Lupus Retinopathy
Lupus retinopathy is the most common vision concern for those living with SLE, and is often one of the first symptoms for the newly diagnosed. Yet, serious problems with eyesight are relatively rare, and there are many ways to avoid the damage that lupus can cause. So, read on to learn more about how lupus affects the eyes and what can be done to protect your vision.
- Introduction – the 30-second Overview
- The Eye – A Very Brief Overview
- Lupus and Retinopathy
- In Conclusion
.
Introduction – the 30-second Overview:
“Retinopathy” refers to any kind of damage to the retina of the eye, the light-sensitive layer of cells in the back of the eye … the part that acts like the sensor in a smart phone camera. This can lead to different amounts of vision loss. The most common type of retinopathy involves microscopic damage to the small blood vessels of the retina that is often caused by diabetes or high blood pressure (hypertension). As a matter of fact, diabetic retinopathy is the leading cause of blindness in people 25-65 years of age and accounts for 5% of blindness world-wide.
Lupus and other autoimmune diseases can also damage these blood vessels – reducing blood flow and leading to vision impairment and other eye complications. This is also referred to as retinal vascular disease.
Here are the most important facts regarding lupus retinopathy:
- Retinopathy is the most common form of damage to the eyes involving SLE.
- Retinopathy affects about 16% of all newly-diagnosed lupus patients – ranging from 3% of patients with low disease state, to approximately 28% for those who are hospitalized for their lupus.
- The damage to vision also ranges widely from barely noticeable to severe vision loss.
- Retinopathy is often an early symptom of lupus, and can even be the first indicator of an eventual SLE diagnosis.
- Some medications, most notably hydroxychloroquine, are known to have a toxic effect on the retina. Hydroxychloroquine retinopathy can occur when high doses are taken over a long period of time.
- Regular eye exams are critical in order to detect retinopathy early so that steps can be taken to avoid or minimize the damage as much as possible.
- Most lupus patients will only experience very mild forms of retinopathy, if any, and the risk of significant vision loss, much less blindness, is quite low.
For more information on the eye and lupus retinopathy, keep reading!
.
[Image courtesy of the National Eye Institute (public domain)]
.
The Eye – A Very Brief Overview:
The eye is an amazing and complex organ. It is both incredibly delicate, and yet surprisingly resilient – as it has one of the quickest rates of healing anywhere in the body.
Of course, it is the sensory organ of sight and gathers light with exquisite detail. Light passes through many layers and tissues, from the cornea, through the pupil, then the lens, then the gel-like vitreous humor and finally on to the retina. The retina is made up of special photoreceptor cells, the rods (for dark and light) and cones (for colors) that many learn about it in biology classes. These special cells convert light into electrical signals that pass to the optic nerve on the way to the brain for further processing.
Some interesting facts about the eye and retina:
- It is estimated that about 70-79% of people have brown eyes, 8-10% have blue eyes and only 2% have green eyes.
- The only tissue in the human body that does not contain blood vessels is the cornea of the eye.
- The retina is actually made up of 10 layers of cells that contain nerves, blood vessels and the photoreceptor cells.
- There are about 120 million rods and 7 million cones in the retina.
- Humans can see more shades of green than any other color.
- The resolution of the human eye would be similar to that of a 576 megapixel camera.
- The part of the retina where the optic nerve is located has no rods or cones and that is why it is called the “blind spot.”
- The macula is a very small area of the retina (less than ¼ inch wide) where all of your central visual focus takes place. It is where you see the most color and the finest details. The macula is also where people notice retinal damage first.
It is possible for lupus to affect any of the many tissue layers, blood vessels and nerves that make up the eye. However, the retina is the most common and that is where lupus retinopathy takes place.
Lupus and Retinopathy:
The two most common forms of retinal damage due to lupus include retinal vasculitis and vaso-occlusive retinopathy.
Retinal vasculitis (RV) is the inflammation of the blood vessels of the retina, and is the most common way that lupus can damage the eyes. One study found that lupus patients are approximately 23 times more likely to have RV than the non-lupus population.
