Lupus and Anticoagulants
For those living with lupus, blood clots can be a significant health risk, possibly leading to strokes, heart attacks, pulmonary thromboses and especially kidney damage. Treating for these conditions means that many with SLE add anticoagulants (blood thinners) to their lengthy list of medications. What could this mean for you? Read on to find out!
Note: This article is for informational purposes only. As always, consult your healthcare provider before making any changes to your treatment plans!
article is for iThis article is for informational purposes only. As always, consult your healthcare provider before making any changes to your treatment plans!
Introduction
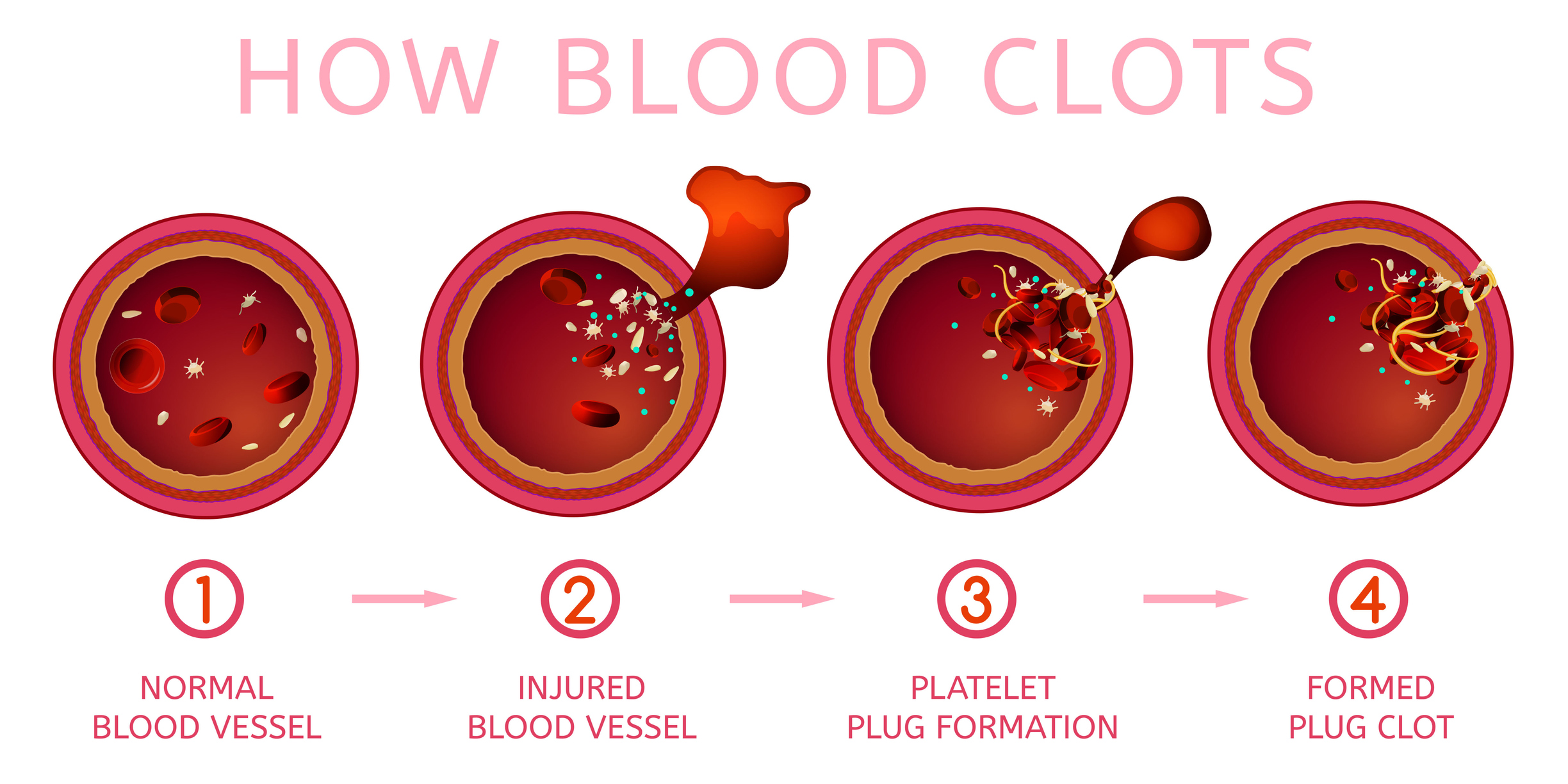
Forming blood clots is a healthy and necessary way for the body to stop the bleeding that occurs during injuries or whenever blood vessels are damaged. This happens all the time. Whenever you bump an elbow or bend your knee, there is the possibility that tiny blood vessels are damaged and begin bleeding. You usually never notice this because the bleeding is minor and blood clots form very quickly.
