Lupus and the Pancreas
Contents
- What is the Pancreas?
- Pancreatitis: Diagnosis, Symptoms and Treatment
- Preventing Pancreatitis
- Diabetes
- Diagnosing Diabetes
- Treating Diabetes
- Diabetes Prevention
- In Conclusion
Introduction
As of 2018, approximately 34 million Americans – 10% of the U.S. population – has diabetes. Unfortunately, that number is not a surprise considering we are living in a time when stress, “fast food” diets and lack of exercise all seem to work toward unhealthy lifestyles that set the tone for this particular disease. We skip stretching or a walk in favor of binge-watching Netflix and stay up way to late – only to start this whole process all over again in the morning.
Ugh. It’s no wonder our bodies suffer at some point.
For individuals with lupus, the rat-race lifestyle can catch up even more quickly because the body is considerably more vulnerable to stress and strain. An organ of particular vulnerability – though probably not even consciously considered – is the pancreas. Prone to inflammation, the pancreas can show signs of stress and neglect in the form of diabetes and even pancreatitis if we do not stop and think for a minute about the toll today’s frenetic lifestyle – along with possibly having lupus thrown in the mix – can take.
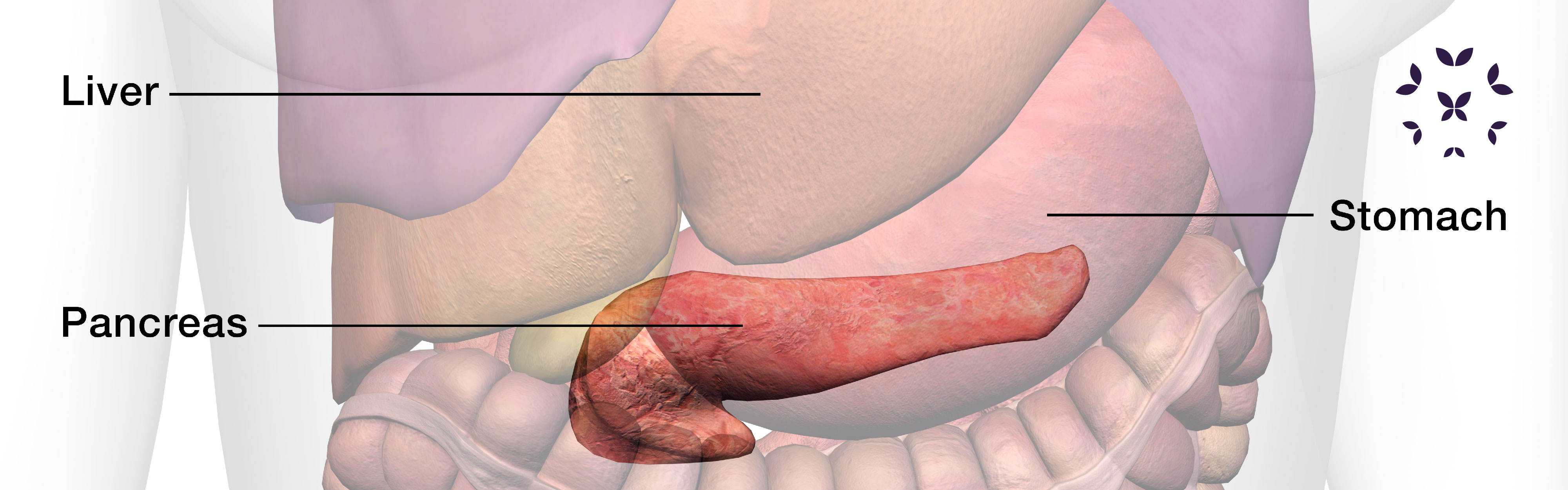
What is the pancreas?
Shaped like a flat pear and located in the upper left abdomen behind the stomach, the pancreas plays a vital role in two very different systems of the body, the digestive system and the endocrine system.
In its digestive role, it produces a wealth of enzymes and chemicals that do everything from neutralize the acid from your stomach, to those that digest fats (lipase), carbohydrates, starch (amylase), and proteins. It is the master digestive gland and does that job almost always without fanfare or problems
More commonly, issues with the pancreas occur from its other role as part of the endocrine system, the system responsible for the creation and regulation of hormones in your body. As an endocrine gland it produces and releases hormones that go directly into the blood system. The two main hormones produced by the pancreas are insulin, which lowers blood sugar, and glucagon, which raises blood sugar. A healthy pancreas performs the delicate dance between the two hormones with ease, regulating each to keep the body in perfect, dynamic balance.
