Lupus, the Heart and Cardiovascular System
Approximately half of individuals with lupus experience hypertension, making cardiovascular disease the number one cause of death. Explore the risks of cardiovascular disease and what can be done to treat these conditions and protect the heart.
.
Contents
- The Heart and its Role as Part of the Cardiovascular System
- Conditions of the Heart and Cardiovascular System
- Staying Healthy
- In Conclusion
Introduction
The average heart beats approximately 100,000 times a day. For an 80-year old, that adds up to an astonishing 280,000,000 beats over the years! It stands to reason how resilient the heart is – and how much demand is placed on it by the rest of the body – to keep us healthy, strong, and functioning at our best.
Sometimes things go awry, however. For individuals with SLE, the risk of developing various heart conditions and cardiovascular disease increases. Black women, for example, are three times as likely as white women to have lupus, and this raises the risk for heart and cardiovascular disease. It is really imperative for individuals with lupus to show the heart some love in order for it to keep beating strong.
Understanding the heart and cardiovascular system and their vulnerabilities can give you the framework you need in order take responsibility for your own well-being and give your heart some tender-loving care.
The Heart and its Role as Part of the Cardiovascular System
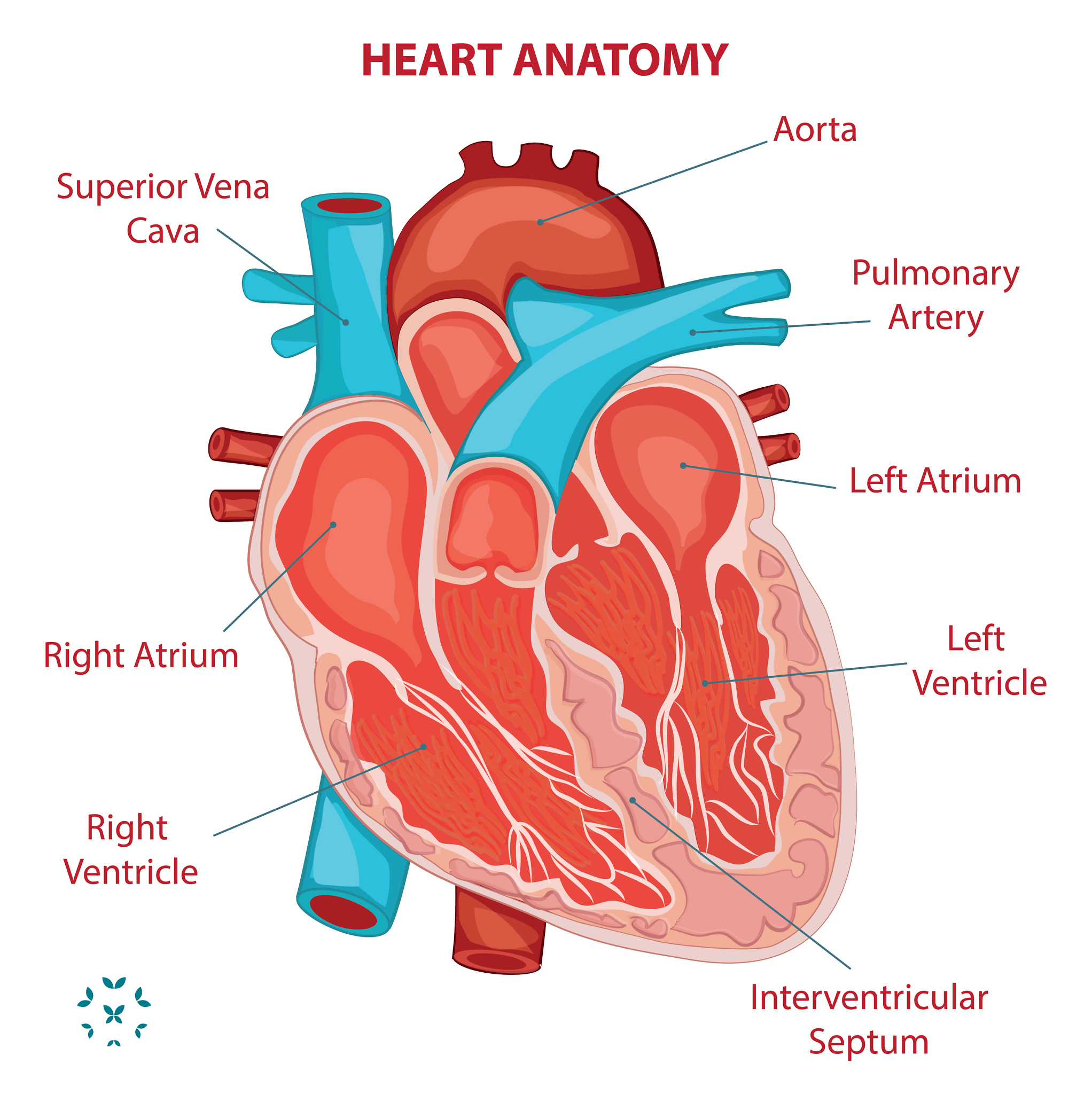
Your heart is the size of both of your fists placed together, and consists of four chambers: two large ventricles, and two smaller atria (the singular is atrium). The chambers are organized into two sides, the left and the right – each with an atrium and a ventricle – that operate almost as if they are two separate pumps. It is this double pump function that gives the heart its characteristic thump-thump or “lub-dub” sound when heard through a stethoscope.
