Lupus and Celiac Disease
Having lupus increases the risk of developing other autoimmune diseases, like celiac disease – by 30% or more. Read on to find out more celiac disease, gluten and what they could mean for those with lupus.
- Introduction to Lupus and Celiac disease
- What if I have lupus and think I have celiac disease?
- More about Gluten and Celiac Disease
- In Conclusion
.
.
Introduction to Lupus and Celiac disease
Celiac disease is an autoimmune condition, affecting over 70 million people worldwide. Diagnosed cases have increased almost 5-fold over the last 50 years. This has brought an increase in awareness of the condition, better disease management, and gluten-free food options on a global scale. As research on celiac disease, as an autoimmune disease, has increased, connections to other conditions, like lupus, have been found.
It is easy to confuse celiac disease with gluten-intolerance or a gluten allergy, but they are not the same.
Celiac disease is a true autoimmune disorder that causes an immune reaction in the small intestine after eating gluten.
Gluten-intolerance, on the other hand, is a digestive issue caused by a lack of the enzymes that digest gluten. Similar to lactose intolerance, it can cause pain and bloating, but it has nothing to do with immunity and is rarely a serious condition.
A gluten allergy is an immune response, like a peanut allergy, but not an autoimmune condition. It can cause reactions similar to intolerance, but can be more severe and even life-threatening.
Celiac disease symptoms can mimic those of lupus, so it helps to understand more about the condition and how the body may respond to gluten – or the absence of it – if diagnosed. Celiac disease can even be asymptomatic, making it difficult to get to the root of why someone may suddenly feel so poorly. While having to give up gluten can seem overwhelming at first, it can also be a great opportunity to learn about new food options and create a diverse, healthy, and tasty menu that supports lupus management!
.

.
What if I have lupus and think I have celiac disease?
Because the symptoms of both celiac disease and lupus can be pretty similar, it can be hard to tell if gluten is the issue. It also makes it difficult for healthcare practitioners. Both diseases result from autoimmunity and share some of the same antibodies – specifically human leukocyte antigens (HLAs). The rash from celiac disease also looks very similar to cutaneous lupus. Since the medications sometimes used to treat lupus may also affect celiac disease, they can even hide celiac disease symptoms from patients and practitioners.
Alternatively, if flares or lupus symptoms seem to not improve, it may be a good idea to get tested for celiac disease. It may also be a good idea to add a gastroenterologist, dietician, hematologist, pathologist, or dermatologist to the healthcare team.
Various types of gluten-free flour – chickpeas, rice, buckwheat, quinoa, almond, corn and oatmeal
.
More about Gluten, Celiac Disease and How They Relate to Lupus.
Gluten is a protein found in wheat, and other grains. It acts like glue and provides elasticity to dough when cooking or baking. It is what holds a cake together and makes pizza dough stretch without breaking.
Gluten can be found most commonly in the following:
- the flour in sweets, breads, and pasta;
- cereals;
- barley and rye products;
- some starches; and
- semolina, spelt, triticale, faro, and kamut.
Importantly, gluten can be sneaky and is found in processed foods like sauces, soups, candy bars, French fries, and even beer. Gluten can also lurk in products like shampoos, lotions, and even tampons.
Some starches contain gluten and may be used as binding agents in medications and supplements. In the U.S., for instance, drug manufacturers are not required to label their products for the consumer. It may take a stealthy pharmacist to find where gluten is hidden in products.
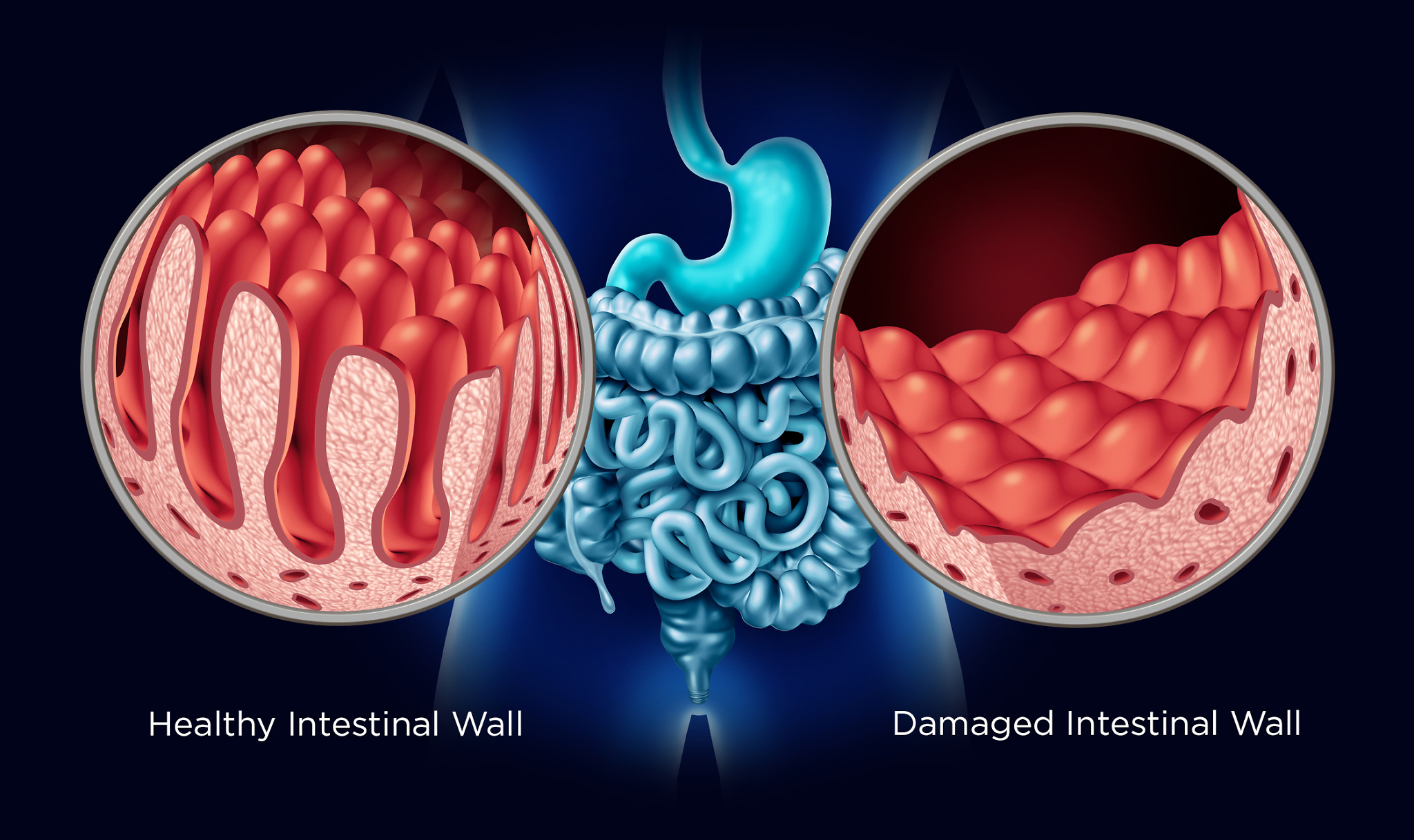
