Running Out of Rheum: The Global Shortage of Rheumatologists!
The access, time, and attention you have with your rheumatologist are vital to your health and treatment planning. However, with more rheumatologists retiring than going into the field, that access may become more challenging. Read on to find out about the shortage of rheumatologists, and how this might affect you.
- Introduction: How big is the problem?
- Why is there a shortage?
- What can be done about it?
- What could this mean for you?
- In Conclusion
Introduction: How big is the problem?
At a time when public awareness of lupus is growing and the number of treatments are expanding, the number of rheumatologists, those specialists trained to diagnose and treat rheumatic diseases like lupus, is declining.
The American College of Rheumatology (ACR), the preeminent organization that tracks trends and provides guidance for the rheumatological medical community, is trying to find out how big the problem is and what can be done about it. Based upon one ACR study:
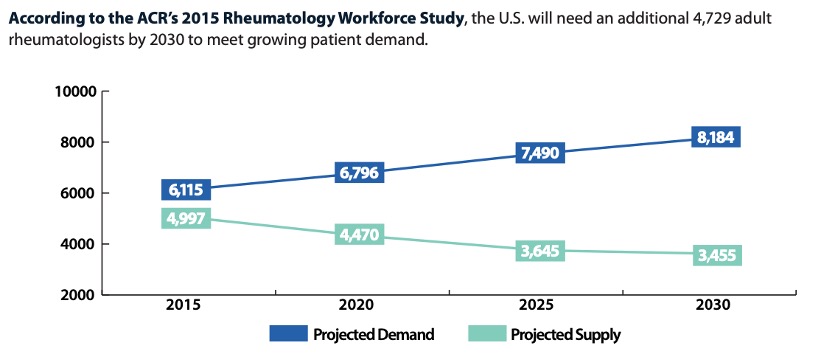
- In 2015, there were 4,997 adult rheumatologists in the U.S. That was already approximately 1,100 fewer than were needed.
- By 2020, only 5 years later, the demand for rheumatologists increased by 680, yet the number of rheumatologists dropped by over 500 to 4,470. The study estimates that the problem will only get worse.
- By 2030, the demand for rheumatologists will increase by 140% and the supply will decline to about 3,455 – leaving a gap of 4,729 too few rheumatologists!
As many living with lupus know all too well, this can mean long waits between appointments with a rheumatologist. One study showed that the average wait time for a new patient appointment is over 6 weeks.
This is not only aggravating, but it can have a big impact on tracking new and the transitory symptoms common in lupus. It can lead to a rheumatologist missing important changes in a patient’s disease state and add to the difficulty in making timely changes to their treatment plans.
The lack of rheumatologists is even greater in rural areas, and this means that some patients must drive long distances, 200 miles or more, to see the nearest specialist. It also means that for some patients the lack of options puts them in a difficult situation. For some who move, even to a different state, it is increasingly common that they keep their original rheumatologists. They would rather travel back to see them for appointments than to go through the hassle of finding a new one in their new city.
The problem is close to crisis proportions in pediatric rheumatology. In 2020 there were fewer than 350 board-certified pediatric rheumatologists in the U.S. while there are almost 300,000 juvenile arthritis patients.

There are a number of reasons why this is happening. Research in the U.S. has found that:
Rheumatologists are retiring and/or working less.
- About half of the rheumatologists in the U.S. are over 55 years of age.
- Over 50% of rheumatologists say they will retire in the next 5 to 10 years.
- 80% of those retiring will begin working part-time even earlier than that.
Fewer medical students are choosing rheumatology.
- It can be a challenge to attract medical students and other healthcare professional to rheumatology because they tend to be near the bottom of the salary scales in their fields.
- International medical students studying rheumatology in the U.S. often return home after graduating.
- 40% of rheumatology graduates choose academic medical careers over clinical ones.
- Other diseases are competing for resources, shifting the attention away from rheumatology and towards some emerging endemics and illnesses.
The demand for rheumatologists is increasing.
- It is estimated that by 2040, the demand will increase by 102% – more than double!
- The number of people who suffer other rheumatic diseases continues to increase. Arthritis and other musculoskeletal conditions have become the #1 one cause of disability in the United States, and these can dominate the attention of most rheumatologists.
The extent of the problem depends upon where you live.
- Those with lupus who live in less populated and underserved areas are most vulnerable to the rheumatologist shortage. In the U.S. for instance, 21% of rheumatologists in the U.S. are in the Northeast, while only 4% are in the Southwest.
- 90% of rheumatologists practice in metropolitan areas. Those with lupus who live outside of major cities often travel for hours to see a rheumatologist. Many never seek treatment out of frustration, and so their health deteriorates. This affects many who are already socioeconomically marginalized by the healthcare system.
In some parts of the globe, the shortage is even more concerning.
- There are only two pediatric rheumatologists in all of Africa to treat children who need care.
- India faces a similar shortage. As a result, many children requiring a diagnosis are not diagnosed until experiencing more than a year of symptoms.
- Those living with lupus in the United Kingdom may wait six months to see a rheumatologist.
- Rheumatologists in Germany and Austria do not have the time to see everyone who needs care. In Austria alone, rheumatologists often spend up to 20% of their time working in general practice due to widespread practitioner shortages.