Sometimes, however, that balance can be disrupted. Individuals with lupus know that lupus often affects major systems and organs of the body, and the pancreas is no exception. Pancreatic inflammation in individuals with SLE may occur as often as 30% of the time, though an individual may not complain of experiencing symptoms. Lupus-related pancreatic inflammation – pancreatitis – occurs most often in women in their 30s.
Pancreatitis: Diagnosis, Symptoms and Treatment
Pancreatitis can be acute (quick onset, lasting for days) or chronic (existing over many years) and is often the first symptom of lupus.
Causes: There are many possible ways for lupus to affect the pancreas, including:
- direct involvement of autoantibodies attacking tissue of the pancreas itself;
- inflammation due to the autoimmune activation of complement, or
- vasculitis – blood vessel inflammation – within the pancreas itself. SLE can produce antibody-antigen complexes that create micro-blood clots in parts of the body, like the kidneys and pancreas. This can produce localized damage to the pancreas.
However, because lupus-related pancreatitis is relatively uncommon, a healthcare practitioner will rule out other underlying causes of pancreatitis before attributing the symptoms to lupus, especially if an individual has yet to be diagnosed. These include:
- gallstones and/or blocked bile ducts;
- chronic and excessive alcohol use;
- abdominal surgery;
- certain medications (e.g. azathioprine, glucocorticoids, furosemide, isoniazid, metronidazole, sulindac);
- cigarette smoking;
- cystic fibrosis;
- genetics – a family history of pancreatitis;
- high calcium levels in blood (hypercalcemia);
- high triglyceride levels in the blood (hypertriglyceridemia);
- infection;
- abdomen injury; and
- pancreatic cancer.
If there are no underlying causes for pancreatitis and the individual experiencing symptoms has not been previously diagnosed with lupus yet exhibits other signs of active lupus, a healthcare practitioner may investigate for the autoimmune disease. A recent lupus diagnosis may still necessitate a test for pancreatitis even if no symptoms are present because it still may be inflamed.
Symptoms: Symptoms of acute pancreatitis may include the following:
- abdominal pain (the most common symptom);
- back pain;
- pain that gets worse after eating;
- nausea, vomiting, diarrhea, and/or cramping;
- fever;
- sweating;
- weakness;
- rapid pulse;
- tenderness to the touch;
- abdominal distension; and
- symptoms that mimic diabetes, but go away after diagnosis of pancreatitis and treatment (read more about diabetes below).
Symptoms of chronic pancreatitis may include the following:
- upper abdominal pain;
- unexplained loss of weight; and
- steatorrhea – fatty or oily, smelly stools.
If you experience any of the symptoms and a healthcare practitioner suspects pancreatitis, they may order the following tests to properly diagnose your symptoms:
- a complete medical history;
- a physical exam;
- blood tests to analyze blood amylase and lipase levels which typically increase when pancreatitis is present;
- an abdominal ultrasound; and
- a CT Scan.
Treatment: Individuals with lupus who have pancreatitis receive similar treatment as individuals with pancreatitis who do not have lupus. Treatment options may include:
- hydration, often intravenously;
- a restricted, low-fat diet, which allows the pancreas to rest and heal;
- stopping alcohol consumption; and
- cessation of any antibiotics, which may have been prescribed.
Individuals with lupus, however, who have pancreatitis may be treated with corticosterioids with or without cytotoxic agents, including azathioprine, cyclophosphamide, and mycophenolate mofetil. A Texas Tech University Health Sciences Center study in 2014 noted that while the use of steroid treatments for acute pancreatitis in individuals with lupus is controversial “because of [a] steroid-induced toxic effect … this concern is regarded as minimal. Because the immunosuppressive effect of steroids can significantly improve prognosis in patients with acute pancreatitis …” (p. 3). For individuals with lupus, the benefit outweighs the risks.

Preventing Pancreatitis
While individuals with lupus are predisposed to inflammation throughout the body, and while pancreatitis may not be altogether unavoidable for some, there are precautions that can be taken to minimize the risk of occurrence:
- Alcohol in moderation: Limit or even avoid consumption.
- Eat a low-fat diet: Avoid greasy foods (deep fried foods make look can often be a trigger) and full-fat dairy products. Eat a diet rich in whole grains, fruits, and vegetables. Skip the crash, fad diets – just do what has been determined and deemed healthy by the healthcare community. They are the experts!
- Exercise: We have said it more than once here. Regular exercise – while acknowledging your limitations and remaining physically active in a way that suits you – is key to maintaining a healthy weight and improving overall well-being!
- Avoid smoking: Too many health risks come with smoking. It is just not worth it.
Working with a trusted healthcare practitioner is key to avoiding risk and achieving optimal health – they know what to do in order to maintain as healthy as possible.