Here’s a primer for how blood enters and exits the heart and moves throughout the body:
Blood enters the heart in two ways and from two sets of veins. The blood from most of your body enters the right atrium from two large veins: one from your head and upper body (the superior vena cava) and one from your legs and lower body (the inferior vena cava). This blood has given its oxygen to all parts of the body, and so the job of the right side of the heart is to get this blood to the lungs for more oxygen. The right atrium momentarily holds about one cup of blood at a time before passing it to the right ventricle through a one-way valve.
Actually, there are heart valves where blood both enters and exits each ventricle. These valves keep the blood flowing in one direction so that the entire circulatory system can carry oxygen, nutrients and wastes in the most efficient way. Damage to these valves can hurt this efficiency and is a common cause of heart disease.
From the heart’s right ventricle, blood is pumped to the lungs where it spreads out into the tiny capillaries of the alveoli so that it can pick up the oxygen that we draw in with each breath. Of course, this same blood dumps excess carbon dioxide into the lungs so that it can be removed from the body when we breathe out.
At this point, bright red, newly oxygenated blood now passes into veins, called pulmonary veins, which bring the blood to the left side of the heart – first the left atrium and then the left ventricle. It is from the left ventricle that the biggest push of blood occurs. The left ventricle pumps blood into our largest artery, the aorta, to be distributed to the rest of the body. It is this strong contraction from the left ventricle that creates the noticeable pulse in our wrists. As this blood moves around the body, it gives up oxygen and gains carbon dioxide and begins its journey back to the right atrium of the heart.
In a heart-healthy person, this cycle repeats constantly throughout the day, every day. The cardiovascular system functions like one of those highly-technical and sustainable plumbing systems that constantly recycles and reuses its own water, keeping it clean and toxin-free. Breakdowns in this system can occur, however, and it’s a good idea to understand what can happen and how to get things back into proper working order.
Conditions of the Heart and Cardiovascular System
Myocarditis
Relatively rare, less than 10% of individuals with lupus may develop myocarditis. Myocarditis is inflammation of the heart muscle which can lead to an enlarged, weakened heart that makes it difficult to pump and circulate blood and oxygen throughout the rest of the body. Symptoms may include a rapid heartbeat and chest pain. This condition needs immediate attention and regular monitoring.
- Diagnostic tools include: blood tests, x-rays, echocardiograms, electrocardiograms, MRIs, and/or cardiac catheterization and endomyocardial biopsy.
- Treatment may include: rest and abstinence from intense exercise for a period of time, antibiotics, corticosteroids, immunosuppressive therapy.
Endocarditis
Endocarditis is an infection of the inner lining (endocardium) of the chambers of the heart and valves. It is typically caused when bacteria or other germs enter the body through the mouth and spread through blood. It is a serious condition that can cause many complications and needs to be treated quickly.
Some individuals with lupus and individuals with antiphospholipid syndrome may develop a form of endocarditis called Libman-Sacks. Libman-Sacks endocarditis affects the heart valves, primarily the mitral and aortic valves. If left untreated, the bacteria from this condition can enter the bloodstream, potentially resulting in the spread of infection and even stroke. Approximately 15% of individuals with lupus may develop Libman-Sacks.
