this might delay an accurate diagnosis of both.
- The symptoms of Cushing’s disease resemble some effects of long-term use of corticosteroids as treatments for lupus. Treating for Cushing’s can also possibly trigger a lupus flare.
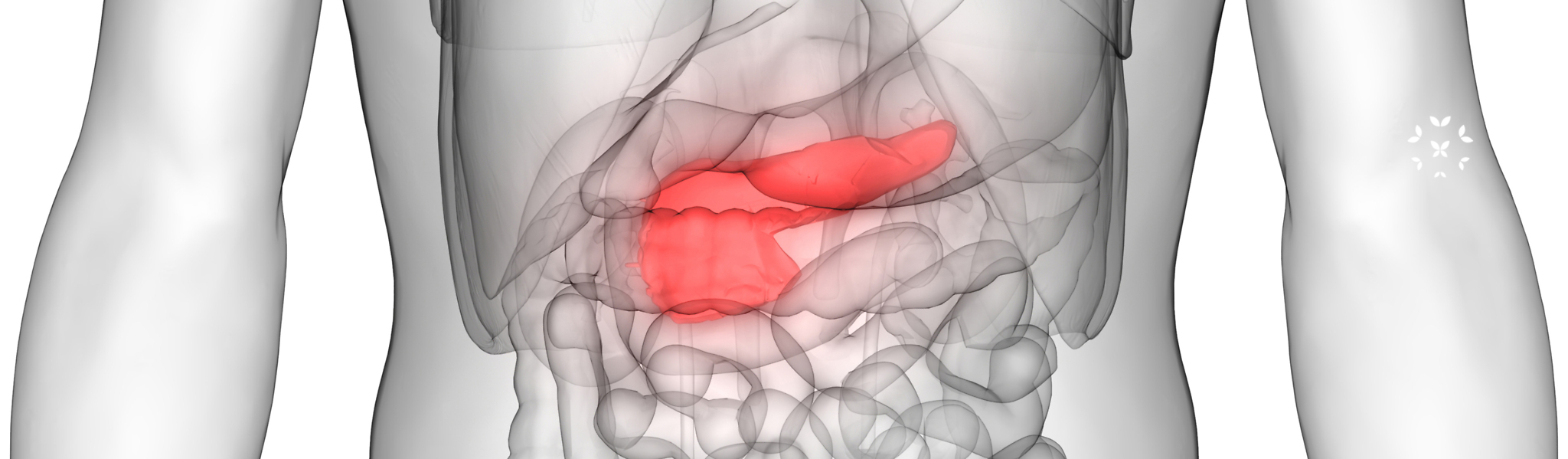
The Pancreas
As an endocrine gland, the pancreas helps regulate the sugar levels in the blood with glucagon, which raises blood sugar, and more famously, insulin, which lowers blood sugar. Diabetes is the increasingly common condition where either the pancreas does not have the ability to produce insulin, or produces some, but cannot utilize it correctly.
What does this mean for someone with lupus?
- Though rare, lupus-associated pancreatitis can be a serious,possibly fatal condition.
- SLE has been associated with insulin resistance, and this puts those with lupus at a higher risk for diabetes.
- Lupus patients with diabetes are also at a higher risk for end-stage renal failure.
- Some medications for treatment of lupus, such as glucocorticoids and mycophenolate mofetil (MMF) have been known to increase the risk of diabetes.
Ovaries
The ovaries are amazing organs. Not only do they produce the eggs (ova) that were the beginning of every single human being who ever lived, but they are also part of the endocrine system and secrete hormones, most notably: estrogen and progesterone.
What does this mean for someone with lupus?
- Estrogen has long been recognized as a factor in strengthening the body’s immune response.
- It is considered one of the most important reasons for why women are 9-times more likely to have lupus than men.
- Many women have more lupus symptoms before menstrual periods and/or during pregnancy, when estrogen production is high.
- Many women find that lupus symptoms decrease significantly after menopause.
- Lupus has been associated with some ovarian conditions, such as:
-
- Primary ovarian insufficiency, which occurs when ovaries stop releasing eggs and a woman’s periods end before the age of 40.
