Lupus, Cystitis and Urinary Tract Infections
More than one in three of all those with lupus experience urinary tract infections (UTIs) – far more than the general public. They are among the most common reasons for lupus hospitalization and if not treated early, can lead to serious damage. Read on find out about the causes, symptoms and treatments for UTIs and cystitis related to lupus – it just might save you from a great deal of pain.
- Introduction to Lupus, Cystitis, and Urinary Tract Infections (UTIs)
- A Brief Tour of the Urinary Tract System
- Cystitis and UTI Causes, Diagnoses and Treatments
- How to Prevent Urinary Tract Inflammation and Infections
- In Conclusion
Introduction to Lupus, Cystitis, and Urinary Tract Infections
Approximately 36% of those with lupus experience urinary tract infections (UTIs), significantly more than the general population. They can occur anywhere along the urinary tract, including the kidneys, ureters, urinary bladder and urethra. In general, UTIs are caused by bacterial infection, most commonly Escherichia coli (E. coli), which can result in inflammation, frequent peeing and sometimes pain. UTIs account for about a third of the infections for those with SLE.
The urinary tract diseases that are most associated with systemic lupus erythematosus (SLE) usually involve the kidneys themselves, in the form of lupus nephritis, or in the lower urinary tract from the bladder to the urethra. When the inflammation is limited to the bladder, it is called cystitis, and there are two types, interstitial cystitis and lupus cystitis, that have autoimmune origins and can develop without an actual infection.
Untreated, chronic bladder inflammation not only damages the bladder, but can affect the rest of the renal system. If the ureters become blocked or inflamed, urine may back up into the kidneys can cause kidney damage and further infection. Those with SLE already have a greater risk for developing renal disease. So, anything that could further affect the kidneys should be taken seriously.
.

.
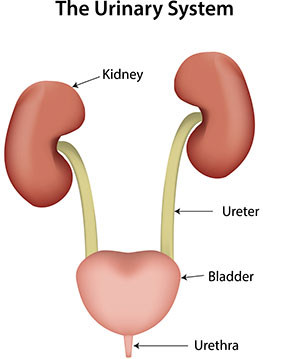
A Brief Tour of the Urinary Tract System
The primary function of the urinary tract system is to filter blood and eliminate waste called urea. Urea enters the kidneys, where it is collected with water and other waste products and is turned into urine. Urine then passes from the kidneys through two tubes called ureters, emptying into the bladder. The bladder is a little triangular sac that sits at the base of the lower abdomen, holding the urine until a nerve signal from the pelvis tells the brain it is time to urinate. Once it is time, the urine leaves the bladder end enters into the urethra, where it comes out of the body and is flushed away.
Cystitis and UTI Causes, Risk Factors, Diagnoses and Treatments
Cystitis, inflammation of the bladder, is usually caused by a bacterial infection. However, cystitis can also occur due to autoimmune reactions, the effects of some lupus medications, the use of fragrant, feminine hygiene sprays and soaps, spermicidal jellies used during intercourse, or other underlying health conditions. Cystitis may go away once those products or medications are eliminated, or the underlying health condition is treated.
There are two kinds of cystitis most associated with lupus:
Interstitial cystitis is chronic cystitis without infection. Women with lupus are at greater risk for interstitial cystitis, and the risk increases with age. Interstitial cystitis causes inflammation and irritation of the bladder’s lining, resulting in increased bladder pressure and lower abdominal pain. Nerves in the pelvis falsely send messages to the brain saying the bladder is full when it is not, creating the feeling of constantly needing to urinate. Interstitial cystitis is also known as painful bladder syndrome because it is!
It is unclear what causes interstitial cystitis, though experts suspect it may be due to bladder or pelvic floor damage. It may also be due to an autoimmune response or allergic reaction.
Diagnosis: Interstitial cystitis can be difficult to diagnose and may require a cystoscopy (examination of the bladder under anesthesia).
Treatment: It can often be treated with physical therapy, nerve stimulation, over-the-counter pain relievers, antihistamines, or even antidepressants. Immunosuppressive therapy is a treatment option if all else fails.
Lupus cystitis is similar to interstitial cystitis, but is fairly rare – affecting only about 2% of the lupus population. It can fluctuate with lupus disease activity and flares, waxing and waning through time, whereas interstitial cystitis symptoms are more consistent.
Symptoms of lupus cystitis more often include lower abdominal upset than bladder or urinary discomfort.
Diagnosis: As with interstitial cystitis, diagnosis can be difficult. It is rare and requires the additional diagnosis of lupus itself. For some, a lupus cystitis diagnosis is the fiRst indication that they have lupus.
Treatment: Since lupus cystitis is an autoimmune condition, it is initially treated with anti-inflammatory steroids and immunosuppressives.
.
Urinary tract infections (UTIs) are caused by a bacteria, usually Escherichia coli (E. coli) that normally live in our digestive tracts.
