Myositis and Lupus
SLE can cause inflammation in all areas of the body. When it directly damages muscle tissue, we call it myositis, a serious condition that causes pain and weakness, sometimes rashes and affects a surprising number of those living with lupus. Read on to find out more about myositis – its causes, diagnosis and treatment.
Contents:
- What is myositis?
- What are the signs and symptoms?
- How is it diagnosed?
- How is it treated?
- What causes myositis?
- Who gets myositis?
- What is the prognosis for someone with myositis?
- What research is being done?
What is Myositis?
 To understand myositis, we need to understand the definition of a myopathy. A myopathy is defined as a muscular disease in which the muscle fibers do not function for any one of many reasons, resulting in muscular weakness. “Myopathy” simply means muscle disease (myo= “muscle” + pathos/pathy=”suffering”) as opposed to a condition describing diseases involving the nerves, called neuropathies. The inflammatory myopathies are a group of diseases that involve chronic muscle inflammation, accompanied by muscle weakness. Another word for chronic inflammation of muscle tissue is myositis.
To understand myositis, we need to understand the definition of a myopathy. A myopathy is defined as a muscular disease in which the muscle fibers do not function for any one of many reasons, resulting in muscular weakness. “Myopathy” simply means muscle disease (myo= “muscle” + pathos/pathy=”suffering”) as opposed to a condition describing diseases involving the nerves, called neuropathies. The inflammatory myopathies are a group of diseases that involve chronic muscle inflammation, accompanied by muscle weakness. Another word for chronic inflammation of muscle tissue is myositis.
Myositis is the term for any one of a group of inflammatory muscle disorders. It is a chronic inflammatory disease of the muscles in the body and a type of mixed connective tissue disease. These almost always cause weakness and may also cause muscle swelling and pain. Myositis can be caused by a number of things such as injury, infection or in combination with an autoimmune disease such as lupus. It may also be caused by some drugs used in treating SLE. It is unclear how many with lupus also may have myositis, but estimates range from 8% to perhaps many more.
There are three primary kinds of myopathies that are associated with lupus:
Polymyositis (PM): This is the direct attack of the immunie system on muscle fibers. This causes muscle weakness that most typically occurs in the muscles closest to the trunk of the body so that sitting up or lifting with the the middle of the body becomes difficult.
Dermatomyositis (DM): This type of myositis causes the muscle weakness of polymyositis plus a skin rash. It is often characterized with areas of slightly raised reddish, scaly rash. The rash can be on the bridge of the nose, around the eyes, or on sun-exposed areas of the neck and chest. This rash often becomes visible before, in combination with or after progressive muscle weakness. Read more about the rash in the “signs and symptoms” section below.  Amyopathic dermatomyositis is when patients present with a rash but show no sign of muscle disease.
Amyopathic dermatomyositis is when patients present with a rash but show no sign of muscle disease.
Inclusion body myositis (IBM): This type is characterized by progressive muscle weakness and atrophy (or wasting away of the muscle tissue). The onset of muscle weakness is generally gradual (over months or years) and affects both those muscles close to the trunk and those of the extremities. Muscle weakness may affect only one side of the body. Falling and tripping are usually the first noticeable symptoms of IBM. The disorder may begin with weakness in the fingers and wrists that may cause difficulty with buttoning, pinching, and gripping objects. There may be weakness of the wrist and finger muscles and of the forearm muscles and quadriceps muscles. Approximately half of those with IBM will experience difficulty in swallowing. Back to top
What are the signs and symptoms?
The most common symptoms of myositis are weakness in the muscles and rash with muscle weakness in dermatomyositis.
Symptoms in the Muscles:
- General feeling of weakness in the muscles closest to the trunk of the body. This muscle weakness usually starts in your neck, arms, or hips and can be felt on both sides of your body. This weakness may get worse over weeks or months. If you experience sudden or progressive weakness in muscles in neck, hip, back and shoulder muscles, please see your physician as soon as possible.
- Occasionally, the muscles may ache and be tender to touch.
- If the disease progresses, it could eventually cause difficulty for patients when lifting objects, rising from a sitting position, climbing stairs, or reaching overhead.
- Tripping or falling
- Some patients may experience fatigue after walking or standing.
- In some cases, muscles not close to the trunk of the body (distal) could be affected later in the course of the disease. This might include the forearms and around the ankles and wrists.
