Lupus and the Lymphatic System
The human body has over 600 lymph nodes, and during a lupus flare, every single one of those 600 lymph nodes can react and become swollen. And if that isn’t enough, lymph nodes are only one part of a vast network of tissues and pathways that make up the lymphatic system – a key player in both immunity and autoimmunity. Read on to learn more about what the lymphatic system means for those living with lupus.
- Introduction
- What You Should Know About Your Lymphatic System
- Lupus and Lymph
- What This Means for You
- Taking Care of Yourself
- In Conclusion
The lymphatic system has a central role in the body’s immune response. It is part of the first line of defense of health and wellbeing, when the body comes in contact with something harmful – a virus, bacteria, infection or injury. The lymphatic system stands ready to take on any unwanted intruder that comes its way, but if lupus is thrown in the mix, it may be harder for it to effectively do its job.
What You Should Know About Your Lymphatic System:
If your cardiovascular system is a super highway of blood vessels, your lymphatic system is a network of back roads and alleyways. Here is why – your cardiovascular system moves blood, oxygen, nutrients and wastes quickly around the body with each beat of your heart. Whereas, your lymphatic system slowly guides the interstitial fluid, called lymph, to flow between the cells of the body. Why is it so slow? The slow moving lymph allows immune cells to travel places were blood does not go and take any infecting microbe to be filtered out by lymph nodes. The cells that do this work are white blood cells, called lymphocytes (B cells and T cells), and they not only fight infections, but can also be the source of an autoimmune response.
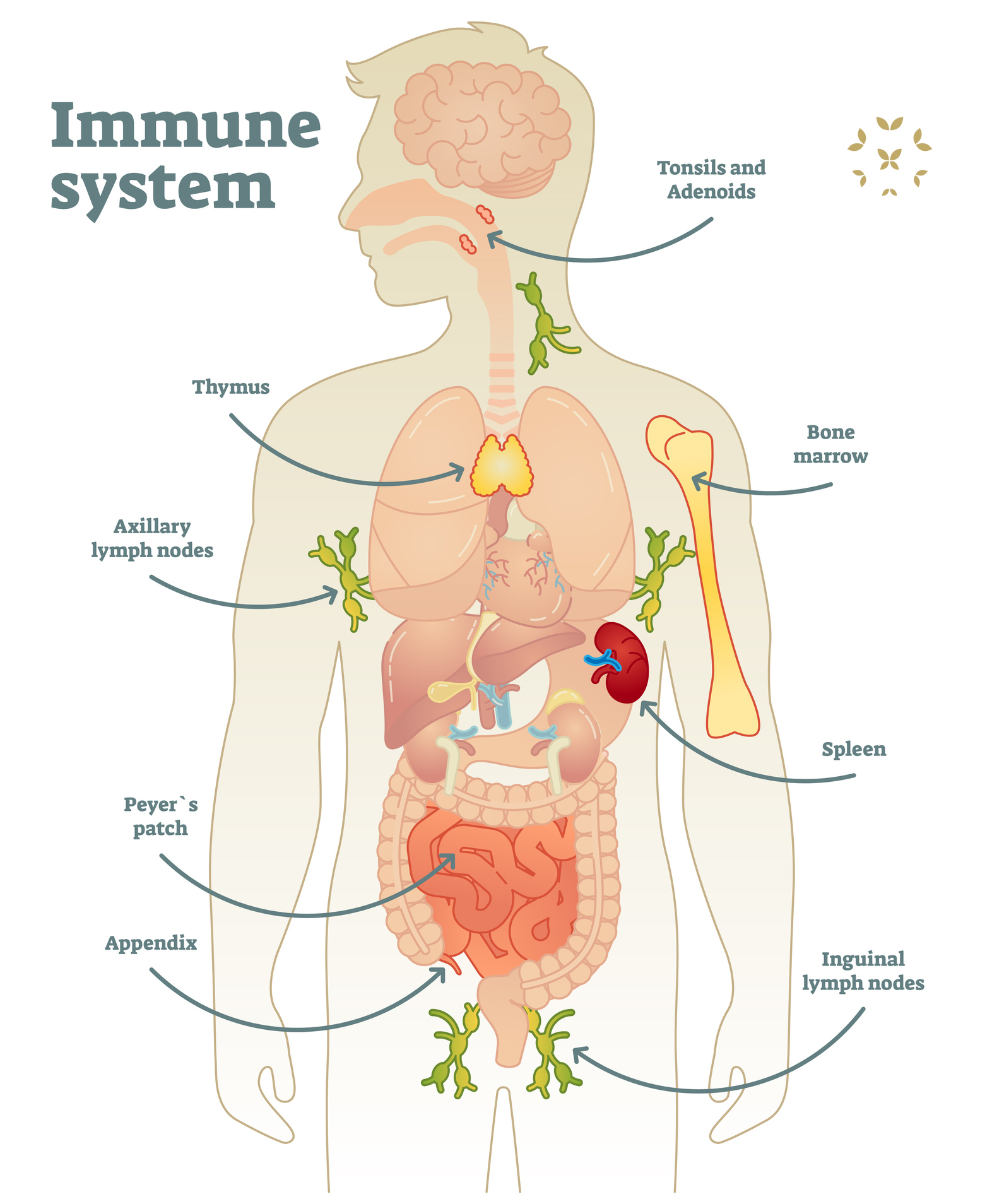
Some parts of the lymphatic system include:
- Lymph Nodes: What many of us call “glands,” hundreds of lymph nodes throughout our body filter all of the fluid collected throughout the lymphatic system. These nodes also hold immune cells that produce antibodies – both the good kind and the bad kind. As these cells increase in number, they can swell the lymph nodes to the point that they make us feel both pressure and pain.
- Bone Marrow: The marrow of the larger bones in the body, such as the ribs, vertebrae, pelvis, humerus (upper arm) and femur (thigh) produce the lymphocytes (including T cells and B cells) that are needed to fight illness and produce the inflammatory response.
- Thymus: Located under the sternum, the thymus is where T cells become ready for their many roles in the immune response.
- Spleen: Located above the stomach on the left side of the body, the spleen filters blood and also produces white blood cells, such as lymphocytes. Up to 45% of those with lupus may develop an enlarged spleen.