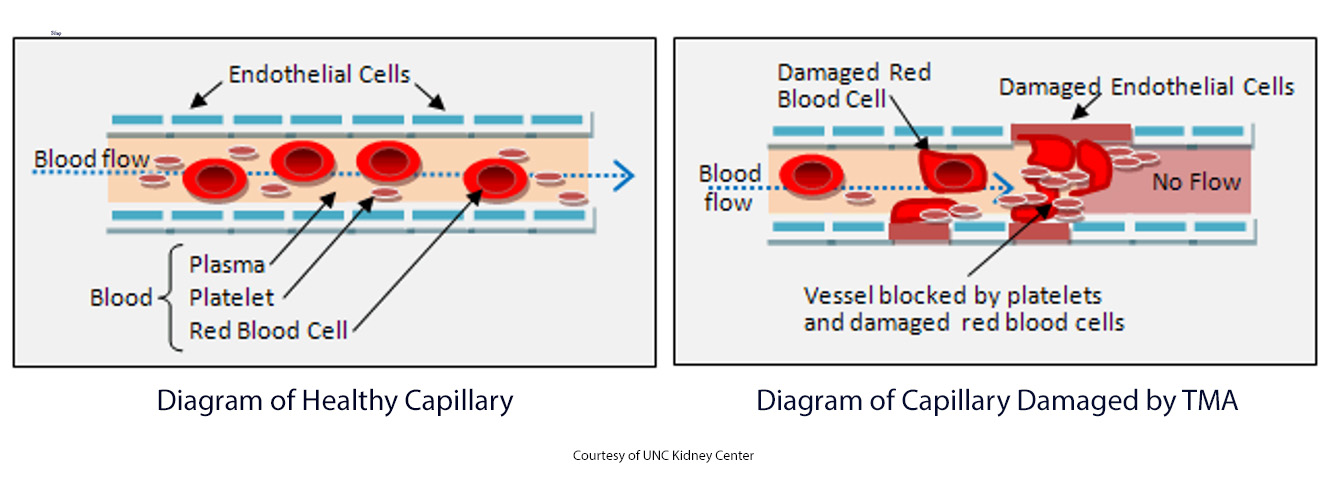
Vaso-occlusive retinopathy is the term for when small blockages in the retina form and affect a person’s vision. These micro-clots are not unlike those that can affect the delicate capillaries of the kidneys in lupus nephritis. Another technical term for this kind of damage is thrombotic microangiopathy (TMA).
Other related eye conditions caused by lupus include:
- Dry Eye: Lupus and the overlapping condition of Sjögren’s syndrome can produce dry eye, which, though not directly affecting the retina, can lead to itching and irritation of several parts of the eye (such as the cornea), which can make any retinopathy worse. Some studies suggest that about one-third of those living with lupus may experience dry eye syndrome and from 14%-18% of those with SLE, also have Sjögren’s.
- Choroiditis: This is the inflammation of the choroid, the thin layer of blood vessels that lies between the retina and the sclera (the whites of the eyes).
- Optic Neuritis: Systemic inflammation caused by lupus can also attack the optic nerve. Though this is quite rare (about 1% of those with SLE) and not considered a retinopathy, it can dramatically affect how the retina sends its signals to the brain.
.
Symptoms
Often lupus retinopathy may be so minor, that no symptoms are even noticed. If damage is enough to affect eyesight, the most common symptoms include:
- Blurred or distorted vision;
- “Floaters,” the dark specks or strings that create shadows on the retina and drift across a person’s vision when the eyes are moved.
- Changes to a person’s color vision.
.