- Muscle pain
Symptoms of the Rash Associated with Dermatomyositis:
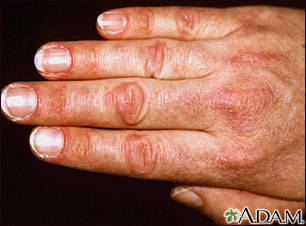 Most commonly in DM, the skin rash will occur on the face, chest, nails, knuckles or elbows. The rash often looks patchy and red or purple in color. It and will also typically develop on the eyelids and other muscles that are used to straight/bend joints, this includes the knees and toes. The inflammation of blood vessels under the skin (also called vasculitis) and in the muscles can cause the rash to be painful and/or itchy.
Most commonly in DM, the skin rash will occur on the face, chest, nails, knuckles or elbows. The rash often looks patchy and red or purple in color. It and will also typically develop on the eyelids and other muscles that are used to straight/bend joints, this includes the knees and toes. The inflammation of blood vessels under the skin (also called vasculitis) and in the muscles can cause the rash to be painful and/or itchy.- Some patients develop hardened bumps of calcium deposits under the skin called calcinosis. This begins to occur most often 1-3 years after the onset of the disease and is more common in children with DM.
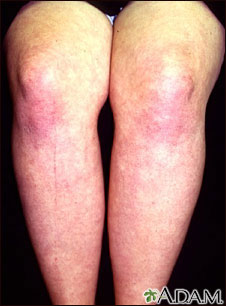 These red rashes can also occur on the face, neck, shoulders, back, upper chest and elsewhere. These areas may also be swelling in the affected areas.
These red rashes can also occur on the face, neck, shoulders, back, upper chest and elsewhere. These areas may also be swelling in the affected areas.- Scaly, dry or rough skin that may even resemble a sunburn
- Swollen and inflamed area around the fingernails
- There may be inflammation of the fat lying just underneath the skin. This is called panniculitis, and can cause tenderness and feeling like little bumps.
Other Related Symptoms and Possible Complications with Myositis:
- Fatigue
- General discomfort
- Weight loss
- Low-grade fever
- Trouble swallowing (dysphagia) which can make it feel like you are choking.
- Breathing difficulties may occur.
- Inflammation of the lungs which causes coughing and shortness of breath.
- Sensitivity to light which can be seen if the rash gets worse with UV (ultraviolet) exposure. This is called photosensitivity.
- Voice changes (dysphonia), especially hoarseness
- Pain in the joints with or without true arthritis (joint inflammation) can be part of myositis.
- Inflammation of the blood vessels of the intestinal tract, eyes and kidneys, and these organs can be damaged by inflammation in patients with myositis.
- Inflammation of the heart muscle tissue and constriction of the blood vessels around the heart can lead to cardiac complications.
- Ulcers
How is it diagnosed?
 A doctor may suspect myopathy when the patient complains of muscle weakness, describes difficulty in completing tasks that require muscle strength, or when they get certain rashes or have breathing problems. If myopathy is suspected, your physician will first take a careful medical and family history and complete a physical exam to document the pattern of muscle weakness that you are experiencing. This will most likely be followed by lab testing and even a muscle/skin biopsy to diagnose myositis and/or dermatomyositis. These tests are used not only to diagnose myopathy, but to rule out disorders that may mimic the symptoms of inflammatory myopathies.
A doctor may suspect myopathy when the patient complains of muscle weakness, describes difficulty in completing tasks that require muscle strength, or when they get certain rashes or have breathing problems. If myopathy is suspected, your physician will first take a careful medical and family history and complete a physical exam to document the pattern of muscle weakness that you are experiencing. This will most likely be followed by lab testing and even a muscle/skin biopsy to diagnose myositis and/or dermatomyositis. These tests are used not only to diagnose myopathy, but to rule out disorders that may mimic the symptoms of inflammatory myopathies.
Some labs and tests that might be ordered are:
- Muscle weakness test: As mentioned earlier in this blog, most people with myopathy have little or no pain in their muscles. This differs from other health problems such as other forms of muscle disease, arthritis related joint pain, numbness or tingling in the hands and feet caused by nerve problems. It is, in fact, very common for many people that have other illnesses to think that they feel weak when they are actually depressed, tired, having shortness of breath rather than having true muscle weakness. The doctor will perform some muscle strength tests to make this differentiation and determine whether true muscle weakness is present.
