Lupus and the Nervous System
- Introduction: The Two-minute Overview
- The Nervous System: Another Overview
- Lupus and the Nervous System
- In Conclusion
Introduction: The Two-minute Overview
Lupus can attack the nervous system as easily as it can attack the joints, kidneys, skin or any other part of the body. Studies have found that up to 90% of all lupus patients will experience some type of nervous system symptoms. These symptoms can be very subtle, diffuse and difficult to diagnose … or they can be devastating and dramatically affect quality of life. These symptoms can include:
- Cognitive issues, like confusion, cloudy thinking, brain fog and problems with memory;
- Headaches, especially migraine-like pain that may not be helped by pain relievers;
- Body pain or even fibromyalgia;
- Increased sensitivity to touch or other senses;
- Strokes and seizures;
- Depression or even psychosis.
Just as diverse as many of these symptoms can be – they can be very difficult to diagnose as the results of lupus rather than from other causes. Lupus can either directly attack the nervous system with autoantibodies, or it can indirectly cause symptoms from systemic inflammation and the micro-clotting of the blood vessels that nourish parts of the nervous system.
Because many of these symptoms can be caused by conditions other than lupus, it may take several tests and referrals to a specialist, such as a neurologist, to confirm the diagnosis.
Treatments also can vary, depending upon the actual diagnosis. However, maintaining a treatment plan that limits inflammation, autoantibodies and the risk of lupus flares is a good baseline. Specific therapies that protect the nerves themselves may be necessary. Of course, if depression and anxiety are a problem, mental health therapy may also help.
Want to learn more? Read on to get the specifics!
The Nervous System: Another Overview
The nervous system is by far the most complex and least understood part of the human body. It’s job is to:
- Regulate things like body temperature, breathing rate and more;
- Coordinate muscular movements like eye-hand coordination;
- Send signals from one part of the body to another;
- Sense things like vision, hearing, taste, smell, touch, pain, etc., and
- Integrate the higher functions of thinking, learning, emotions and memory.
.
The nervous system is divided into two parts: the Central Nervous System and the Peripheral Nervous System.
The Central Nervous System:
The central nervous system (CNS) is made up of the brain and the spinal cord. It not only is responsible for the mental functions of the mind, like thinking, emotions and sensations, but also controls or regulates many other functions of the body – like muscle movements, breathing, body temperature, digestion and much more.
There is definitely heated debate about the numbers, even today, but on average the brain contains around a 100 billion nerve cells or “neurons” and about a 100 billion support cells called “glial cells.”
Neurons are the “working units” of the brain and spinal cord and they do most of what we call the actual functions of the nervous system. Individually, each neuron basically takes information from the senses or other neurons and transmits them to another neuron. That seems pretty simple. However, each neuron (on average) is connected to at least 10,000 other neurons (sometimes and each neuron can “decide” whether to transmit this information or not.
What does that mean? Multiply over one hundred billion nerve cells that are each connected to at least ten thousand other nerve cells and that means that there are may be 100 to 1,000 trillion connections, or synapses, that work to perceive, remember, regulate, feel, think or create thousands of things per second! That is thousands of times more than the stars in the Milky Way galaxy.
This is why most scientists feel that the human brain is the most complex 3-pound “thing” in the universe!
So, what about those 100 billion glial cells? The glial cells support the neurons with water, nutrients, oxygen – everything they need to operate effectively. Glial cells even clean up brain debris, help hold neurons in place and digest parts of dead neurons. There are new studies finding more about the glial cells all the time, but the fact is that at least half of your brain isn’t involved in thinking at all!