- Irregular menstrual cycles: These are not uncommon for those with lupus and some menstrual irregularities can also be caused by lupus medications, like prednisone and other glucocorticoids.

.
Testes
The testes are the male sex organs, analogous to female ovaries. They produce the sperm, and also secrete androgen sex hormones, most significantly, testosterone. Interestingly enough, both sperm and testosterone production are controlled by hormones produced by the pituitary gland.
What does this mean for someone with lupus?
- Lupus itself, does not necessarily affect the testes or testosterone levels.
- It is possible that lupus may induce anti-sperm antibodies. However, this is not uncommon in men who do not have lupus.
- In men, there are several common lupus drugs that can affect the testes and possibly reduce sperm count or lead to infertility: methotrexate, sulfasalazine, cyclophosphamide and mycophenolate mofetil (CellCept).
For more information on lupus and men, check out the blog-article, “Symptoms of Lupus in Men” by clicking here.

How can you keep your endocrine system healthy?
- Maintain a healthy (perhaps anti-inflammatory) diet and eat foods rich in the omega 3’s and 6’s, which can be found in salmon, halibut, walnuts, cashews and avocados
- Avoid as much as possible, junk food! Too much refined sugar, salt and processed foods can affect your endocrine system and increase your risk of developing Type 2 diabetes.
- Be aware of your family history and talk openly with your doctor about any concerns you may have regarding your endocrine system.
- Talk to your doctor before you make any dramatic changes to your exercise regime or diet, and be careful of supplements that claim to improve your endocrine system.
- Try to be as physically active as possible. This can mean walks and low impact workouts like yoga. Don’t push yourself too hard, but keep moving! Physical activity can positively affect the feedback loops within the endocrine system!
- Reduce stress! Make sure to get 7-8 hours of sleep each night, try meditation, breathing exercises, and calm or repetitive activities like walking, knitting, etc.
In Conclusion: The Most Important Take Aways!
The endocrine system is a complex chemical network of feedback loops, controlled by glands spread all throughout the body. With all the possible things that could go wrong, it is truly a miracle that any of it works at all!
How can your lupus affect the endocrine system?
- Lupus can increase a person’s risk of developing an endocrine disease, but no one is sure why.
- Though it is relatively rare, inflammation caused by the autoantibodies associated with lupus can directly damage glands of the endocrine system.
- Some lupus symptoms can mimic and mask those of an endocrine condition.
- The most common endocrine conditions that are influenced by lupus include problems with the thyroid and sex organs.
How can the endocrine system affect your lupus?
- Statistically, having an endocrine disease with their lupus does not seem to increase a patient’s mortality.
- Most often, endocrine disease developed after lupus was diagnosed.
- Of course, it is possible for a person to develop an endocrine disease that is not directly related to their lupus.
- Some symptoms of endocrine conditions can mimic and mask those of lupus.
- Several lupus medications have been found to increase the risks for some endocrine diseases.
Finally, the most important thing is to consistently take you prescribed medications and stick to your treatment plans in order to reduce your overall disease activity and avoid the flares. Active flares can lead to organ damage and that can include those amazing , endocrine glands!
