Vasculitis and Lupus
Though relatively rare in general – possibly affecting as few as one individual in a million – vasculitis can pose health risks in individuals with SLE where it reportedly affects between 11% and 36% of those with lupus.
- Introduction
- What causes vasculitis?
- Antibody Activity in Vasculitis
- What are the symptoms of vasculitis?
- How is vasculitis diagnosed and treated?
- Vasculitis Risks for Individuals with Systemic Lupus Erythematosus (SLE)
- What is the prognosis for vasculitis?
- In Conclusion
Introduction
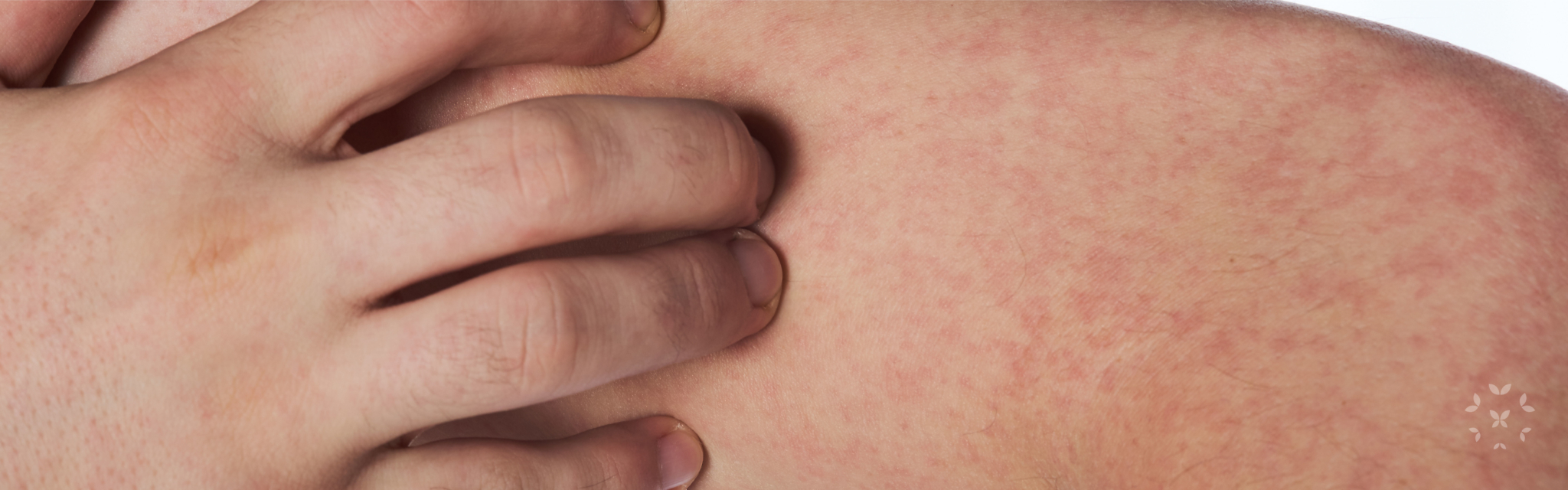
Vasculitis is the general term for a condition that occurs when the lining of blood vessels become inflamed. More specifically, vasculitis is classified by the size of the vessels affected and where they are located in the body – there are well over a dozen types of vasculitis that can affect the small tiny veins and capillaries of the skin (cutaneous vasculitis) and eyes (retinal vasculitis) or even larger arteries such as the aorta (isolated aortitis). Vasculitis can also be systemic, affecting entire systems such as the central nervous system (central nervous system vasculitis). The American College of Rheumatology (ACR) notes that it is thought to be an autoimmune disease. It is relatively indiscriminate, affecting both men and women of any age depending on the specific type of vasculitis that develops. Even children can have some forms of vasculitis such as IgA (also known as Henoch-Schönlein purpura), which affects the small vessels of the kidneys, joints, skin or intestines, particularly in boys, and Kawasaki disease, which primarily affects children from ages 6 months to 5 years, causing inflammation of the mucus membranes, lymph nodes or coronary arteries.
There is a connection between vasculitis and vascular disease such as atherosclerosis. A 2009 review article published in the journal Clinical and Experimental Immunology discusses how some forms of vasculitis such as Takayasu arteritis and Kawasaki disease, accelerated atherosclerosis can occur, especially in younger individuals. Some vasculitis in which specific antibodies develop can also exacerbate the occurrence of cardiovascular disease. Individuals who also have renal impairment and increased levels of C-reactive protein are also at greater risk for developing atherosclerosis as a result of vasculitis.