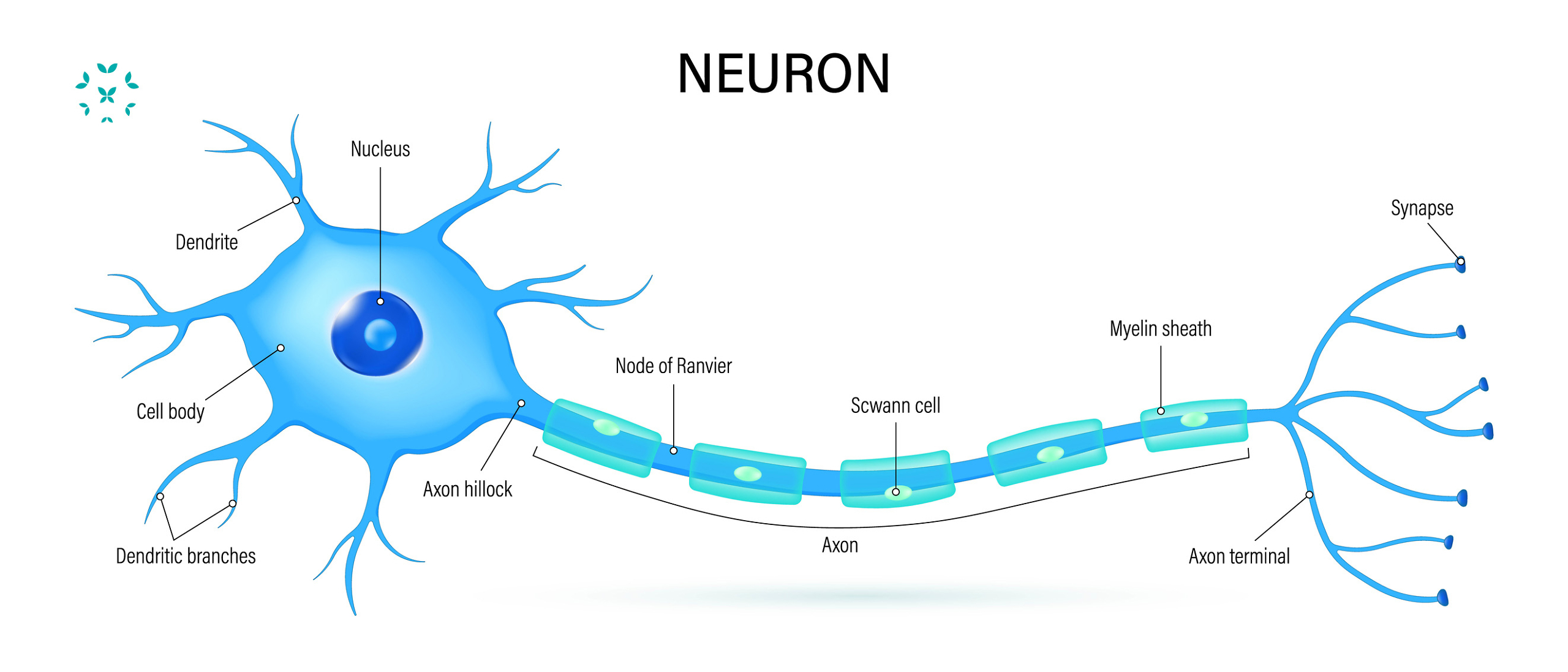
The Peripheral Nervous System:
The peripheral nervous system (PNS) consists of all the nerves outside of the brain and spinal cord to the rest of the body. These include the sensory neurons and motor neurons. The sensory neurons gather information from the outside environment, such as touch, sound, light and all other stimuli, while the motor neurons control how muscles move and glands function.
The motor side of the PNS also has the autonomic nervous system. This part controls the involuntary aspects of the body, such as digestion, heart rate, pupil size and secretions of glands like the adrenals and sweat glands.
So what does this all this mean for someone with lupus? Read on to explore some of the most common nervous system issues associated with lupus and find advice on how to help with those symptoms that can “get on your nerves.”
.
Lupus and the Nervous System:
Lupus can affect pretty much any part of the nervous system – and that means it can affect everything from thinking, sensing, regulating digestion, controlling muscle movements or governing emotions.
How? Broadly speaking in two ways:
- Autoantibodies or inflammatory chemicals directly affecting neurons themselves, or
- Autoantibodies or inflammatory chemicals damaging the blood vessels or other organs that support those neurons.

What are the major effects of lupus on the nervous system?
Cognitive Dysfunction: This is the most common problem related to the CNS and lupus. It includes cloudy thinking, lupus fog, memory loss/impairment and confusion.
It is believed that 80 percent of lupus individuals who have had the disease for ten years or more will experience some facet of cognitive dysfunction. Scientists feel that this disruption is attributed to a decrease in oxygen delivery to certain parts of the brain.
Unfortunately, there is no definitive treatment for these problems at this time. However, reducing overall inflammation and limiting the autoimmune response is always important. Additionally, some individuals have found relief through cognitive therapy or medications to increase concentration. A diet high in fruits and vegetables, nuts and seeds (particularly walnuts), olive oil and turmeric may help cognitive function as well.
.
Migraines: Around 20 percent of people with lupus will experience migraines. It is important to understand and avoid the triggers for lupus headaches. UV lights, lack of sleep, food sensitivities, dehydration, stress, hormone changes, alcohol, weather changes and caffeine dependency are all common migraine triggers.
There are many different medications out there to help alleviate migraine symptoms. They are broken down into two different categories: preventative and abortive/acute.
Preventative medications include:
- Cardiovascular, beta-blocker drugs (like Propranolol);
- Antidepressants (like Nortriptyline), and
- Anti-seizure medications (like Topamax).
Acute symptom relieving medications include:
- NSAIDS;
- Triptans, like Imitrex and Zomig, and
- Ergots or caffeine combo drugs, like Migergot.
Alternative therapies like acupuncture and yoga have been known to give some migraine sufferers relief as well.