Diabetes
As mentioned earlier, the pancreas is responsible for making insulin and maintaining healthy blood sugar levels. What happens when there is a breakdown in that process? If the pancreas produces insufficient levels of insulin – or stops producing it at all – and if the body fails to use the insulin that is produced properly, glucose stays in the bloodstream and never reaches the cells that rely on it for energy. Blood sugar levels remain too high, and a diabetes diagnosis may be imminent.
There are three types of diabetes:
- Individuals have type 1 diabetes if they are unable to produce insulin. It is typically diagnosed at a young age and the individual must rely on taking insulin every day.
- Individuals have type 2 diabetes if their bodies not use nor make insulin efficiently. An individual may receive a diagnosis at any time in life, but typically when they are middle-aged or older.
- Pregnant women may develop gestational diabetes that usually goes away after their baby is born, though sometimes it is a precursor to developing type 2 diabetes later on.
It is no wonder that individuals with lupus are at greater risk of developing diabetes – especially those treated with high-dose glucocorticoids. This medication interaction can increase diabetes risk due to chronic inflammation that occurs in individuals with lupus that can alter insulin homoeostasis, contributing to insulin resistance.
Symptoms of diabetes may include:
- increased thirst and/or hunger;
- frequent urination;
- fatigue;
- inexplicable weight loss;
- irritability;
- blurred vision;
- slow-healing sores; and
- frequent infections, especially of skin, mouth/gums, and vagina.
Along with having lupus, individuals may be at greater risk for developing diabetes if:
- BMI (Body Mass Index) is higher than 25.
- There is a family history of diabetes.
- An individual has high cholesterol, hypertension, a sedentary lifestyle, a history of heart disease and/or polycystic ovary syndrome.
- An individual is older than 45.
- Gestational diabetes has occurred in the past.
- An individuals has been diagnosed with pre-diabetes.
Diagnosing Diabetes
Diagnostic testing may include the following:
- AC1 blood tests: Test results of equal to or greater than 6.5% indicate diabetes, while less than 5.7% is considered normal.
- Fasting blood sugar tests: Two tests indicating a blood-sugar level of 126 mg/dl indicates diabetes. Having less than 100 mg/dl is considered normal.
- Random blood sugar tests: Equal to or greater than 200 mg/dl indicates diabetes, while less than this is considered normal.
- Oral glucose intolerance tests: Equal to or greater than 200 mg/dl indicates diabetes while less than this is considered normal.
- A zinc transporter 8 autoantibody (ZnT8Ab) test.
- Urine tests.
Treating Diabetes
Treating diabetes in individuals with lupus is much like treating it in individuals who do not have lupus though closer monitoring by a healthcare practitioner may be advised. Monitoring blood sugar levels several times daily will be key to working with a healthcare practitioner to make sure they are implementing the correct and adequate treatment plan.
Type 1 diabetes treatment includes:
- Injectable, oral, or inhaled insulin daily. A healthcare practitioner will help set up goals and determine which product and dose is best.
- Diet modifications.
- Exercise.
- Maintaining a healthy weight.
Type 2 diabetes medication interventions include:
- drugs that increase insulin production by the pancreas;
- drugs that decrease sugar absorption by the intestines;
- drugs that decrease sugar production by the liver and improve insulin resistance;
- drugs that enhance how the body uses insulin;
- drugs that increase insulin production by the pancreas and reduce sugar production by the liver;
- drugs that inhibit the reabsorption of glucose by the kidneys and increase glucose excretion in urine;
- synthetic hormones that lower blood sugar levels after eating; and
- recently FDA-approved drugs that combine types of diabetes medications into one.
Many individuals with type 2 diabetes can manage their diabetes through diet and exercise alone. Sometimes, however, a healthcare practitioner may prescribe insulin (see above) and oral drugs to maintain normal blood sugar levels.
Diabetes Prevention
Type 1 diabetes is difficult to prevent since its onset often occurs in childhood and may be hereditary. Type 2 diabetes, however, is a bit easier to prevent though a little trickier for individuals with lupus and if taking high-dose glucocorticoids. Glucocorticoids can interfere with glucose metabolism.
Individuals with lupus who have diabetes also have a greater risk of developing other diabetic complications such as neuropathy and renal insufficiency, making it even more imperative for individuals with lupus to work diabetes prevention into their overall health goals.
Type 2 diabetes prevention for individuals with lupus include:
- Hydroxychloroquine (Plaquenil): Scientists found that individuals with lupus who take a cumulative dose of hydroxychloroquine (Plaquenil) had a 74% lower risk of diabetes than individuals taking high-dose glucocorticoids alone.
- Exercise: Both aerobic exercise and resistance exercise are beneficial to getting and staying healthy. Individuals with lupus and its related symptoms and co-diseases may find it difficult to exercise strenuously and regularly, making it even more important to talk with a trusted healthcare practitioner to help develop an exercise plan that can be managed and maintained – there are so many options out there these days that enhance both sound body and mind!