What causes vasculitis?
It is unclear about exactly what causes vasculitis. The American College of Rheumatology (ACR), however, cites the following possible factors:
- Genetic: A specific gene may be responsible.
- The presence of other rheumatic diseases: Individuals with rheumatoid arthritis (RA), systemic lupus erythematosus or Sjögren’s syndrome may be more susceptible to developing inflammation in blood vessels.
- Serious, chronic infections: Viruses such as hepatitis B and hepatitis C can cause vasculitis.
- Adverse reactions to medications: The Vasculitis Foundation lists the following drugs that have been known to induce vasculitis: penicillin, cephalosporin, sulfonamide, loop and thiazide-type diuretics used to control blood pressure, phenytoin and allopurinol.
- Blood cancers – the Arthritis Foundation notes that cancers such as leukemia and lymphoma may trigger vasculitis.
Antibody Activity in Vasculitis
As with autoimmune diseases such as lupus, when an individual develops vasculitis, their body starts making antibodies to fight as though it is fighting a foreign invader rather than itself. When an individual suffers from vasculitis, there can be very specific antibodies that are present. According to a 2015 article published in the journal Frontiers in Immunology, researchers have been successful in discovering several antibodies that are present in vasculitis that affects small vessels and capillaries. There are no antibodies present in medium or large vessel vasculitis that have been found to be particularly helpful in diagnoses, however.
The antibodies that researcher have discovered in small vessel vasculitis include:
- Antineutrophil Cytoplasmic Antibodies (ANCA): The presence of ANCA is a diagnostic indicator for vasculitis that may affects small vessels in conditions such as granulomatosis with polyangiitis, eosinophilic granulomatosis with polyangiitis or microscopic polyangiitis. According to the Frontiers in Immunology article, ANCA is present in up to 90% of the individuals affected by these forms of vasculitis. An atypical form of ANCA can also be found in individuals with ulcerative colitis, inflammatory bowel disease and RA.
- Anti-Lysosome Associated Membrane Protein-2 Antibodies (LAMP-2): Considered a subset of ANCA, LAMP-2 can also be present in granulomatosis with polyangiitis, eosinophilic granulomatosis with polyangiitis, microscopic polyangiitis or even vasculitis that affects an individual’s renal system.
- Cryoglobulins: Cryoglobulins are broken into three types including Type I which occurs without rheumatoid factor activity, Type II which occurs with rheumatoid factor activity and Type III which is often present when an individual has a connective tissue disease or chronic viral infections such as hepatitis C. Cryoglobulins can be present in cryoglobulinemic vasculitis, central nervous system vasculitis and pulmonary vasculitis.
- Anti-Glomerular Basement Membrane Antibodies: These antibodies are present in pulmonary capillaries or glomerular capillaries, which are found in the kidneys.
- Anti-C1q Antibodies: Anti-C1q is a biomarker for urticarial vasculitis and hypocomplementemic urticarial Vasculitis, which may affects not only the skin, but the eyes, lungs, joints or kidneys as well.
- Anti-Endothelial Cell Antibodies (AECA): These antibodies have been found with Takayasu arteritis, giant cell arteritis, polyarteritis nodosa, Kawasaki disease, Behcet’s disease, granulomatosis with polyangiitis, microscopic polyangiitis, and eosinophilic granulomatosis with polyangiitis. Researchers have yet to discover, however, how useful these antibodies may be.
- Anti-Ferritin Antibodies: These antibodies are found in Giant Cell Arteritis, Takayasu arteritis and PMR. Anti-ferritin antibodies, however, are also found in individuals with SLE and atherosclerotic disease so it is unclear yet how these markers can be useful in distinguishing between vasculitis and these other conditions.
What are the symptoms of vasculitis?
Like with any illness including lupus, how an individual experiences symptoms can be unique from anyone else. Symptoms can come on suddenly and intensely or develop slowly over time and can also be life-threatening. Symptoms can also be very general as though an individual is suffering from the flu or common cold or can be very specific, unlike anything the individual has experienced before.
The Arthritis Foundation lists the following as the more common symptoms of vasculitis:
- Fever
- Loss of appetite
- Weight loss
- Fatigue
- General aches and pains
Since these symptoms are very broad and can cover a range of conditions, it is important to take note and let a healthcare practitioner know right away if any seem to worsen, persist or cause alarm. While an individual with a chronic healthcare condition may attribute these symptoms to how they generally feel – or in the case of lupus, a flare – it is extremely important not to take anything for granted and let a healthcare practitioner know right away.