Diagnosis
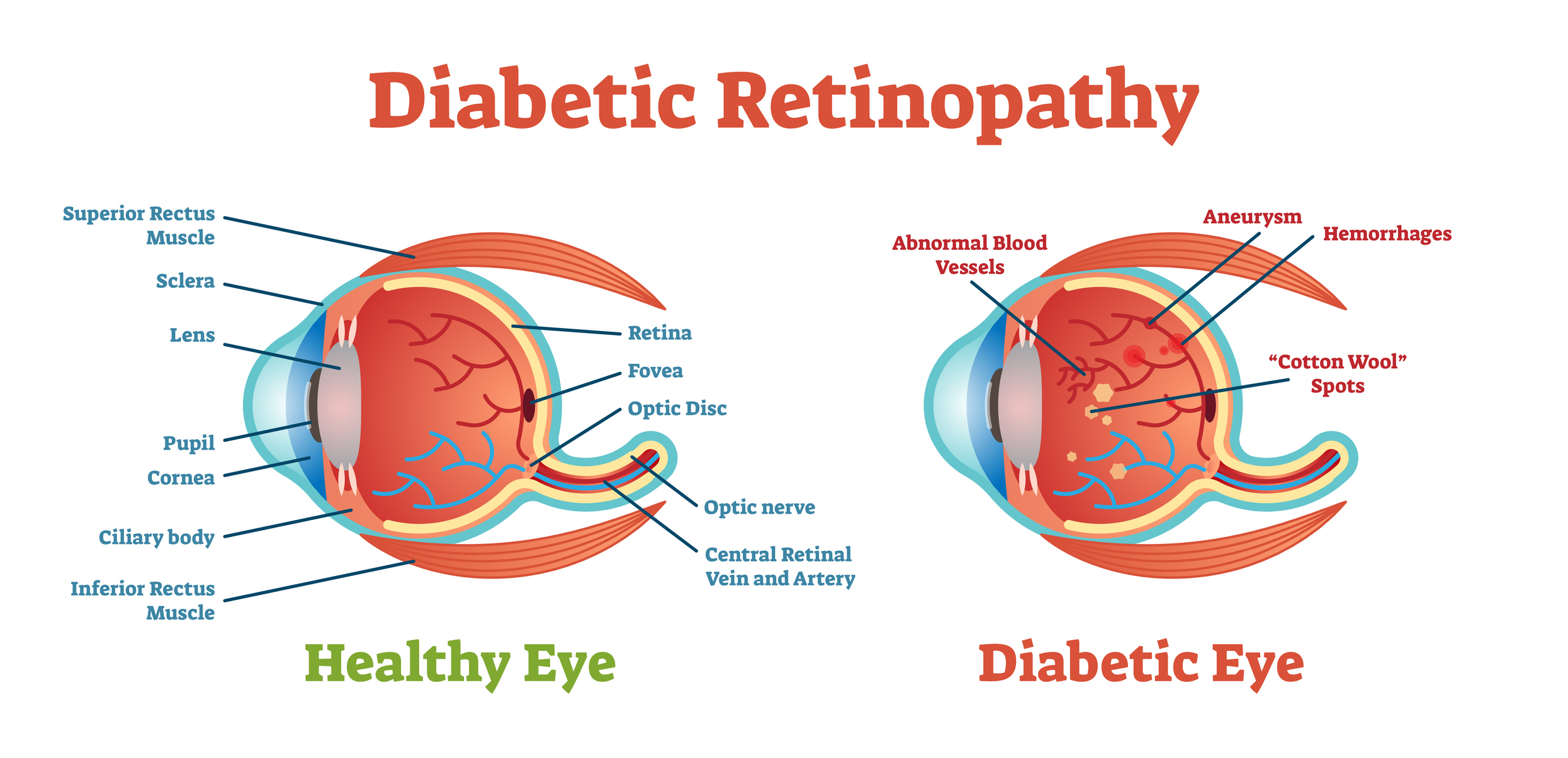
Diagnosing lupus retinopathy requires careful eye examinations by an ophthalmologist. Sometimes called a funduscopic exam, these involve an ophthalmoscope, which uses special lights and magnifying lenses to detect retinal blood vessel damage, such as blood clots, ruptured capillaries, or swelling in the retina or around the optic nerve.
Often, about 78% of the time, this damage will look like fuzzy white patches on the retina called, “cotton wool” spots.
This cannot be stated enough – it is imperative for those living with lupus, especially those taking high dosages of hydroxychloroquine to have regular eye exams – screenings – in order to detect any possible retinopathy early!
.
Treatment and Other Considerations
Thankfully, many lupus medications also reduce a person’s risk for retinopathy. How? Medications that reduce overall inflammation in the body or reduce the production of auto-antibodies can also protect the retina and its blood vessels from the systemic damage that both can cause.
Treatments include:
- Anti-inflammatories like corticosteroids, which can reduce systemic inflammation and the risks for retinal vasculitis. In rare cases, methylprednisolone therapy may be needed.
- Anticoagulants (blood thinners), which can be taken to maintain a healthy supply of blood to the retinas.