The symptoms for all of these conditions are similar and include:
- discomfort while urinating (dysuria);
- frequently waking at night to urinate (nocturia);
- cloudy or bloody urine;
- more often and urgently needing to urinate;
- lower abdominal discomfort, including pain, nausea, vomiting, diarrhea, and constipation; and
- fever, chills, and joint pain.
Diagnosis: A urinalysis will initially look for signs of infection. Additional blood tests, imaging, or even a biopsy may be needed for diagnosis, depending on the results.
Treatment: While a UTI will go away quickly for some by drinking fluids and resting, you will need medical attention if you have lupus. To dispel the myth, drinking cranberry juice or taking cranberry supplements may help prevent a UTI but not cure it – there is just no solid evidence. Antibiotics will be necessary!
For those living with lupus, these the most important risk factor for UTIs and cystitis:
- Being female: Women account for over 90% of those diagnosed with lupus; urinary tract infections are the most common form of bacterial infection in women, and women are 5 times more likely to get urinary tract infections than men. Why? Women have shorter urethras than men, so anatomically bacteria have a far shorter distance to get to the bladder in women than men.
- Vasculitis of the gastrointestinal tract: Cystitis is more likely to occur if a person also has lupus mesenteric vasculitis;
- Positive antinuclear antibody and complement C3 and C4 protein tests are associated with a great risk for cystitis;
- Frequency of sexual intercourse;
- Leucopenia – a low white cell blood count: With fewer white blood cells, the body is less able to fight urinary tract infections;
- Immunosuppressant therapy: These drugs are commonly prescribed to those with lupus, and since they decreases the body’s ability to fight infection they may make UTIs more likely, and
- Central Nervous System SLE: Up to 21% of those with lupus have autonomic nervous system dysfunction, and this can affect the nerves responsible for urinary function.
.

How to Prevent Urinary Tract Inflammation and Infections
While inflammation may not be entirely preventable, if you have lupus, several things can be done to limit the risk of urinary tract infections:
- Drink plenty of fluids, especially water, by aiming for eight glasses a day, unless otherwise recommended by a practitioner.
- Limit alcohol and caffeine as these stimulants can be very dehydrating.
- Eat plenty of fiber to prevent constipation.
- Wear breathable cotton underwear and loose-fitting clothes to maintain airflow and prevent moisture-breeding bacteria.
- Practice urinary hygiene by going when you need to go and finish urinating completely. Wipe the area gently and thoroughly after urinating. Urinate after sex to get rid of bacteria.
As mentioned earlier, always seek advice from a healthcare practitioner immediately if you suspect a UTI, especially if you have lupus!
In Conclusion
Infections are some of the most damaging consequences of having lupus, and UTIs are one of the most common and serious types associated with lupus. An uncomfortable feeling lower in the abdomen and frequent peeing may indicate a problem in the urinary tract – either from infection or inflammation. If you notice any of the symptoms described in this article, take precautions and seek medical advice immediately.
References
13 tips to keep your bladder healthy. (17, May 2017). National Institute on Aging. https://www.nia.nih.gov/health/13-tips-keep-your-bladder-healthy
Cystitis. (20210. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/cystitis/diagnosis-treatment/drc-20371311
Duran-Barragan, S., Naranjo, H., Rodriguez-Gutierrez, L., Solano-Moreno, h., Hernandez-Rios, G., Sanchez-Ortiz, A., & Ramos-Remus, C. (2008). Recurrent urinary tract infections and bladder dysfunction in systemic lupus erythematosus. Lupus, 17, 1117-1121.
Hidalgo-Tenorio, C., Jimenez-Alonso, J., de Dios Luna, J., Tallada, M., Martinez-Brocal, A., & Sabio, J. (2004). Urinary tract infections and lupus erythematosus. Annals of Rheumatic Disease, 63, 431-437.
Interstitial cystitis. (2021). Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/interstitial-cystitis/symptoms-causes/syc-20354357
Koh, J., Lee, J., Jung, S., Ju, J., Park, S., Kim, H., & Kwok, S. (2015). Lupus cystitis in Korean patients with systemic lupus erythematosus: Risk factors and clinical outcomes. Lupus, 24, 1300-1307.
Liberski, S., Marczak, D., Mazur, E., Mietkiewicz, K., Leis, K., & Gatazka, P. (2018). Systemic lupus erythematosus of the urinary tract: Focus on lupus cystitis. Reumatologia, 56(4), 255-258.
Urinary tract infection. (2021). Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/urinary-tract-infection/symptoms-causes/syc-20353447
Wen, J., Lo, T., Chuang, Y., Ho, C., Long, C., Law, K., Tong, Y., & Wu, M. (2019). Risks of interstitial cystitis among patients with systemic lupus erythematosus: a population-based cohort study. International Journal of Urology, 26, 897-902.
Author: Liz Heintz
Liz Heintz is a technical and creative writer who received her BA in Communications, Advocacy, and Relational Communications from Marylhurst University in Lake Oswego, Oregon. She most recently worked for several years in the healthcare industry. A native of San Francisco, California, Liz now calls the beautiful Pacific Northwest home.
All images, unless otherwise noted, are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