- Diagnosis tools include: blood tests, x-rays, echocardiograms, electrocardiograms, CT scans, and/or MRIs.
- Treatment may include: antibiotics and sometimes surgery which may include heart valve replacement.
Pericarditis
The most common heart abnormality in individuals with lupus, pericarditis has been reported to affect between 6 – 45% of individuals with lupus and often goes undiagnosed. Pericarditis is the inflammation and irritation of the pericardium, the thin sac-like membrane that surrounds the heart. Symptoms can be acute with quick onset, but do not last long. Symptoms can also be chronic if they appear gradually and are persistent.
- Diagnostic tools may include: chest x-ray, CT scan, MRI, echocardiogram, fluid drainage (rare), and/or electrocardiogram.
- Trfeatment may include: antibiotics, pain relievers, fluid drain, corticosteroids, colchicines, and/or surgery including pericardiocentesis and/or pericardiectomy (cutting a hole in the pericardium).
 Blood Pressure and Hypertension
Blood Pressure and Hypertension
Blood pressure is the strength at which your blood is pushed against the sides of your blood vessels. The top number in a blood pressure reading – the systolic reading – is the pressure in your blood vessels when the left ventricle contracts. The bottom number – the diastolic reading – is the pressure in your arteries when your heart relaxes between beats. A blood pressure reading below 120/80 is considered normal.
Hypertension (high blood pressure) can affect anyone at any time and often catches people completely unaware – it happens when the blood pushes against the walls of your vessels with greater force. Chronic hypertension can cause damage to the walls of the blood vessels, and can lead to other cardiovascular problems and hardening of the arteries. Hypertension can occur in stages:
- Stage 1 hypertension is defined as a blood pressure reading that has a systolic pressure reading of 130-139 (the top number) over a diastolic pressure reading of 80-89 (the bottom number).
- Stage 2 hypertension is defined as a blood pressure reading of 140+/90+. As hypertension enters the crisis stage, readings can reflect blood pressure of 180+ over 120+.
Blood pressure can be more difficult to control for individuals with lupus because prednisone and other NSAIDS (non-steroidal anti-inflammatory drugs) can elevate it. Kidney disease may also affect your blood pressure. Hypertension can be one of the first symptoms for people who have lupus nephritis.
- Diagnostic tools include: routine blood pressure checks, often numerous times throughout the day over a period of time.
- Treatment may include: diet and weight modifications, limiting alcohol consumption, engaging in stress relief practices. Medications may include: thiazide diuretics, angiotensin-converting enzyme (ACE) inhibitors, angiotensin II receptor blockers (ARBs), alpha blockers, beta blockers, calcium channel blockers, vasodilators, renin inhibitors, and/or central acting agents.
Cholesterol, Atherosclerosis, and Coronary Artery Disease
First, it helps to understand a bit more about cholesterol. In simple terms, cholesterol is a kind of fat that is found in your blood. Your liver makes cholesterol, but you can also get it from the food you eat. Dairy products, meat, eggs and fish contain cholesterol. Our bodies need a certain amount of it, but within limits.
There are two types of cholesterol:
- High-density lipoprotein (HDL): HDL is often referred to as “good” cholesterol. HDL absorbs cholesterol and carries it to the liver so that it can leave the body. HDL can reduce the chance of developing heart disease and stroke.
- Low-density lipoprotein (LDL): LDL is considered “bad” cholesterol. LDL builds up in the walls of blood vessels, creating “plaques” and restricting blood flow to and from the heart and throughout the body. This condition leaves an individual vulnerable to angina, heart attack and stroke.
A buildup of bad cholesterol can lead to atherosclerosis and coronary artery disease. Atherosclerosis, also known as ASVD or premature coronary heart disease, is a form of arteriosclerosis where the artery wall thickens in result of a buildup of white blood cells. The buildup of the cells causes a fibrofatty plaque with LDL and affects the elasticity of the artery walls. Atherosclerosis can cause hardening and narrowing of the arteries, and after time, slowly blocks the artery from obtaining proper blood flow. It can cause strokes, heart attacks, and peripheral vascular disease. The risk of heart attack for women with lupus between the ages of 35-44 is 50 times greater than healthy women of the same age, and their risk of stroke is also up to nine times greater.