Note: It is critically important to talk with healthcare providers before making any changes to your medications!..
.
Central Nervous System Vasculitis: CNS vasculitis involves inflammation of the blood vessels in the brain or spine. It usually occurs when abnormal antibodies attack the white blood cells, and the walls of the blood vessels become inflamed, often resulting swelling. Sometimes infections or virus can cause this as well.
Symptoms of CNS vasculitis can be seizures, mental fuzziness or confusion, abnormal sensations or even stroke. It is diagnosed by a blood vessel study (brain MRA or CT-angiogram) and is most often treated with high-dose steroids such as prednisone, in combination with immunosuppressants.
.
Fibromyalgia: Fibromyalgia is a condition that is categorized by chronic widespread pain and heightened sensitivity to touch. This sensitivity appears to stem from a neurochemical imbalance with pain-processing. Many advances have been made in acknowledging the disease and the physical impacts it has on the individual.
Anti-seizure medications like Lyrica have been introduced to help with pain management and studies have shown that regular exercise increases the body’s production of endorphins, which are natural painkillers and mood boosters...
Organic Brain Syndrome (OBS): Sometimes called cerebritis or encephalopathy, OBS is sometimes confused with dementia, but is a general term that describes a decreased mental function and state due to a medical condition. Brain injury from trauma, breathing disorders, poor cardiovascular health, and degenerative conditions like Alzheimer’s or multiple sclerosis can also cause OBS.
Diagnosis may require a lumbar puncture or EEG brain wave study. Treatment depends on the origin of the problem, but often include high doses of steroids. Supportive care and rehabilitation to assist where brain function is lost, as well as medications to reduce any behavioral issues may be helpful.
Central Nervous System Lupus: This can be caused by lupus directly leading to increase of inflammation of the central nervous system and the resulting swelling. It is an illness that can be serious. but is treatable. It can range from mild cognitive dysfunction to major issues, like stroke, seizure or coma.
The standard treatment for the CNS Lupus is immunosuppression with corticosteroids and symptom management.
.
Note: It is also important to note that 20% of those who take steroids can also develop some of the symptoms of lupus on the nervous system as side effects, including headaches, mood changes and difficulty concentrating. This can make it difficult to differentiate between symptoms cause by lupus and those caused by steroid medications.

In Conclusion:
The complexity of the nervous system, especially the brain, is almost too much to contemplate. Though, occasionally, inflammation of the brain and nervous system can lead to conditions like the ones listed above, serious complications are rare. And with some basic knowledge of what to expect, and with the recent advances in diagnostic tests and treatments, people living with neurological disorders associated with lupus can live well-balanced and long lives!
So, don’t be “nervous;” you are not alone!
For more information on neuropsychological lupus, check out this KFL blog article, “Neuropsychiatric Lupus.”
References
Hunt, D. (2023). The nervous system. In Thomas, D. (Ed.), The lupus encyclopedia (2nd ed.) (pp. 262–301). Johns Hopkins Press.
Kirou, K.A., & Ruiz, R. (2023, June 14). Neuropsychiatric lupus – Lupus and the brain. Hospital for Special Surgery. https://www.hss.edu/conditions_neuropsychiatric-sle-lupus-and-brain.asp
Nervous System. (n.d.). Johns Hopkins Lupus Center. https://www.hopkinslupus.org/lupus-info/lupus-affects-body/lupus-nervous-system/
Ota, Y., Srinivasan, A., Capizzano, A.A., Bapuraj, J.R., Kim, J., Kurokawa, R., Bab, A., & Moritani, T. (2022). Central nervous system systemic lupus erythematosus: Pathophysiologic, clinical and imaging features. RadioGraphics 41(1), 212-232. https://doi.org/10.1148/rg.210045
Von Bartheld, C. S., Bahney, J., & Herculano-Houzel, S. (2016). The search for true numbers of neurons and glial cells in the human brain: A review of 150 years of cell counting. The Journal of comparative neurology, 524(18), 3865–3895. https://doi.org/10.1002/cne.24040
Wallace, D. (1995). Heady connections: The nervous system and behavioral changes. The lupus book: A guide for patients and their families (1st ed.) (pp. 99-115). Oxford University Press.
Author: Kaleidoscope Fighting Lupus Staff (updated 2023)
All images unless otherwise noted are property of and were created by Kaleidoscope Fighting Lupus. To use one of these images, please contact us at [email protected] for written permission; image credit and link-back must be given to Kaleidoscope Fighting Lupus.
All resources provided by us are for informational purposes only and should be used as a guide or for supplemental information, not to replace the advice of a medical professional. The personal views expressed here do not necessarily encompass the views of the organization, but the information has been vetted as a relevant resource. We encourage you to be your strongest advocate and always contact your healthcare practitioner with any specific questions or concerns.