The Arthritis Foundation and Johns Hopkins also list the following symptoms that affect organs and major systems of the body:
- Skin: Red spots or bumps (also known as purpura) and other skin manifestations.
- Joints: Stiffness or aching, much like with arthritis.
- Lungs: Difficulties breathing, inexplicable coughing, coughing up blood.
- Gastrointestinal tract: Stomach pain and discomfort, sores in the mouth, pancreatitis, etc.
- Eyes: Blurred vision, itchy and burning eyes, redness and sensitivity to light.
- Brain: Cognitive issues such as feeling foggy and unable to focus or concentrate,
- Nerves: Numbness, weakness, sharp pain or tingling especially in the arms and legs.
- Kidneys: The presence of red blood cells in urine and protein loss in urine.
- Sinuses: Persistent sinus infections, congestion, inflammation or even hearing loss.
Many of these symptoms can be due to constricted blood flow and potentially cause organ damage which increases the urgency to see a healthcare practitioner right away.
Vasculitis Risks for Individuals with Systemic Lupus Erythematosus (SLE)
Though rare, individuals with systemic lupus erythematosus (SLE) can develop vasculitis. Children are sometimes even diagnosed with juvenile SLE (JSLE) after they are diagnosed with vasculitis. Vasculitis can also be a symptom of an SLE flare in both adults and children. Dr. Daniel Wallace, author of “The Lupus Book” notes that the most common types of vasculitis that may affect individuals with SLE are in the skin (cutaneous vasculitis), the gastrointestinal tract (lupus mesenteric vasculitis) and the eyes (retinal vasculitis), though vasculitis can also occur in other areas such of the body such as the kidneys as well.
Cutaneous Vasculitis
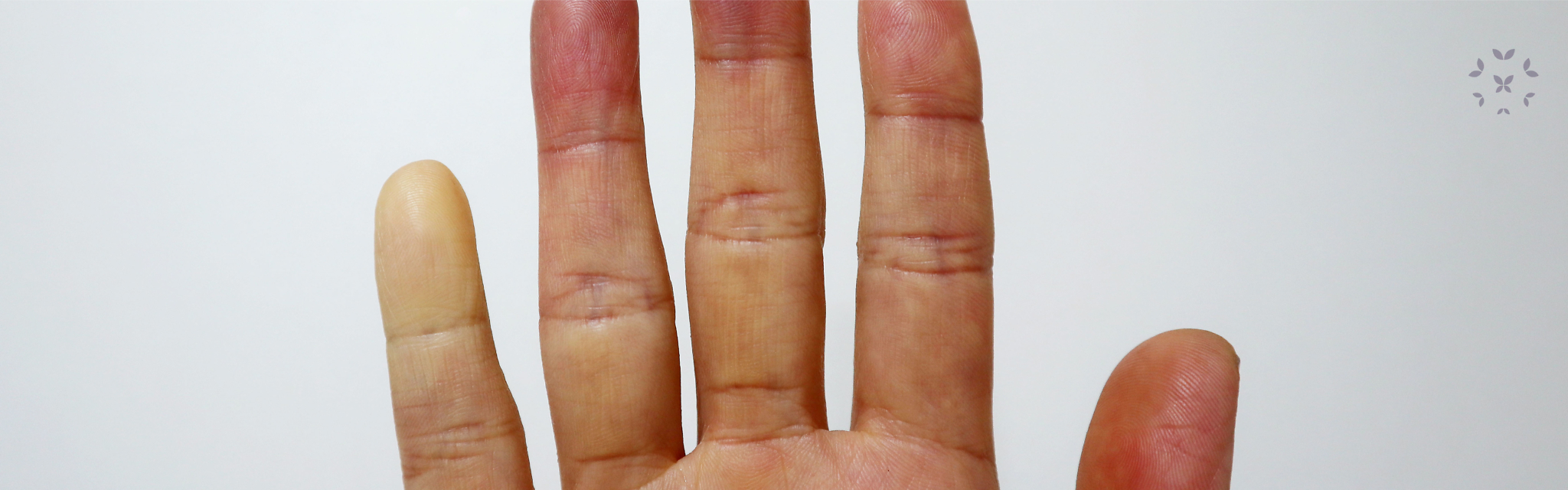
Cutaneous vasculitis involves the inflammation of the small blood vessels of the skin and is the most common type of vasculitis in individuals with lupus. Much like cutaneous lupus, cutaneous vasculitis is also characterized by lesions that appear on the skin, specifically red, raised bumps. A 2018 article published the journal Lupus states that cutaneous vasculitis may occur in up to 70% of individuals with SLE. If an individual with SLE also has the overlap disease Sjögren’s syndrome, there is even greater risk of developing cutaneous vasculitis. Individuals with SLE and cutaneous vasculitis also are more at risk of developing Raynaud’s phenomenon, malar rash, and photosensitivity.