References
Choux C, Cavalieri M, Barberet J, et al. Traitements immunosuppresseurs et préservation de la fertilité: indications et modalités pratiques [Immunosuppressive therapy and fertility preservation: indications and methods]. Rev Med Interne. 2018;39(7):557-565. doi:10.1016/j.revmed.2018.02.010
Hickman, R.A., & Gordon, C. (2011). Causes and management of infertility in systemic lupus erythematosus. Rheumatology, 50(9):1551-8. doi: 10.1093/rheumatology/ker105
Klionsky, Y., & Antonelli, M. (2020). Thyroid disease in lupus: An updated Rreview. ACR open rheumatology, 2(2), 74–78. https://doi.org/10.1002/acr2.11105
Kostoglou-Athanassiou, I., Athanassiou, L., and Athanassiou, P. (2021). Endocrine manifestations of systemic lupus erythematosus. Hamdy, R, & Mohammed, A. (Eds.), Lupus. IntechOpen. DOI:10.5772/intechopen.97363
Jara, L. J., Medina, G., Saavedra, M. A., Vera-Lastra, O., Torres-Aguilar, H., Navarro, C., Vazquez Del Mercado, M., & Espinoza, L. R. (2017). Prolactin has a pathogenic role in systemic lupus erythematosus. Immunologic Research, 65(2), 512–523. https://doi.org/10.1007/s12026-016-8891-x
Jiang, M.Y., Hwang, J.C. & Feng, IJ. (2018). Impact of diabetes mellitus on the risk of end-stage renal disease in patients with systemic lupus erythematosus. Nature Scientific Reports, 8, Article 6008. https://doi.org/10.1038/s41598-018-24529-2
Lee, K.H., Lee, H.J., Lee, C., Kim, J.Y., Kim, J.M., Kim, S.S., Jeong, S., Hwang, I.S., Kim, N., Kim, N.E., Shin, S., Shin, D., Song, J.S., Shin, D.H., Kim, J.D., Kim, J., Lee, Y.S., Kang, H., Kim, … Shin, J. (2019). Adrenal insufficiency in systematic lupus erythematosus (SLE) and antiphospholipid syndrome (APS): A systematic review. Autoimmunity Reviews,18(1). 1-8. https://doi.org/10.1016/j.autrev.2018.06.014.
Li, J., May, W., & McMurray, R.W. (2005). Pituitary hormones and systemic lupus erythematosus. Arthritis and Rheumatism, 52(12). 3701-3712. https://onlinelibrary.wiley.com/doi/epdf/10.1002/art.21436
Makol, A., & Petri, M. (2010). Pancreatitis in systemic lupus erythematosus: frequency and associated factors — A review of the Hopkins Lupus Cohort. The Journal of Rheumatology, 37(2). 341-345. https://www.jrheum.org/content/37/2/341
Muñoz, C., & Isenberg, D.A. (2019). Review of major endocrine abnormalities in patients with systemic lupus erythematosus. Clinical and Experimental Rheumatology, 37(5), 791-796. https://pubmed.ncbi.nlm.nih.gov/31172923/
Panareses, A., D’Andrea, V., Pironi, D., & Filippini,A. (2014) Thymectomy and systemic lupus erythematosus (SLE), Annali Italiani di Chirurgia, 85(6). 617-618. https://pubmed.ncbi.nlm.nih.gov/25919914/
Robeva, R., Tanev, D., Kirilov, G., Stoycheva, M., Tomova, A., Kumanov, P., Rashkov, R., & Kolarov, Z. (2013) Decreased melatonin levels in women with systemic lupus erythematosus – a short report. Balkan Medical Journal, 30(3). 273-276. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4115899/
The Cleveland Clinic. (2022, May 15). Thymus. https://my.clevelandclinic.org/health/body/23016-thymus
The Mayo Clinic. (2022, August 13). Hyperparathyroidism. https://www.mayoclinic.org/diseases-conditions/hyperparathyroidism/symptoms-causes/syc-20356194
Stein, E.M., & Erkan, D. (2018, May 21). Top 10 points lupus patients should know about autoimmune thyroid diseases. Hospital of Special Surgery. https://www.hss.edu/conditions_top-ten-series-lupus-autoimmune-thyroid-diseases.asp
Xiang, P., We, Q., Zhang, H., Luo, C., & Zou, H. (2020). Autoimmune Hypophysitis With Systemic Lupus Erythematosus: A Case Report and Literature Review. Frontiers in Endocrinology, 11, 579436. https://doi.org/10.3389/fendo.2020.579436
Author: Greg Dardis, MS
Professor Dardis was formerly the Chair of the Science Department at Marylhurst University and is currently an Assistant Professor at Portland State University. His focus has been human biology and physiology with an interest in autoimmunity. Professor Dardis is also the President of the Board of Directors of Kaleidoscope Fighting Lupus.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