- A blood test to measure the level of various muscle enzymes: Creatine kinase(CK) is an enzyme that leaks out of muscle fibers when the fibers are being damaged. In DM, the CK level is usually very high.
- An electromyogram (EMG): This test is used to gauge electrical activity in muscle. In this test, tiny needles are inserted into the muscles to test their electrical activity both when at rest and when the person tries to contract the muscle. Inflammatory myopathies will show a distinctive pattern of electrical activity that can help differentiate them from other types of muscle disease.
- Magnetic Resonance Imaging (MRI): This test is used to show any abnormalities in the muscles.
- Blood test for myositis-related antibodies (immune proteins): This test helps detect myopathy and may also provide some information about the prognosis (how serious the disease is).
- Muscle biopsy: In this test, a small piece of muscle tissue is removed for testing to determine the type of myositis present. In one study, biopsies revealed muscle cell damage in many individuals with lupus that did not show clinical symptoms. This suggests that muscle damage is happening to a greater degree than often appreciated.
- Skin biopsy: A skin sample will show changes caused by the disease that may help the diagnosis.
Understandably, DM is the easiest type of myositis to diagnose because of the visible rash that is associated with it. A physician will rule out any other causes for the rash before making a diagnosis of myositis. Back to top
How is it treated?
There is no cure for dermatomyositis, but the symptoms can be treated. Some treatment options may include: 
Medications: The standard treatment for dermatomyositis and polymyositis is a corticosteroid drug such as prednisone either administered in pill form or IV (intravenously). Immunosuppressant drugs such as Methotrexate, azathioprine, tacrolimus, and cyclosporine may be given to those who do not respond well to prednisone. These medications are also commonly used to treat and manage lupus symptoms as well. A drug called intravenous immunoglobulin (IVIG) was recently shown to be effective and safe in the treatment of the disease. It uses healthy antibodies to block the attacking antibodies you are producing that target your skin and muscles and consists of a mixture of antibodies that have been collected from thousands of healthy people who have donated their blood. These treatments don’t last very long, and it’s likely you’ll need a new infusion every six to eight weeks.
For those with DM, a topical corticosteroid ointment or crème may be prescribed to help reduce the appearance and severity of the skin disorder associated with this type of myositis. Learning about photosensitivity may also be of help to those with DM. Antimalarial medications like Plaquenil might be prescribed for a persistent rash. Corticosteroids lower the response of your immune system. This reduces the amount of inflammation-causing antibodies. Your doctor will most likely start you on a high dose of corticosteroids and then slowly lower the amount over a few weeks. This is called tapering down.
Physical therapy: This can help preserve muscle function, assist those with muscle atrophy or help regain strength and range of movement that has been lost 
Exercise: Mobility, flexibility and mood can all be positively affected by getting regular gentle exercise such as yoga, swimming, walking, etc.
Surgical intervention: For those with calcium deposits that cause nerve pain and/or recurring infections, surgery may be required to remove the deposits.
Heat therapy: This can including microwave and ultrasound therapies.
Orthotics and assistive devices: These can help you accomplish everyday activities that have become difficult due to muscle weakness.
Rest: Taking care to get the proper rest when living with any illness is very important Most cases of dermatomyositis respond well to therapy and are considered highly treatable. Some patients may recover completely while others may have very long periods with little or no disease activity. It may take several years of treatment to suppress the immune system for this to take place. The disease is usually more severe and resistant to therapy in patients with associated cardiac or pulmonary problems. For those who do not recover, a low dose of continued immune suppressing medication may be required throughout their lives. Back to top
What causes myositis?
The exact cause of these conditions isn’t known although they are thought to be immune disorders. However, there are some suspected links. Here are a few of the possible causes being further examined:
- Autoimmune disorders: Similarities between myopathies and autoimmune diseases like systemic lupus erythematosus (SLE) have caused doctors to believe that there may be a link between the two. Autoimmune diseases occur when the body’s disease-fighting cells (called antibodies) attack healthy cells. A compromised immune system may also contribute to the development of dermatomyositis.
- Exposure to a toxic substance or medicine: Some of the drugs that have been suspected of contributing to myositis are interferon-alpha (mostly used to treat cancer and hepatitis), penicillamine (a drug used to lower copper levels in the body), carticaine (a local anesthetic), cimetidine (used to treat ulcers), carbimazole (to treat thyroid disease), phenytoin (used to treat seizures) and growth hormone. The vaccine for hepatitis B also has been implicated in some cases.
