Lupus Overlap Diseases and Overlap Syndrome
As an individual with lupus, you may find yourself managing additional autoimmune and connective tissue diseases. This article provides a brief overview of these conditions collectively known as lupus overlap diseases and overlap syndrome.
- Introduction
- Rheumatoid Arthritis
- Sjögren’s Syndrome
- Raynaud’s Phenomenon
- Scleroderma
- Mixed Connective Tissue Disease
- Overlap Syndrome
- In Conclusion
Introduction
Several autoimmune, rheumatic and connective tissue diseases that manifest and behave in ways akin to lupus are considered lupus overlap diseases. However, there is lack of agreement within the medical and lupus communities on just one, definitive and inclusive list of these conditions. For this article, Kaleidoscope Fighting Lupus decided to focus on the most commonly reported conditions, which include:
- Rheumatoid arthritis (RA)
- Sjögren’s syndrome
- Raynaud’s phenomenon
- Scleroderma
- Mixed Connective Tissue Disease (MCTD)
It is important to note that there is a lack of general consensus as to whether or not mixed connective tissue disease (MCTD) is truly an overlap of lupus. It is even often hard to determine which of these two are manifested in an individual first. We recognize this and have decided to include MCTD in the list above in order to be inclusive of those who suffer from this condition along with SLE.
In a 2015 Lupus Science & Medicine article, Michael D. Lockshin and others found that up to 38% of individuals with SLE may have an overlap disease. The study also found that individuals with an overlap disease experience more “disease-associated damage” and are older than individuals who are diagnosed with SLE only. Just like with many other health conditions including lupus, the degree to which an individual experiences any overlap diseases can wax and wane over time and may even go into remission.
Individuals may also develop overlap syndrome, which is a bit different from having an overlap disease. In overlap syndrome, an individual has two or more connective tissue diseases that usually occur at the same time. For example, an individual who has lupus and Sjögren’s (another connective tissue disorder) has overlap syndrome, but if another individual has lupus and Raynaud’s and no other conditions, they have overlap disease. This differs from MCTD where the multiple conditions typically occur in a sequence and not at the same time. Scientists have also found that in some cases of overlap syndrome, there is a distinct antibody profile that can help healthcare practitioners with a diagnosis of that condition specifically. Finding diagnostic antibodies or other biomarkers for each condition is an important and ongoing effort in the research community.
Yes, with lupus and overlap diseases, things can get very complicated! Unfortunately, it is not uncommon for someone with lupus to face one or more of these conditions. So, it is important to be as informed as possible in order to maintain an active role in the management of one’s own healthcare … and to be an empowered self-advocate! Take the time to learn about the different overlap conditions, including overlap syndrome itself, and pay close attention to changes in your symptoms and overall health. That way, you can effectively communicate with your healthcare practitioners.
Here is a brief overview of the most commonly reported overlap diseases.
Rheumatoid Arthritis (RA)
RA is an autoimmune and a connective tissue disease most-often characterized by joint swelling, stiffness and pain in the small joints of the hands and feet though it can affect the lungs, eyes or other organs. RA is often worse in the morning and tends to ease a bit throughout the day. About 1-3% of the population has RA, primarily women.
The earlier RA is diagnosed and treated, the better the outcome. It is typically treated by a rheumatologist through the use of antirheumatic medications, which include methotrexate, hydroxychloroquine (Plaquenil) and sulfasalazine. Each of these drugs can cause significant side effects, but each can also alleviate and even prevent joint damage. Low-impact exercise may also help manage symptoms and increase range of mobility as muscle strength increases.

Sjögren’s Syndrome
Sjögren’s syndrome is also an autoimmune disorder and a connective tissue disease that can affect the entire body. Symptoms often include dry eyes, dry mouth, joint pain and fatigue. Structures and systems such as the kidneys, gastrointestinal system, blood vessels and lungs, however, may be affected. Similar to lupus, the symptoms of Sjögren’s can change throughout life, and sometimes go into remission. Iaccarino and others note that Sjögren’s and SLE are closely related to each other and share many of the same features. In a 2010 study, researchers observed that approximately 14.5% of individuals with lupus have Sjögren’s as a secondary condition.
A rheumatologist may prescribe medications that target dry eyes and mouth such as cyclosporine ophthalmic emulsion (Restasis) for the eyes or pilocarpine hydrochloride (Salagen) for the mouth. Immunosuppressants may also be prescribed, and many over-the-counter medications may help alleviate pain and discomfort.