What is being done to solve the problem?
The greatest focus is in attracting more healthcare professionals and medical students to become rheumatologists – and to also specialize in lupus and its overlapping diseases. How?
- The hope is to expand rheumatological education for medical students. This is done by providing more online training opportunities, subsidies for rheumatology study, and by introducing rheumatology as a specialty to medical students earlier in their education.
- A nonprofit called the Rheumatology Research Foundation (https://www.rheumresearch.org) is offering scholarships to recruit medical students and provide training in clinical rheumatology and research.
- Providing more rheumatology training to physician assistants, nurse practitioners, and even pharmacists can help to fill the gaps in care.
- Also, reducing barriers to employment in the U.S. for international medical students who are interesting in rheumatology may help.
- In the short-term, expanding telehealth for rheumatology visits can also bridge the widening gap for those living where a rheumatologist is not available.
For most living with lupus, this might affect the amount of time a rheumatologist has to meet with you during an appointment, and it may increase the time between office visits. Even though the causes for some of these changes are largely outside of the patient’s control, there are things you can do to get the most out of your rheum care.
- Join a local lupus support group to find out more about healthcare providers in your area and reach out online for advice and options.
- Take an active role in how you are being treated and find the rheumatologist with whom you feel the most comfortable and who makes themselves accessible.
- If you have a rheumatologist, set regular appointments so that you stay connected to your healthcare provider. Four or more times a year may be necessary if you have active symptoms or are concerned about lupus nephritis.
- Make sure to go to all your appointments. Do not assume that it will be easy to reschedule any that you miss.
- Become familiar with your telemedicine options so that, if necessary, you are more flexible in making appointments.

The shortage of rheumatologists is a serious issue, and for some reading this article, it may even be critical. However, there is increasing awareness about the problem and more options than ever to help solve it! A concerted effort on the part of medical schools and several organizations, like the American College of Rheumatology, will hopefully narrow the gap between number of rheumatologists and the need for those living with lupus and other autoimmune conditions.
In the meantime, if you do not have good access to a rheumatologist, reach out and find the support you need to find one. If you do have one, be the best patient you can be, and let them know how much you appreciate what they do!

References
Al Maini, M., Adelowo, F., Al Saleh, J., Al Weshahi, Y., Burmester, G., Cutolo, M., Flood, J., March, L., McDonald-Blumer, D., Pile, K., Pineda, C., Thorne, C., & Kvien, T. (2015) The global challenges and opportunities in the practice of rheumatology: White paper by the World Forum on Rheumatic and Musculoskeletal Diseases. Clinical Rheumatology, 34, 819-826. https://dx.doi.org/10.1007%2Fs10067-014-2841-6
American College of Rheumatology. (2022, February 17). 2105 Workforce Study of Rheumatology Specialists in the United States. [Graph] https://www.rheumatology.org/portals/0/files/ACR-Workforce-Study-2015.pdf
Battafarano, D., Ditmyer, M., Bolster, M., Fitzgerald, J., Deal, C., Bass, A., Molina, R., Erickson, A., Hausmann, J., Klein-Gitelman, M., Imundo, L., Smith B., Jones, K., Greene, K., & Monrad, S. (2018). 2015 American College of Rheumatology workforce study: Supply and demand projections of adult rheumatology workforce, 2015-2030. Arthritis Care & Research, 70(4), 617-626. https://doi.org/10.1002/acr.23518
Borenstein, D. (2021, September 20). Hug Your Rheumatologist: The Shortage is Coming. The Arthritis Connection. https://www.thearthritisconnection.com/rheumatoid-arthritis/hug-your-rheumatologist-the-shortage-is-coming
Miloslavsky, E.M., & Bolster, M.B. (2020) Addressing the rheumatology workforce shortage: A multifaceted approach. Seminars in Arthritis and Rheumatism, 50(4), 791-796. https://doi.org/10.1016/j.semarthrit.2020.05.009
Puchner, R., Vavrovsky, A., Pieringer, H., Hochreiter, R., & Machold, K. (2020). The supply of rheumatology specialist care in real life. Results of a nationwide survey and analysis of supply and needs. Frontiers in Medicine, 7(18), article 16. https://doi.org/10.3389/fmed.2020.00016
Rheumatology Research Foundation. (2022, February 19). Research and Training.https://www.rheumresearch.org/about-our-awards
Thomas, D. (24, April 2021). Worldwide shortage of lupus doctors = getting worse. The Lupus Encyclopedia Blog. https://www.lupusencyclopedia.com/blog/worldwide-shortage-of-lupus-doctors
Tyrrell, K. (2019, March 5). ACR Addresses the rheumatology workforce shortage. The Rheumatologist. https://www.the-rheumatologist.org/article/acr-addresses-the-rheumatology-workforce-shortage/
Volansky, R. (2021, February 18) Workforce shortage: Selling a specialty that should sell itself. Healio Rheumatology. https://www.healio.com/news/rheumatology/20210212/workforce-shortage-selling-a-specialty-that-should-sell-itself
Author: The KFL Team
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