There may also be a correlation between vasculitis and antiphospholipid syndrome (APS) in individuals with SLE. In the 2018 Lupus article, researchers noted that individuals who were diagnosed with cutaneous vasculitis were later diagnosed with APS. These diagnoses are a “necessary first step on the road toward understanding why and how [cutaneous vasculitis] occurs.”
Lupus Mesenteric Vasculitis
In a 2010 article published in the World Journal of Gastroenterology, researchers Xin-Ping Tian and Xuan Zhang noted that up to 40% of individuals with active SLE experience abdominal pain and that lupus mesenteric vasculitis (vasculitis of the gastrointestinal tract) is one of the main causes. Symptoms can range from the mild discomfort of digestion issues such as bloating, more acute symptoms such as rebound pain or more life-threatening symptoms such as intestinal perforation and internal bleeding.
Retinal Vasculitis
Researchers in a 2016 review article published in the Saudi Journal of Ophthalmology cited that approximately one-third of individuals with SLE also experience eye or ocular complications, especially at the onset of SLE. One of these complications is retinal vasculitis which occurs when the vessels of the retina become inflamed. It is diagnosed by an ophthalmologist by dilating the eye and conducting an examination or possibly performing a special type of angiogram. Often, an individual will not experience any symptoms.
Juvenile SLE (JSLE) and Vasculitis
Vasculitis is a common feature of JSLE and is sometimes the first indication that a child has autoimmune disease. The body of research and reporting is small and, therefore, it is unclear how many children may be affected. Researchers of a 2019 review article published in the journal Frontiers in Pediatrics cite that vasculitis may occur in up to approximately 22% of children with JSLE. Typically, the vasculitis manifests as cutaneous vasculitis. Cutaneous vasculitis often presents on the legs and arms of children with JSLE and occurs more often in these children than in adults with SLE. Though more rare, visceral vasculitis can occur in children with JSLE and often poses a potentially life-threatening condition as permanent organ damage may occur quickly.
Lupus Nephritis and Renal Vasculitis
It is important to note that because individuals with SLE often have lupus nephritis, renal vasculitis may also occur. Lupus nephritis and renal vasculitis are the two main causes of renal failure in individuals with conditions such as SLE. Glomerulonephritis is the inflammation of the tiny filters of the kidneys and according to a 2011 article published in the journal Medicine, is the “main renal manifestation of vasculitis” in individuals with SLE. Glomerulonephritis is often caused by ANCA-associated vasculitis (AAV).
How is vasculitis diagnosed and treated?
A rheumatologist can diagnose and treat vasculitis.
Diagnosing Vasculitis
The Arthritis Foundation lists the following vasculitis diagnostic tools depending on the type of vasculitis and the symptoms an individual is experiencing:
- Biopsy
- Blood and/or urine laboratory tests
- Angiogram
- Echocardiogram
- Chest x-ray
- Lung function test
- Abdominal ultrasound
- Computed tomography (CT) scan
- Magnetic resonance imaging (MRI)
- Blood pressure measurements
- Electrocardiogram (EKG)
Wallace also adds the following as diagnostic tests for vasculitis:
- Spinal tap
- Magnetic resonance angiogram
- Single photon emission computerized tomography (SPECT) scan
- Positron emission tomography (PET) scan
A biopsy of the affected area is typically the best, most conclusive way to diagnose vasculitis.
Treating Vasculitis
The Arthritis Foundation lists the following as treatment for vasculitis depending on the severity:
- Over-the-counter pain and/or anti-inflammatory medicines (acetaminophen, ibuprofen, aspirin, naproxen)
- Corticosteroids (prednisone, prednisolone, methylprednisolone)
- Anti-rheumatics/immunosuppressants (azathioprine, methotrexate, cyclophosphamide)
In mild cases of vasculitis that mainly affect the skin, a doctor may not prescribe anything unless the individual is experiencing discomfort or they may prescribe the over-the-counter medications used to reduce pain and inflammation as listed above. The more severe the vasculitis, the more aggressive the treatment at which time a corticosteroid or immunosuppressant may be prescribed, sometimes intravenously.

What is the prognosis for vasculitis?
While there currently is no cure, advancements in technology and research have resulted in better treatments for vasculitis. Under the care of a healthcare practitioner, remission from vasculitis is possible when it is properly diagnosed, treated and managed and flares are caught early.