As a note, those with hemophilia or other bleeding disorders definitely notice these daily minor injuries because their blood has difficulty clotting normally.
With lupus, when blood clots form where they are not supposed to – a condition called thrombosis – they can block blood vessels to healthy tissues and organs. These can be very small clots that, again, may go unnoticed for a while, as is often the case with kidney damage. Yet, they can also block larger vessels of the heart causing heart attacks (myocardial infarction), or the lungs causing pulmonary embolisms, or the brain causing strokes.
One study found that around 16% of all SLE patients had experienced a “thrombotic event” during the 5 year period of the study.
So, what exactly are anticoagulants, and how are they used to treat lupus and prevent the damage due to thromboses? Read on to find out.
Anticoagulants and Lupus
The process of how the body creates blood clots to stop bleeding is actually quite complex. It involves blood cells called platelets (thrombocytes) and special proteins, called clotting factors (like fibrin, fibrinogen, prothrombin and others). These float around the blood stream waiting, at a moment’s notice, to be triggered to form the tiny “nets” of fibers and platelets that plug the damaged areas and stop the bleeding. Again, this is a process that happens daily under normal circumstances, and is a necessary reacti0n to injuries great and small.
.
Why can blood clots become an issue for those living with lupus?
There are several reasons why abnormal blood clotting is a significant problem for those living with lupus.
- The inflammation caused by lupus can directly damage blood vessels (vasculitis) which then can trigger blood clots to form and reduce the blood supply to vital organs, increasing the risk for heart or kidney involvement.
- Lupus can produce so many autoantibodies that the resulting antigen-antibody complexes (micro-clots) can lead to blockages of small blood vessels, especially in areas where the most delicate capillaries are found, like the kidneys.
- Some medications, specifically glucocorticoids, which are commonly used to treatment SLE, have been associated with an increased risk of thrombosis.
- Also, the use of immunosuppressive drugs, can increase the risks for infection, and this in turn can lead to an increase in blood clots.
- Finally, and most significantly, 30% to 50% of those with lupus also create specific antibodies called antiphospholipid antibodies. These antibodies disrupt the normal clotting process, and can force the body to over-react into forming blood clots too quickly. In people with lupus and antiphospholipid syndrome, anticoagulants are not only essential, but lifesaving.
These autoantibodies have been given the unfortunately confusing name, “lupus anticoagulants.” These are very different from the anticoagulants that are used to treat lupus … and are the topic of this article. For more on lupus anticoagulants as part of antiphospholipid syndrome
Note: Lupus can cause other types of abnormal blood clotting. For example, from 25% to 50% of those living with lupus can develop mild thrombocytopenia, which means they produce too few platelets and this can cause excessive bleeding.
.
.
What kinds of anticoagulants are used in treating lupus?
Anticoagulants are designed to prevent blood clots in different ways – at different stages of this very complex process. Choosing the best anticoagulant requires careful consideration of the individual patient. The most common anticoagulants for those with lupus include:
- Aspirin, which is considered an antiplatelet drug and may be sufficient for many circumstances. It is used by millions in low doses to “thin the blood,” and works by preventing platelets from clumping together to form the clot. They are often taken by those who have a history of heart attack or stroke.
- Warfarin (also known as Coumadin). It is a vitamin K antagonist and is the most commonly prescribed anticoagulant for those with SLE. Warfarin works by blocking vitamin K which is important in producing the prothrombin clotting factor. Warfarin is not recommended for pregnant women.
- Direct Oral Anticoagulants (DOACs). These include apixaban, dabigatran and rivaroxaban. They inhibit different stages of the clotting process and are considered safe and effective alternatives to vitamin K antagonists.