Individuals with lupus are also at risk for developing a condition known as dysfunctional pro-inflammatory HDL (piHDL). piHDL occurs when inflammation causes HDL to lose its antioxidant capacity, making an individual vulnerable to atherosclerosis because LDL is no longer protected from oxidative damage. Researchers believe that the presence of piHDL may indicate which individuals with lupus are at greater risk of developing atherosclerosis.
Coronary artery disease develops when the major blood vessels that carry blood to the heart become damaged and diseased over time if cholesterol levels are not kept in check.
- Diagnostic tools may include: a physical examination including a complete medical history, blood tests, ultrasounds, stress tests, heart scans, CT scans, and/or cardiac catheterization and angiogram.
- Treatment may include: diet and weight modifications, cholesterol-modifying medications such as statins; angiotensin-converting enzyme (ACE) inhibitors, angiotensin II receptor blockers (ARBs), beta blockers, calcium channel blockers, ranolazine, and/or nitroglycerine; surgery including angioplasty, stent implants, and/or coronary artery bypass grafting (CABG).
Staying Healthy
Be proactive when it comes to your health. Take charge of feeling good and pay heed when you do not. There are several things you can do to achieve your health goals:
- Maintain a healthy diet and achieve a healthy weight: Limit fat, sugar, and salt intake. Eat whole grains, fruits and vegetables – try to stay away from processed foods. Learn to make healthy changes without skimping on taste. Limit caffeine intake.
- Make sure you receive regular testing for diabetes.
- Practicing good oral hygiene is a MUST: Periodontal (gum) disease can often make one susceptible to heart disease. Keep your teeth and mouth clean and see your dentist regularly.
- Get plenty of rest and sleep.
- Get up and move: Many of us have sedentary lifestyles and sit too long. Make it a goal to get up and move around at least once every 20 minutes. If you cannot exercise regularly due to health, try to stand and stretchoccasionally to keep the blood flowing.
- Stop smoking and avoid secondhand smoke.
- Moderate alcohol intake: Happy hour can still be happy sipping on mineral water spiked with a lime while catching up with friends.
- Incorporate and practice stress-relief habits into your daily routine: Take a walk in nature. Perform gentle yoga. Meditate and practice mindfulness. Consider seeing a therapist to learn better coping skills. Develop a good support system of friends and family. Do more of what you love and celebrate life!
In Conclusion
Being proactive and taking your health seriously can go a long, long, way….possibly almost 800,000,000 heart beats or more away. By taking as many preventative measures as you can – without forsaking what you enjoy – you stand a greater chance of warding off unwanted illness and disease while protecting your precious heart. Understanding lupus, the risks involved, and maintaining a trusting, open, and honest relationship with your healthcare practitioner will also enable you to make and meet realistic healthcare goals, paving the way to a life worth celebrating!
References
About myocarditis. (2020). Myocarditis Foundation. Retrieved July 24, 2020 from https://www.myocarditisfoundation.org/about-myocarditis/?gclid=EAIaIQobChMI5dyAyo7p6gIVLP7jBx2uhwcAEAAYASAAEgLf6fD_BwE
Axford, J. (2015). The heart and lupus. Lupus UK. Retrieved July 24, 2020 from: https://www.lupusuk.org.uk/medical/gp-guide/clinical-aspects-of-lupus/the-heart and-lupus/
Brites, F., Martin, M., Guillas, I., & Kontush, A. (2017). Antioxidative activity of high-density lipoprotein (HDL): Mechanistic insights into potential clinical benefit. BBA Clinical, 66-77. doi: 10.1016/j.bbacli.2017.07.002. Retrieved July 24, 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5597817/
Cholesterol medications (statins). (2020). Johns Hopkins Lupus Center. Retrieved July 24, 2020 from https://www.hopkinslupus.org/lupus-treatment/common-medications-conditions/cholesterol-medications-statins/#:~:text=Studies%20have%20shown%20that%20people,often%20in%20people%20with%20lupus.