The Arthritis Foundation notes that maintaining healthy habits and practicing self-care can be beneficial when managing vasculitis. They recommend the following:
- Eating healthy and maintaining a balanced diet.
- Getting regular exercise.
- Making sure all vaccinations are up-to-date
- Building a strong support system.
If an individual with lupus also has vasculitis, a healthcare practitioner will tailor treatment plans that take both conditions and an individual’s lupus activity into consideration. The Mayo Clinic also adds that understanding vasculitis by educating oneself about their specific condition and adhering to treatments plans will help an individual to cope with and manage their vasculitis.
In Conclusion
Keeping the lines of communication open between an individual and their healthcare practitioner, advocating for oneself, understanding what it means to have vasculitis along with other conditions such as lupus and paying attention to the signs and signals our bodies give us when something is wrong will help an individual can make sure they receive the utmost in care in order to stay healthy and feel their best.
References
7 things you should know about vasculitis. (n.d.). Retrieved January 13, 2020 from https://health.clevelandclinic.org/7-things-you-should-know-about-vasculitis/
American College of Rheumatology. (2020). Vasculitis. Retrieved January 13, 2020 from https://www.rheumatology.org/I-Am-A/Patient-Caregiver/Diseases-Conditions/Vasculitis
Arthritis Foundation. (n.d.). Vasculitis. Retrieved January 13, 2020 from https://www.arthritis.org/diseases/vasculitis
Cleveland Clinic. (2020). IgA vasculitis (Henoch-Schönlein purpura). Retrieved January 13, 2020 from https://my.clevelandclinic.org/health/diseases/14893-iga-vasculitis-henoch-sch%C3%B6nlein-purpura
De Souza, A. (2015). Autoantibodies in systemic vasculitis. Frontiers in Immunology. Retrieved January 13, 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4406058/pdf/fimmu-06-00184.pdf
Gheita, T., Abaza, N., Sayed, S., El-Azkalany, G., Fishawy, H., & Eissa, A. (2018). Cutaneous vasculitis in systemic lupus erythematosus patients: Potential key players and implications. Lupus, 2018(27) 738-743. doi: 10.1177/0961203317739134
Johns Hopkins Vasculitis Center. (2020). Symptoms of vasculitis. Retrieved January 13, 2020 from https://www.hopkinsvasculitis.org/vasculitis/symptoms-vasculitis/
Mayo Clinic. (2020). Glomerulonephritis. Retrieved January 13, 2020 from https://www.mayoclinic.org/diseases-conditions/glomerulonephritis/symptoms-causes/syc-20355705
Rosenbaum, J., Sibley, C., & Lin, P. (2016). Retinal vasculitis. Current Opinions in Rheumatology. Retrieved January 13, 2020 from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4893321/pdf/nihms-789799.pdf
Shoughy, S., & Tabbara, K. (2016). Ocular findings in systemic lupus erythematosus. Saudi Journal of Ophthalmology. Retrieved January 13, 2020 from https://www.sciencedirect.com/science/article/pii/S1319453416000242
Smith, E., Lythgoe, H., & Hedrich. (2019). Vasculitis in juvenile-onset systemic lupus erythematosus. Frontiers in Pediatrics. Retrieved January 13, 2020 from https://www.frontiersin.org/articles/10.3389/fped.2019.00149/full
Tervaert, J. (2009). Translational mini-review series on immunology of vascular disease: Accelerated atherosclerosis in vasculitis. The Journal of Translational Immunology. Retrieved January 13, 2020 from https://onlinelibrary.wiley.com/doi/pdf/10.1111/j.1365-2249.2009.03885.x
Tian, X., & Zhang, X. (2010). Gastrointestinal involvement in systemic lupus erythematosus: Insight into pathogenesis, diagnosis and treatment. World Journal of Gastroenterology. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2890936/pdf/WJG-16-2971.pdf
Vasculitis Foundation. (n.d.). General vasculitis. Retrieved January 13, 2020 from https://www.vasculitisfoundation.org/
Wilcocks, L., Jones, Rachel, & Jayne, D. (2011). Lupus nephropathy and vasculitis. Medicine, 39(8).
Author: Liz Heintz
Liz Heintz is a technical and creative writer who received her BA in Communications, Advocacy, and Relational Communications from Marylhurst University in Lake Oswego, Oregon. She most recently worked for several years in the healthcare industry. A native of San Francisco, California, Liz now calls the beautiful Pacific Northwest home.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