- Heparin inhibits the clotting factors thrombin and fibrin, and is only given as an injection – usually used in hospital situations or for pregnant women who are diagnosed with antiphospholipid antibodies.
- Hydroxychloroquine (Plaquenil), an antimalarial that is used by many SLE patients, has also been shown to reduce the risk of blood clots for some.
What are the most important considerations for those living with lupus?
For those with lupus who are at risk for the tissue and organ damage that can come from thrombosis, there are some important things to consider:
- Stick to treatment plans! By reducing the risk of flares and taking the medications that reduce overall inflammatory and immune responses, there is less likelihood of the vascular damage or antibody production that can cause unhealthy blood clots from forming in the first place.
- Get regular blood work done, including complete blood counts (CBCs). This will indicate several possible blood issues associated with lupus, especially abnormal platelet counts.
- You may need to see a hematologist, a specialist in blood disorders.
- Do not smoke or drink alcohol when taking anticoagulants. Smoking can increase the risk of blood clots, especially related to cardiovascular disease, and alcohol can interfere with anticoagulant medications.
What are the risks associated with anticoagulants?
Unfortunately, because anticoagulants work by preventing blood clots, they also can lead to side effects or contraindications:
- Injury: Anticoagulants are not recommended, if a patient has had a bleeding event or chronic conditions like ulcers where bleeding could be difficult to control.
- Menstruation or Pregnancy: Anticoagulants can lead to heavier periods and so care must be taken when they are prescribed during a woman’s “childbearing years” – the time in life when SLE is the most likely to occur. Warfarin, in particular, has been associated with birth defects.
- Surgeries: Patients who are planning to have surgery are often advise to stop taking anticoagulants, especially Warfarin, at a point before a surgical procedure and perhaps switch to other medications to avoid bleeding problems.
Note: Again, this article is for informational purposes only. As always, consult your healthcare provider before making any changes to your treatment plans!
.

In Conclusion
Thrombosis – blood clots – are a significant health risk for those living with lupus – this is particularly important for those with lupus nephritis. Thankfully, anticoagulants are powerful medications and can successfully reduce these risks. Anticoagulants can also offer peace of mind by alleviating the anxiety that the risk of life-threatening blood clots can cause. Just remember that they are best when patients also get regular blood work done, stick to their treatment plans, live as healthy of a lifestyle as possible, including appropriate exercise and a good diet, and do whatever it takes to reduce the inflammation and flares that can lead to organ damage.
As our understanding of lupus and the blood improve, anticoagulants will become even more effective within prescribed treatment options.
To learn more about blood and other blood conditions that affect those living with lupus, check out the KFL article, “Lupus and Blood Disorders.”
.
References
Al-Homood, I. A. (2012). Thrombosis in systemic lupus erythematosus: a review article. ISRN Rheumatology, Article 428269. https://doi.org/10.5402/2012/428269
Anticoagulants (2023, September 20). Johns Hopkins Lupus Center. https://www.hopkinslupus.org/lupus-treatment/common-medications-conditions/anticoagulants/
Health Union Medical Review Board. (2022, September 30). Abnormal blood clotting with lupus. Lupus.net. https://lupus.net/symptoms/blood-clotting
Cleveland Clinic (2023, September 27). Anticoagulants. https://my.clevelandclinic.org/health/treatments/22288-anticoagulants
Julia, S., & James, U. (2017). Direct oral anticoagulants: A quick guide. European Cardiology, 12(1), 40-45. https://doi.org/10.15420/ecr.2017:11:2
Rasool Z.S., & Tiwari V. (2023, July 17). Biochemistry, lupus anticoagulant. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK544357/
Vitamin K. (2023, March). Harvard, T.H. Chan School of Public Health. https://www.hsph.harvard.edu/nutritionsource/vitamin-k/
Yuan, W., & Guan, F. (2022). Thrombosis and anticoagulation therapy in systemic lupus erythematosus. Autoimmune Diseases, Article 3208037. https://doi.org/10.1155/2022/3208037
.
Author: Greg Dardis, MS
Professor Dardis was formerly the Chair of the Science Department at Marylhurst University and is currently an Assistant Professor at Portland State University. His focus has been human biology and physiology with an interest in autoimmunity. Professor Dardis is also a former President of the Board of Directors of Kaleidoscope Fighting Lupus.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