- In the very rare, severe situations, when blindness is a threat, a technique called retinal laser photocoagulation may be used to prevent abnormal blood vessels or blockages from creating more damage.
Other Considerations:
- Avoid Some Salicylates: It is suggested that lupus patients with some retinopathy avoid consuming some salicylates, like aspirin and the traditional quinine found in tonic water. These, like hydroxychloroquine, may increase the risks of retinal damage.
- Regular Exercise: This has been found to help lower the incidence and progression of retinopathy as well as overall inflammation.
- Eye Surgeries: Also, due to possible problems with healing after some surgical procedures, the FDA has suggested that lupus patients might not be good candidates for some elective eye procedures, like LASIK surgeries. However, necessary procedures, like cataract surgeries, are typically quite successful.
- Pregnancy: Pregnancy can pose challenges, as hormonal changes may impact lupus activity and potentially worsen retinal involvement. Close collaboration between obstetricians, rheumatologists, and ophthalmologists is essential to navigate these complexities.

.
In Conclusion:
While lupus retinopathy is rather common and can become a serious condition, it can be easily diagnosed and treated with regular eye exams. Keep the following in mind:
- Consistently follow your treatment plan.
- Schedule regular vision screenings, especially if you are taking hydroxychloroquine.
- Maintain a healthy diet and exercise program.
- Protect your eyes from sunlight and trauma.
- Learn as much as you can about how lupus can affect your eyes, and be observant for any changes in your vision.
Following these simple guidelines will go a long way to maintain good eyesight while living with lupus!
.
References
Alderaan, K., Sekicki, V., Magder, L.S., & Petri, M. (2015). Risk factors for cataracts in systemic lupus erythematosus (SLE). Rehumatology International, 35(4), 701-708. https://pubmed.ncbi.nlm.nih.gov/25257763/
Bashiri, H., Karimi, N., Mostafaei, S., Baghdadi, A., Nejadhosseinian, M., & Faezi, S.T. (2021). Retinopathy in newly-diagnosed systemic lupus erythematosus: Should we screen for ocular involvement? BMC Rheumatology, (5)34. https://doi.org/10.1186/s41927-021-00203-5
Chan, K. (2023, June 14). Eye problems in lupus. Hospital for Special Surgery. https://www.hss.edu/conditions_eye-problems-lupus.asp
Chen, X-H., Shi, J-C., Wei, J. C-C, Chen, H-H., & Mo, H-Y. (2021). Increased risk of retinal vasculitis in patients with systemic lupus erythematosus: A nationwide population-based cohort study. Rheumatology, 8. https://www.frontiersin.org/articles/10.3389/fmed.2021.739883/full
Cleveland Clinic. (2022, May 25). Macula. https://my.clevelandclinic.org/health/body/23185-macula
Huang, G., Shen, H., Zhao, J., & Mao, J. (2020). Severe vaso-occlusive lupus retinopathy in the early stage of a pediatric patient with systemic lupus erythematosus: a case report. Medicine, 99(16), e19875. DOI: 10.1097/MD.0000000000019875
Kharel Sitaula, R., Shah, D. N., & Singh, D. (2016). Role of lupus retinopathy in systemic lupus erythematosus. Journal of ophthalmic inflammation and infection, 6(1), 15. https://doi.org/10.1186/s12348-016-0081-4
Palejwala, N.V., Walia, H.S., & Yeh, S. (2012). Ocular manifestations of systemic lupus erythematosus: A review of the literature. Autoimmune Diseases, Article 290898. https://doi.org/10.1155/2012/290898
Saha, M. (2023). Thrombic microangiopathy (TMA). University of North Carolina Kidney Center. https://unckidneycenter.org/kidneyhealthlibrary/glomerular-disease/thrombotic-microangiopathy-tma/
Wong, R.W., & Cunningham, E.T. (2013, January 17). Posterior segment findings in SLE. Review of opthalmology. https://www.reviewofophthalmology.com/article/posterior-segment-findings-in-sle
.
Author: Greg Dardis, MS
Professor Dardis was formerly the Chair of the Science Department at Marylhurst University and is currently an Assistant Professor at Portland State University and the American College of Healthcare Sciences. His focus has been human biology and physiology with an interest in autoimmunity. Professor Dardis is also a former President of the Board of Directors of Kaleidoscope Fighting Lupus.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