- Tonsils: Our tonsils are specialized lymph nodes that filter harmful microbes that enter through our nose and mouth.
- Peyer’s Patches: These lymphatic nodules are spread throughout the lower small intestine and monitor the bacteria in the gut for pathogens.
- Appendix: The appendix is not as useless as many believe. Recent studies show that it contains lymphatic tissue. It acts like a “safe house” for good gut bacteria and produces antibodies to limit the growth of bad intestinal bacteria.
The relationship between the lymphatic system and lupus is not entirely understood. However, with lupus, as with other autoimmune diseases, such as rheumatoid arthritis (RA) and scleroderma, lymphatic vessels may expand and contract more readily than normal as they try to get rid of inflammatory cells. The lymph nodes also swell as they accumulate and filter lymph, causing a buildup of inflammatory cells and fluid. As fluid accumulates, this can lead to increased joint swelling and pain. This is the most common symptom for those with lupus.
While the nodes are not necessarily swollen all of the time, they can swell when disease activity is high or during a lupus flare. In some cases, lymph has been found to leak outside of the lymphatic system into the abdomen and upper spine in those with lupus. This may be due to lymphatic blockage or other lymphatic flow defects. This is an area that needs more research.
It has been shown that patients with scleroderma may have fewer lymphatic vessels in their skin, which may ultimately lead to lymph blockage as the existing vessels cannot accommodate the increased volume of fluid. This buildup can ultimately cause ulcers and sores.

Since swollen lymph nodes may indicate high disease activity or a lupus flare, it is really important to pay close attention to your symptoms. If your nodes become tender and swollen, or the body seems to be retaining fluid, or if you have a fever, it is wise to reach out to a healthcare provider right away to seek advice to find out if it is because of a flare or if there is something else going on such as an infection or other condition.
The most common lymphatic system disorders that those with lupus should know about include:
- Lymphadenopathy: Common to those with lupus, lymphadenopathy (swollen lymph nodes) is most often caused by inflammation and is worse during a flare or high disease activity. Lymphadenopathy may be one of the first symptoms of SLE for some, especially children – the glands will typically swell in the neck, armpits, and groin. Lymph nodes can also swell due to infection and even cancer.
- Kikuchi’s syndrome: When lymph nodes swell ≥ 1.5 inches in diameter, Kikuchi’s syndrome may be to blame. Though relatively harmless, Kikuchi’s can also cause mild fever and night sweats.