Coronary artery disease. (2020). Mayo Clinic. Retrieved July 24, 2020 from: https://www.mayoclinic.org/diseases-conditions/coronary-artery-disease/symptoms-causes/syc-20350613
Endocarditis. (2018). Mayo Clinic. Retrieved July 24, 2020 from: https://www.mayoclinic.org/diseases-conditions/endocarditis/diagnosis-treatment/drc-20352582
Erkan, D., Persad, P.,& Rusli, M. (2010). Top 10 series: lupus and cardiovascular disease. Hospital for Special Surgery. Retrieved from: https://www.hss.edu/conditions_minimize-risk-cardiovascular-disease-lupus.asp
Gavin, M. (2018). What’s cholesterol? KidsHealth. Retrieved July 24, 2020 from: https://kidshealth.org/en/kids/cholesterol.html
Gillinov, A.M. (2019). 5 things to do daily to keep your heart healthy. Cleveland Clinic. Retrieved July 24, 2020 from: https://health.clevelandclinic.org/5-things-to-do-daily-to-keep-your-heart-healthy/
How does lupus affect the cardiovascular system? (2020). Johns Hopkins Lupus Center. Retrieved July 24, 2020 from: https://www.hopkinslupus.org/lupus-info/lupus-affects-body/lupus-cardiovascular-system/
Ibrahim, A. & Siddique, M. (2020). Libman Sacks endocarditis. National Center for Biotechnology Information. Retrieved July 24, 2020 from https://www.ncbi.nlm.nih.gov/books/NBK532864/#:~:text=Libman%2DSacks%20(LS)%20endocarditis,antiphospholipid%20antibody%20syndrome%20(APS).
LDL and HDL cholesterol: “Bad” and “good” cholesterol. (2020). Centers for Disease Control and Prevention. Retrieved July 24, 2020 from https://www.cdc.gov/cholesterol/ldl_hdl.htm#:~:text=LDL%20(low%2Ddensity%20lipoprotein),for%20heart%20disease%20and%20stroke.
Lockshin, M. (2009). Unlocking the mystery of lupus: Lupus and the heart FAQs. Hospital for Specialty Surgery. Retrieved July 24, 2020 from: https://www.hss.edu/conditions_unlocking-mystery-lupus-heart-faqs.asp
McMahon, M., Grossman, J., Skaggs, B., FitzGerald, J., Shakian, L., Ragavendra, N., Charles-Schoeman, C., Watson, K., Wong, W., Chen, W., Gorn, A., Karpouzas, G., Weisman, M., Wallace, D., & Hahn, B. (2009). Dysfunctional pro-inflammatory high density lipoproteins confer increased risk for atherosclerosis in women with systemic lupus erythematosus. Arthritis & Rheumatology, 60(8), 2428-2437. doi: 10.1002/art.24677. Retrieved July 24, 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2753974/#:~:text=In%20summary%2C%20piHDL%20contribute%20to,low%20risk%20for%20subclinical%20atherosclerosis.
Pericarditis. (2018). Mayo Clinic. Retrieved July 24, 2020 from: https://www.mayoclinic.org/diseases-conditions/pericarditis/symptoms-causes/syc-20352510
Pulmonary hypertension. (2020). Mayo Clinic. Retrieved July 24, 2020 from: https://www.mayoclinic.org/diseases-conditions/pulmonary-hypertension/symptoms-causes/syc-20350697
Thomas, D. E. (2014). The lupus encyclopedia: A comprehensive guide for patients and families. Baltimore, MD: Johns Hopkins University Press.
What is blood pressure? (2008). Retrieved from: http://www.bloodpressureuk.org/BloodPressureandyou/Thebasics/Bloodpressure
What is high blood pressure? (2020). American Heart Association. Retrieved July 24, 2020 from https://www.stroke.org/-/media/data-import/downloadables/f/9/8/pe-abh-what-is-high-blood-pressure-ucm_300310.pdf
When is it high blood pressure? (n.d.). Blood Pressure UK. Retrieved July 24, 2020 from: https://www.healthline.com/health/what-considered-high-blood-pressure#healthyreading
Author: Liz Heintz
Liz Heintz is a medical research writer who received her BA in Communications, Advocacy, and Relational Communications from Marylhurst University in Lake Oswego, Oregon. She most recently worked for several years in the healthcare industry. A native of San Francisco, California, Liz now calls the beautiful Pacific Northwest home.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.