Importantly, the chronic use of high-dose corticosteroids (exceeding 40-60 mg/day) has been associated with certain myopathies. Some patients who increased dosages to these levels were seen to have clinically significant muscle weakness within two weeks.
- Other diseases such as cancer or rheumatic conditions, or a virus (such as HIV, Coxsackie B, or HTLV-1) or other infectious agent.
Unfortunately, in the majority of cases, there is no clear cause for the development of myositis. Back to top
Who gets myositis?
These rare disorders may affect both adults and children of any age or sex. Polymyositis and dermatomyositis are more common in women than in men. Although anyone can develop dermatomyositis, it is most common in adults between the ages of 40 and 60 and children between the ages of 5 and 15. Dermatomyositis is becoming more prevalent in African-American women for reasons that are not yet understood. Back to top
What is the prognosis for someone with myositis?
In dermatomyositis, most cases and symptoms respond very well to therapy. In DM, permanent loss of strength and muscle atrophy sometimes occurs, but in other cases, full strength and muscle size are recovered. In individuals with cardiac or pulmonary problems, the disease is usually more severe and resistant to therapy. In polymyositis, the prognosis varies. Some patients have a more severe form of the disease, do not respond well to therapies, and are left with significant disability, but most patients respond fairly well to the available treatment options. For those who have difficulty swallowing, malnourishment can be a concern. Because falls and tripping can be common in those with myositis, it is important to be very careful to avoid falling injuries that can lead to fractures, disability or even death. In rare cases people with severe and progressive muscle weakness can have pneumonia or even respiratory failure. IBM is generally resistant to all therapies and its rate of progression appears to be unaffected by currently available treatments. As with most autoimmune diseases, earlier diagnosis and treatment greatly increase the chances for achieving the best possible outcome and avoiding more serious complications. Back to top
In conclusion
A diagnosis of myositis may feel overwhelming, but it doesn’t have to be. It is a complex disease and the symptoms and severity can vary widely between those diagnosed, depending on which type of myositis is diagnosed as well as which overlapping diseases and symptoms are involved. Understanding and educating yourself is the first step in regaining a feeling of control, thus calming some of the natural concerns that come with any diagnosis. There are many feelings that go along with learning to cope with a chronic illness and they are all normal. You may not know where to turn to for advice, support, or information. Your family, friends, and caregivers may feel the same way. The first thing to understand is that a person with myositis, lupus, fibromyalgia, or any other chronic illness is just that. A person. The disease should not become your identity. There is so much more to you than your diagnosis, so maintaining a [positive but realistic attitude], and understanding the mind/body connection can really help when learning to live with any chronic disease. Lead as full of a life as possible and understand that this is just a part of your life, meaning that the disease is what you have, not who you are. If you are feeling depressed or hopeless, or having trouble accepting your diagnosis, please seek counseling from a professional to help provide the tools to support you in coping with these complicated feelings. If you or someone you care about is showing any of the above signs or symptoms, getting a quick, accurate diagnosis and early treatment, can help to minimize the symptoms of myositis, decrease the chances of irreversible damage, and create the best possible outcome and quality of life.
References
Dalakas, M. C. (2020). Inflammatory myopathies: update on diagnosis, pathogenesis and therapies, and COVID-19-related implications. Acta Myologica, 39(4) 289-301. https://doi. org/10.36185/2532-1900-032
Inflammatory myopathies fact sheet. (2020, January). National institute of neurological disorders and strokes. Retrieved March 11, 2021, from https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Inflammatory-Myopathies-Fact-Sheet
Jakati, S., Rajasekhar, L., Uppin, M., & Challa, S. (2015). SLE myopathy: A clinicopathological study. International Journal of Rheumatic Diseases, 18(8), 886-891. https://doi-org.proxy.lib.pdx.edu/10.1111/1756-185X.12592
Myopathy. (n.d.) Cedars sinai. Retrieved March 11, 2021, from https://www.cedars-sinai.org/health-library/diseases-and-conditions/m/myopathy.html
Myositis. (2015, April 17). MedlinePlus. Retrieved March 11, 2021, from https://medlineplus.gov/myositis.html
Silver, E. M, & Ochoa, W. (2018). Glucocorticoid-induced myopathy in a patient with systemic lupus erythematosis (SLE): A case report and review of the literature. The American Journal of Case Reports, 2018(19) 277-283. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5865408/
Author: KFL Team
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.