Celiac disease is an autoimmune reaction to gluten that occurs in the small intestine. It creates autoantibodies in the small intestine causing inflammation when gluten is consumed. This inflammation can prevent the small intestines from absorbing nutrients. It also may cause something called a “leaky gut.” A leaky gut means that antigens (food and bacteria) can ”leak” through the intestinal wall and to the blood steam. This can initiate inflammation and an immune response.
The gut microbiome may also play a significant role in the risk for celiac disease. Scientists have found that those with celiac disease, have too few good bacteria, like Bifidobacteria.
.
.
Symptoms of celiac disease can resemble some of the symptoms of lupus, including:
- diarrhea, nausea, and vomiting;
- fatigue, headaches, and brain fog;
- constipation, bloating, and gas;
- rash; and
- joint and abdominal pain.
Testing for celiac disease requires blood tests that look for autoantibodies, genetic tests that looks for antigens specific to celiac, and endoscopies that allow gastroenterologists to look for damage in the small intestines and take biopsies, if necessary.
Celiac disease is not curable, but can be treated using the steroids and immunosuppressives that are often used for lupus. It is also treated by strictly following a gluten-free diet. However, for about 30% of those with the condition, celiac disease is not responsive to treatment – possibly due to underlying, undiagnosed issues, such as lactose intolerance. If celiac disease is not strictly managed or treated at all, it may develop into refractory celiac disease, which can cause permanent damage to the small intestine. That is why it is so important to diagnose celiac disease and to follow treatment guidelines as strictly as possible.
.
In Conclusion
Celiac disease is manageable. I may require some adjustments to the steroids and immunosuppressives that are taken for lupus. It also requires adopting a gluten-free diet. This can be intimidating and scary, but it does not have to be. Because the disease is so prevalent, it has received greater awareness not only from the medical community but the food manufacturing community as well. There are many great gluten-free choices that can make eating pleasurable!
References
Celiac disease. (21, October 2020). The Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/celiac-disease/symptoms-causes/syc-20352220
Celiac disease, non-celiac gluten sensitivity, and food allergy: How are they different? (2021). American Academy of Allergy Asthma & Immunology. https://www.aaaai.org/conditions-and-treatments/library/allergy-library/celiac-disease
Dahan, S., Shor, D., Comaneshter, D., Tekes-Manova, D., Shovman, O., Amital, H., & Cohen, A. (2016). All disease begins in the gut: Celiac disease co-existence with SLE. Autoimmunity Reviews, 15, 848-853.http://dx.doi.org/10.1016/j.autrev.2016.06.003
Kumral, D. & Syed, S. (2020). Celiac disease screening for high-risk groups: Are we doing it right? Digestive Diseases and Sciences, 65, 2187-2195. https://doi.org/10.1007/s10620-020-06352-w
Ludvigsson, J., Rubio-Tapia, A., Chowdhary, V., Murray, J., & Simard, J. (2012). Increased risk of systemic lupus erythematosus in 29,000 patients with biopsy-verified celiac disease. The Journal of Rheumatology, 39(10), 1964-1970. doi: 10.3899/jrheum.120493
Punder, K. and Pruimboom, L. (2013). The dietary intake of wheat and other cereal grains and their role in inflammation. Nutrients, 5(3), 771-787. https://doi.org/10.3390/nu5030771
What is celiac disease? (n.d.). Celiac disease Foundation. https://celiac.org/about-celiac-disease/what-is-celiac-disease/
Author: Liz Heintz
Liz Heintz is a technical and creative writer who received her BA in Communications, Advocacy, and Relational Communications from Marylhurst University in Lake Oswego, Oregon. She most recently worked for several years in the healthcare industry. A native of San Francisco, California, Liz now calls the beautiful Pacific Northwest home.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.