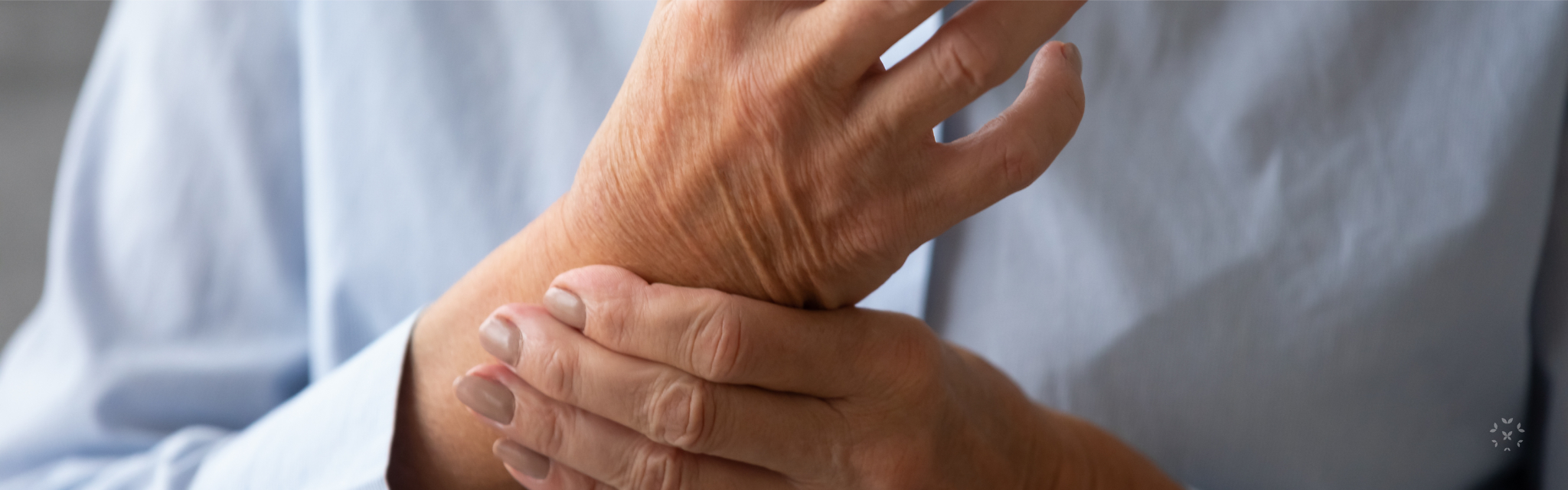
Raynaud’s Phenomenon
Raynaud’s phenomenon causes a restriction in the small blood vessels of the extremities, which in turn reduces blood flow. When the extremities are subjected to cold, the blood vessels go into spasms causing pain, numbness and skin discoloration. Raynaud’s primarily affects fingers, but can also affect the face, nose, ears and toes. Stress and emotional duress can often trigger a Raynaud’s attack. If untreated, skin ulcers may develop or in a worst-case scenario, gangrene.
If there is no underlying explanation for the symptoms, then the individual is considered to have primary Raynaud’s – because it cannot be attributed to anything else. If an individual has an autoimmune and/or other connective tissue disease, then the diagnosis is referred to as secondary Raynaud’s.
More than likely, a rheumatologist will diagnose Raynaud’s. There is no one drug to treat Raynaud’s although calcium channel blockers to dilate blood vessels or topical antibiotics to treat skin manifestations may be prescribed. Additionally, with primary Raynaud’s, relaxation therapies such as Tai chi and meditation may help to decrease stress or even a regular exercise regime that keeps the body active and stress at bay.