- Lymphedema: Lymphedema occurs when the body retains too much lymphatic fluid, usually as a result of surgery or radiation for cancer. The lymph nodes and vessels may become damaged and scar tissue may grow, blocking fluid from moving. This disorder is rare in lupus, however, and usually turns out to be lymphadenopathy.
- Lymphoma: Hodgkin’s lymphoma and non-Hodgkin’s lymphoma are cancers of the lymph nodes, which can stop lymph from flowing normally due to tumors that may develop which block the collective ducts or nodes. There is a 3 times greater risk for lymphoma in those with lupus, possibly due to the overstimulation of B-cells and problems with how the immune system scouts for harmful substances. Those with Sjogren’s syndrome may have a 44 times increased risk of developing non-Hodgkin’s lymphoma.
Lupus medications such as azathioprine (Imuran) and mycophenolate mofetil (CellCept) may increase the risk of lymphoma, as well as the overstimulation of B-cells. Cyclophosphamide may increase the risk of lymphoma, as well.
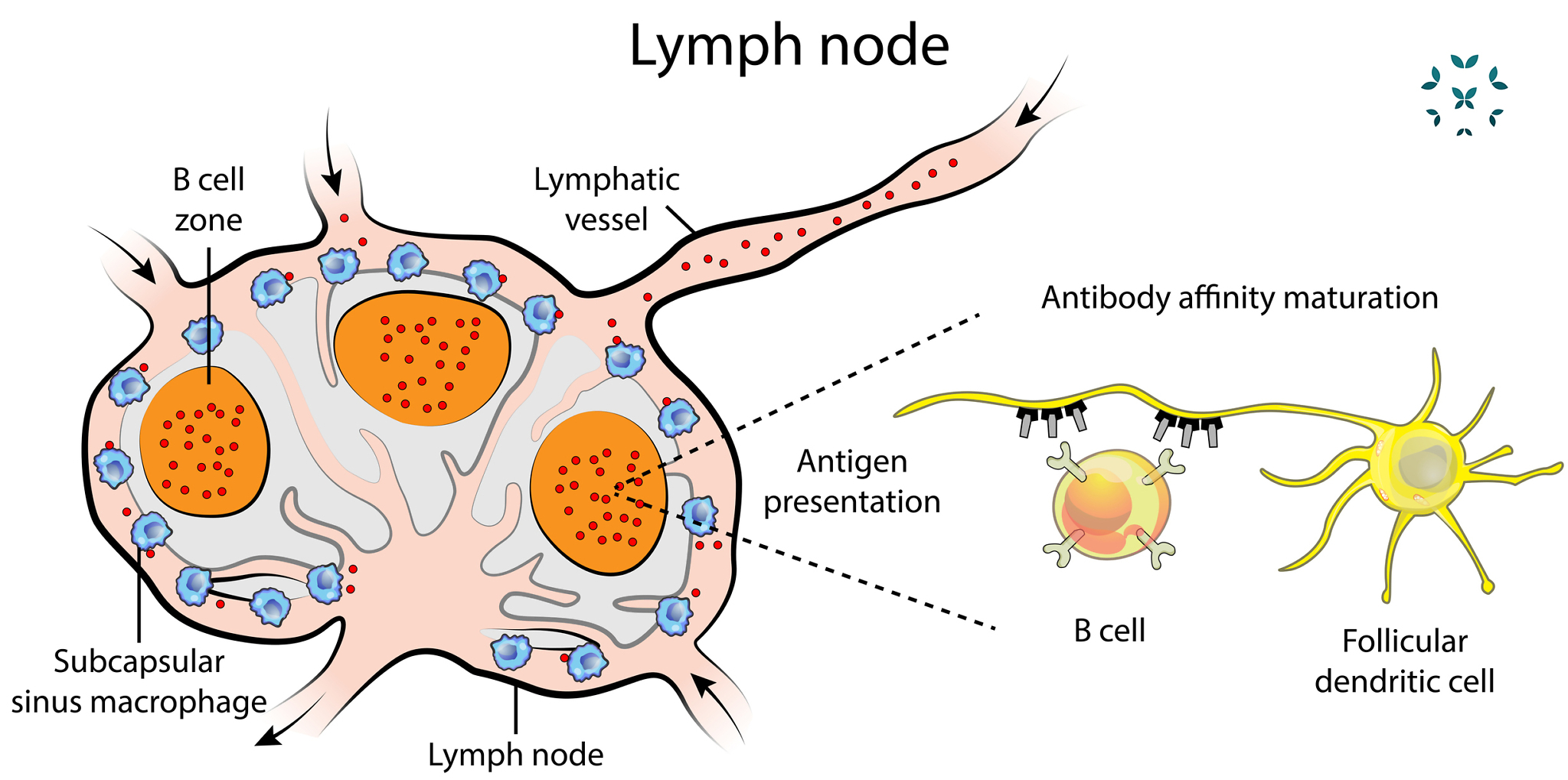
Since lymph nodes may swell from time to time, it is good to know about some things that can be done at home to ease discomfort until you can see your healthcare team. Warm, wet compresses can be applied to the tender areas to help relieve pain. NSAIDs may also help to alleviate soreness, but it is always wise to check in with a healthcare practitioner first to make sure they can be taken safely. A healthcare practitioner may also prescribe other anti-inflammatory drugs to bring down swelling.