- Diet: Work with a healthcare practitioner to develop a healthy and delicious diet that will help control blood sugar levels as well as help achieve and maintain a healthy weight/BMI. A diet should include plenty of fiber and whole grains. Once again, skip those Hollywood fad diets!
- See a healthcare practitioner regularly for checkups: Make sure to tell a practitioner right away if experiencing any changes in health and/or general well-being.
In Conclusion
It goes without saying to never take health and well-being for granted. Take a minute and breathe. Be mindful for a moment and start paying attention to what goes into your body at every meal. Can a salad be ordered instead of a cheeseburger or an apple instead of fries? Start considering how down-time is spent – can Netflix wait until after a short walk around the block or some simple stretches? This may be a great time to examine the choices made in an effort to save time and instead spend some time making some important life changes. Our bodies – in particular our pancreas – will thank us for the thoughtful consideration!
References
Chen, Y., Lin, C., Lan, T., Chen, H., Chang, S., Chen, Y., Wang, J., Hung, W., Lan, J., & Chen, D. (2015). Hydroxychloroquine reduces risk of incident diabetes mellitus in lupus patients in a dose-dependent manner: A population-based cohort study. Rheumatology, 54(7), 1244-1249. doi: 10.1093/rheumatology/keu451. Retrieved August 10, 2020 from: https://www.ncbi.nlm.nih.gov/pubmed/25587177
Dallas, M. (2, January 2020). 5 ways to prevent pancreatitis and EPI. Everyday Health. Retrieved August 10, 2020 from: https://www.everydayhealth.com/hs/exocrine-pancreatic-insufficiency/prevent-pancreatitis-and-epi/
Diabetes. (2018). Mayo Clinic. Retrieved August 10, 2020 from: https://www.mayoclinic.org/diseases-conditions/diabetes/symptoms-causes/syc-20371444
Diabetes: 5 tips for taking control. (2019). Mayo Clinic. Retrieved August 10, 2020 from: https://www.mayoclinic.org/diseases-conditions/type-2-diabetes/in-depth/diabetes-prevention/art-20047639
Favarato, M. (2015). Lupus-associated pancreatitis: Clinical aspects. Journal of Rheumatic Diseases and Treatment, 1(3). Retrieved August 10, 2020 from: https://clinmedjournals.org/articles/jrdt/journal-of-rheumatic-diseases-and-treatment-jrdt-1-022.pdf
Hyperamylasemia (high blood amylase level). (n.d.). Chemocare. Retrieved August 10, 2020 from http://chemocare.com/chemotherapy/side-effects/hyperamylasemia-high-amylase.aspx#:~:text=Hyperamylasemia%20may%20be%20described%20as,begin%20the%20digestion%20of%20starches.
Jia, Y., Ortiz, A., Mccallum, R., Salameh, H., & Serrato, P. (2014). Acute pancreatitis as the initial presentation of systematic lupus erythematosus. Case Reports in Gastrointestinal Medicine, 2014, Article 571493. doi: 10.1155/2014/571493. Retrieved August 10, 2020 from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4150433/pdf/CRIGM2014-571493.pdf
Pancreatitis. (n.d.). Mayo Clinic. Retrieved August 10, 2020 from: https://www.mayoclinic.org/diseases-conditions/pancreatitis/symptoms-causes/syc-20360227?p=1
Statistics about diabetes. (2018). American Diabetes Association. Retrieved August 10, 2020 from: https://www.diabetes.org/resources/statistics/statistics-about-diabetes#:~:text=Prevalence%3A%20In%202018%2C%2034.2%20million,of%20the%20population%2C%20had%20diabetes.&text=Undiagnosed%3A%20Of%20the%2034.2%20million,and%207.3%20million%20were%20undiagnosed.
The pancreas and its functions. (n.d.). Columbia Surgery. Retrieved August 10, 2020 from: http://columbiasurgery.org/pancreas/pancreas-and-its-functions
Thomas, D. E. (2014). The lupus encyclopedia: A comprehensive guide for patients and families. Johns Hopkins University Press.
What is diabetes? (2016). National Institute of Diabetes and Digestive and Kidney Diseases. Retrieved August 10, 2020 from: https://www.niddk.nih.gov/health-information/diabetes/overview/what-is-diabetes
Author: Liz Heintz (updated August, 2020)
Liz Heintz is a technical and creative writer who received her BA in Communications, Advocacy, and Relational Communications from Marylhurst University in Lake Oswego, Oregon. She most recently worked for several years in the healthcare industry. A native of San Francisco, California, Liz now calls the beautiful Pacific Northwest home.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.