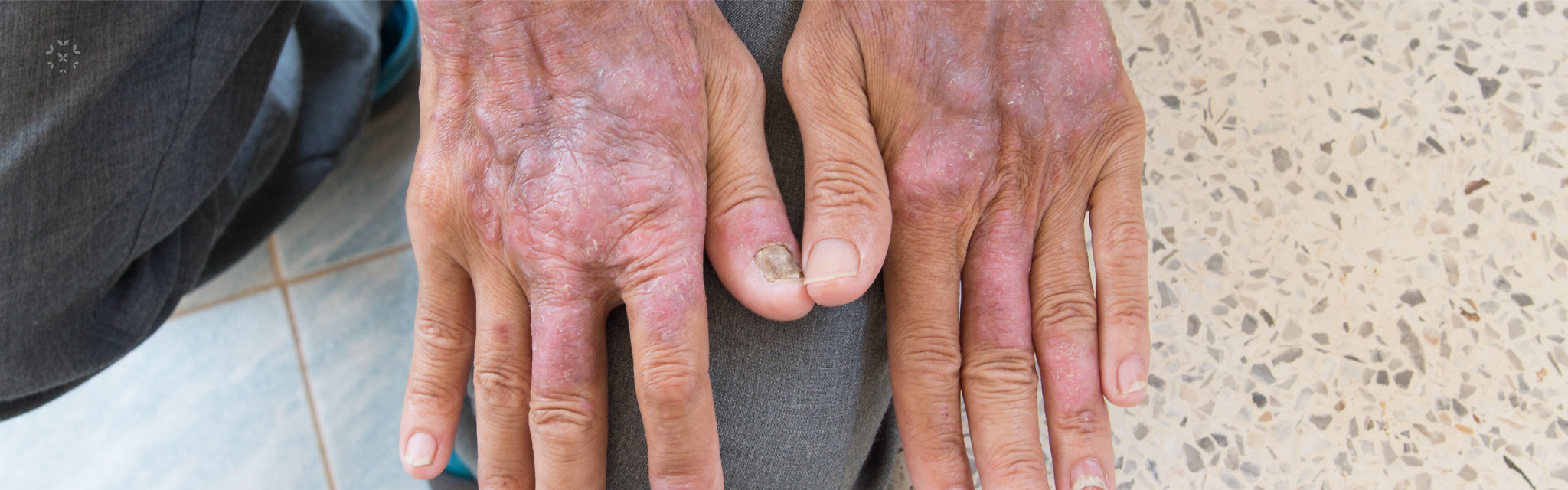
Scleroderma
Scleroderma is often preceded by Raynaud’s phenomenon. Symptoms of scleroderma include joint pain, swelling and stiffness in the fingers and hands that is often worse in the morning like RA. Scleroderma is considered a connective tissue and autoimmune rheumatic disease. If not treated, the skin can become tough and leathery due to a buildup of collagen, which can even spread to the face. Tissue loss and discoloration may occur. Organ and systemic involvement may occur in later stages of scleroderma including in the gastrointestinal tract, pulmonary and renal systems.
A rheumatologist and/or dermatologist can treat scleroderma. Treatment frequently includes immunosuppressants, anti-inflammatory medications, vasodilator therapy and/or anti-fibrotic medications that are used to reduce collagen production.
Mixed Connective Tissue Disease (MCTD)
MCTD has the symptoms of several connective tissue disease disorders such as lupus, scleroderma and polymyositis. An individual may not experience the symptoms of the multiple disorders concurrently, however, and instead they can occur in sequence over time. This makes MCTD difficult to diagnose. Symptoms can include muscle weakness, kidney disease, Raynaud’s phenomenon, heart and lung abnormalities, esophageal dysfunction, general malaise and skin rashes. Many who have MCTD also have symptoms of RA. Symptoms may progress into the organs if MCTD is not treated. MCTD affects more women than men and is most common in women younger than 30.
Several healthcare practitioners treat MCTD such as general practitioners, internists, neurologists, cardiologists, nephrologists, rheumatologists and dermatologists. Medications that can help manage MCTD symptoms are similar to those that treat lupus. These include corticosteroids, antimalarial drugs, calcium channel blockers, hypertension medications and immunosuppressants. There is no cure, but an individual’s symptoms may subside from time-to-time and during low-activity, they may not need drug intervention.
What is overlap syndrome?
An individual has overlap syndrome when they have at least two connective tissue diseases at the same time. These diseases include SLE, RA, Sjögren’s, systemic sclerosis (SSc), dermatomyositis and polymyositis. It is also possible for an individual to have both MCTD and overlap syndrome. Unfortunately, there has been less research on overlap syndrome itself than for each of the other individual connective tissue diseases. Researchers at the Jawaharlal Institute of Postgraduate Medical Education & Research acknowledge that there is a “need for dedicated clinal trials in patients of overlap syndrome for better understanding of the natural history, outcome and treatment strategy required for these syndromes.”
Luca Iaccarino and his research team note that an individual typically experiences milder symptoms of each individual condition when they have overlap syndrome. In the kind of overlap syndrome that involves both SLE and Sjögren’s for example, Iaccarino and others found that individuals experience less-intense symptoms of SLE and a “predominance of [Sjögren’s syndrome]-related features.”
Some cases of overlap syndrome are easier to diagnose than others because of the identification of specific antibodies. Anti-aminoacyl-t-RNA synthetase (Anti-ARS) is an antibody associated with dermatomyositis and polymyositis. The antibody Anti-PM-Scl is present when an individual has the overlap syndrome of systemic sclerosis and polymyositis. Rheumatoid factor (RF), as well as anti-Ro/SSA and anti-La/SSB can be found when an individual has SLE and Sjögren’s. In some cases like with RA and lupus, however, there is no specific antibody profile.