Developing healthy habits may not only help with lupus symptoms but may help with lymphatic and immune health as well. These habits include:
- Maintaining a healthy weight and diet by choosing the right foods and exercising to keep the body moving.
- Drinking plenty of water to keep hydrated for lymph to move easily throughout the body.
- Avoiding harmful chemicals and known toxins found in household products, cleaning products, etc., to keep them from getting into the body which can make it harder for the body to move and filter waste.
- Rest! If your body is telling you to slow down or even stop, listen to it. Sometimes rest and sleep can be the best medicines.
Like many other systems of the body, the lymphatic system is complex … and a lupus diagnosis only adds to that complexity. Knowing a little bit more about the lymphatic system can be an important addition to your healthcare toolkit. While this information may be confusing at first, you may be able to eventually see how the pieces fit together and gain a greater appreciation for all the functions your body is responsible for maintaining and why there is such a delicate balance to maintain between feeling relatively fit and feeling unwell.
References
Afzal, W., Arab, T., Ullah, T., Teller, K., & Doshi, K. (2016). Generalized lymphadenopathy as presenting feature of systemic lupus erythematosus: Case report and review of the literature. Journal of Clinical Medicine Research, 8(11), 819-823. doi: 10.14740/mocmr2717w.
Brown, J. & Skarin, A. (2004). Clinical mimics of lymphoma. The Oncologist, 9(4), 406-416. doi: 10.1634/theoncologist.9-4-406. https://theoncologist.onlinelibrary.wiley.com/doi/full/10.1634/theoncologist.9-4-406
Lupus and cancer. (2020). Johns Hopkins Lupus Center.
https://www.hopkinslupus.org/lupus-info/lifestyle-additional-information/lupus-cancer/
Lymphatic system. (23, February 2020). Cleveland Clinic. https://my.clevelandclinic.org/health/articles/21199-lymphatic-system
Mader, S. & Windelspecht, M. (2018). Human biology (15th ed.). McGraw Hill Education.
Randolph, G., Ivanov, S., Zinselmeyer, B., & Scallan, J. (2017). The lymphatic system: Integral roles in immunity. Annual Review of Immunology, 35, 31-52. doi: 10.1146/annurev-immunol-041015-055354. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5551392/
Scallan, J., Zaweija, S., Castorena-Gonzales, J., & Davis, M. (2016). Lymphatic pumping: Mechanics, mechanisms and malfunction. The Journal of Physiology, 594(20), 5749-5768. Doi: 10.1113/JP272088. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5063934/
Schwartz, N., Chalasani, M., Li, T., Feng, Z., Shipman, W., & Lu, T. ( 2019). Lymphatic function in autoimmune diseases. Frontiers in Immunology, 10, Article 519. Doi: 10.3389/fimmu.2019.00519. https://www.frontiersin.org/articles/10.3389/fimmu.2019.00519/full
Thomas, D. (2014). The lupus encyclopedia. Johns Hopkins Press.
Wallace, D. (2019). The lupus book (6th ed.). Oxford University Press.
Author: Liz Heintz
Liz Heintz is a technical and creative writer who received her BA in Communications, Advocacy, and Relational Communications from Marylhurst University in Lake Oswego, Oregon. She most recently worked for several years in the healthcare industry. A native of San Francisco, California, Liz now calls the beautiful Pacific Northwest home.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.