With regard to RA and lupus (“rhupus”), there is some debate as to whether or not this is an example of an overlap syndrome. This scenario is rare, occurring in approximately 2% of systemic rheumatic diseases. Iancarrino and others remark that while some researchers agree that having both lupus and RA is a true overlap syndrome, others disagree stating that it should be regarded as “an erosive subset of lupus arthropathy.” On the other hand, arthritis and arthralgia are extremely common manifestations of SLE occurring in up to 90% of individuals with lupus.
In Conclusion
Managing multiple illnesses in addition to lupus can seem overwhelming. Keeping track of all the symptoms an individual may experience, however, will help healthcare practitioners properly diagnose, treat and manage any additional conditions that may arise early on. Understanding when symptoms seem outside the norm of what an individual may typically experience can help in the early detection of overlap diseases, which in turn can help maintain optimal health.
References
Baer, A., Maynard, J., Shaikh, F., Magder, L., & Petri, M. (2010). Secondary Sjogren’s syndrome in systemic lupus erythematosus defines a distinct disease subset. The Journal of Rheumatology, 37(6), 1143-1149. doi: 10.3899/jrheum.090804. Retrieved March 3, 2020 from http://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.963.9944&rep=rep1&type=pdf
Frequently asked questions. (2020). Raynaud’s Association. Retrieved March 3, 2020 from https://www.raynauds.org/frequently-asked-questions/
Iaccarino, L., Gatto, M., Bettio, S., Caso, F., Rampudda, M., Zen, M., Ghiradello, A., Punzi, L., Doria, A. (2012). Overlap connective tissue disease syndromes. Autoimmunity Reviews, 12(2013), 363-373. doi: 10.1016/j.autrev.2012.06.004.
Lockshin, M., Levine, A., Erkan, D. (2015). Patients with overlap autoimmune disease differ from those with ‘pure’ disease. Lupus Science & Medicine, Article e000084. doi: 10.1136/lupus-2015-000084. Retrieved March 3, 2020 from https://lupus.bmj.com/content/2/1/e000084
Lupus signs, symptoms, and co-occurring conditions. (2020). Johns Hopkins Lupus Center. Retrieved March 3, 2020 from https://www.hopkinslupus.org/lupus-info/lupus-signs-symptoms-comorbidities/
Mixed connective tissue disease. (n.d.). Mayo Clinic. Retrieved March 3, 2020 from https://www.mayoclinic.org/diseases-conditions/mixed-connective-tissue-disease/symptoms-causes/syc-20375147
Mixed connective tissue disease. (2014). Genetic and rare diseases information center. Retrieved March 3, 2020 from https://rarediseases.info.nih.gov/diseases/7051/mixed-connective-tissue-disease
Rheumatoid arthritis. (2020). American College of Rheumatology. Retrieved March 3, 2020 from https://www.rheumatology.org/I-Am-A/Patient-Caregiver/Diseases-Conditions/Rheumatoid-Arthritis
Scleroderma symptoms. (n.d.). The Scleroderma Education Project. Retrieved March 3, 2020 from https://sclerodermainfo.org/faq/symptoms-and-prognosis/?gclid=CjwKCAiAy9jyBRA6EiwAeclQhIctG-T8-8Du8mHphtQen4tqupxB-SXO85wAIhkm1suPX_oDHwAH9xoCKjkQAvD_BwE
Shah, S., KG, C., & Negi, V. (2019). Systemic lupus erythematosus and overlap: A clinician perspective. Clinical Dermatology Review, 3(1), 12-17. doi: 10.4103/cdr.cdr_44_18. Retrieved March 3, 2020 from http://www.cdriadvlkn.org/article.asp?issn=2542-551X;year=2019;volume=3;issue=1;spage=12;epage=17;aulast=Shah
Understanding scleroderma. (2020). Johns Hopkins Scleroderma Center. Retrieved March 3, 2020 from https://www.hopkinsscleroderma.org/scleroderma/
What is Sjogren’s? (2019). Sjogren’s Syndrome Foundation. Retrieved March 3, 2020 from https://www.sjogrens.org/
Author: Liz Heintz
Liz Heintz is a technical and creative writer who received her BA in Communications, Advocacy, and Relational Communications from Marylhurst University in Lake Oswego, Oregon. She most recently worked for several years in the healthcare industry. A native of San Francisco, California, Liz now calls the beautiful Pacific Northwest home.
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.


